Dinner is not a reward at the end of a high-output day — it is a physiological intervention with measurable consequences for the next 24 hours of performance. For executives and founders operating under chronic cognitive and metabolic load, the composition of healthy meals for dinner directly influences overnight cortisol clearance, fasting insulin sensitivity, and the depth of slow-wave sleep essential for prefrontal cortex restoration. Suboptimal dinner choices accelerate biological age markers detectable in inflammatory cytokine panels, compounding over years into cardiovascular risk profiles inconsistent with long-term leadership capacity. What follows is structured for professionals who understand that nutritional precision at dinner is a non-negotiable pillar of sustained high performance.
The Metabolic Window Nobody Talks About
The hours between 6 p.m. and midnight matter more than most professionals realize. This is not about caloric volume. Instead, it is about hormonal context.
As the body shifts toward rest, metabolic rate slows and insulin sensitivity drops. The liver also moves from glucose production toward fat processing. Eating late — especially large, refined-carb meals — therefore produces a different outcome than the same meal eaten at noon.
Research published in Cell Metabolism found that identical calories consumed later in the day produced greater fat storage. This also disrupted hunger signaling. Both effects occurred even when total energy intake stayed the same.
READ ALSO: 10 Best Foods to Fight Aging
Circadian Biology and the Evening Meal

The brain's master clock sends timing signals to every organ involved in digestion and energy use. The pancreas, liver, and fat tissue all run on time-sensitive circadian programs. Eating in line with these programs supports normal overnight insulin control.
When the pancreas repeatedly activates late at night, however, fasting insulin rises over time. This slow drift then speeds up biological aging. As a result, finishing dinner before 8 p.m. works with this biology rather than against it.
Dinner that is full in nutrients but not excessive in calories is the practical target. It does not require extreme restriction. It simply requires awareness of timing and composition.
READ ALSO: Natural Superfoods for Energy: Fuel Your Day the Right Way
Inflammatory Load and Food Selection

Chronic low-grade inflammation drives heart disease, brain decline, and faster biological aging. The Harvard T.H. Chan School of Public Health has documented the link between diet and key inflammatory markers. These include C-reactive protein and interleukin-6.
Dinner choices that bring in pro-inflammatory compounds raise these markers over time. Ultra-processed ingredients, refined seed oils, and high-fructose corn syrup are common sources. Moreover, the effect shows up in standard blood panels long before symptoms appear.
In contrast, meals built around oily fish, cruciferous vegetables, olive oil, and polyphenol-dense plant foods reduce these markers. For executives already managing high stress loads, cortisol itself elevates baseline inflammation. The anti-inflammatory quality of dinner is therefore not a secondary concern — it is a direct lever on systemic inflammatory burden.
READ ALSO: Superfoods for Energy and Well-Being: Power Up Naturally
Glycemic Architecture and Sleep Quality

The link between post-dinner blood glucose and sleep quality is direct. A high-glycemic dinner spikes glucose fast. The resulting insulin surge can then trigger a glucose drop in the early hours of sleep.
This drop activates the stress response and raises cortisol. It also breaks up the deep sleep stages where the body releases growth hormone and the brain locks in memory. For a professional whose performance depends on clear thinking and emotional control, this is a direct nightly cost.
Low-glycemic dinners — built around legumes, non-starchy vegetables, and whole grains — produce a flatter glucose curve. As a result, sleep is less likely to break apart. Over time, this structural shift in dinner composition supports both sleep quality and next-day cognitive output.
READ ALSO: Peruvian Diet and Nourishing Foods for Balanced Energy
The Role of Fiber in Overnight Metabolic Function
Fiber consumed at dinner has effects that extend well into the next morning. Gut bacteria break down soluble fiber overnight into short-chain fatty acids. These compounds then reduce inflammation and support gut barrier strength.
They also improve next-morning insulin sensitivity through the gut-liver connection. This means the quality of tomorrow's metabolic function is partly determined by tonight's dinner. The relationship is direct and well-supported by research.
The Nurses' Health Study and Health Professionals Follow-Up Study, both run through Harvard, found clear links between higher fiber intake and lower rates of heart disease and type 2 diabetes. They also found links to lower rates of early death. Dinner built around lentils, chickpeas, leafy greens, and root vegetables is therefore both a digestive strategy and a direct investment in next-day metabolic health.
READ ALSO: Foods to Avoid Eating with Acid Reflux for Daily Comfort
Fat Quality and Cardiovascular Risk
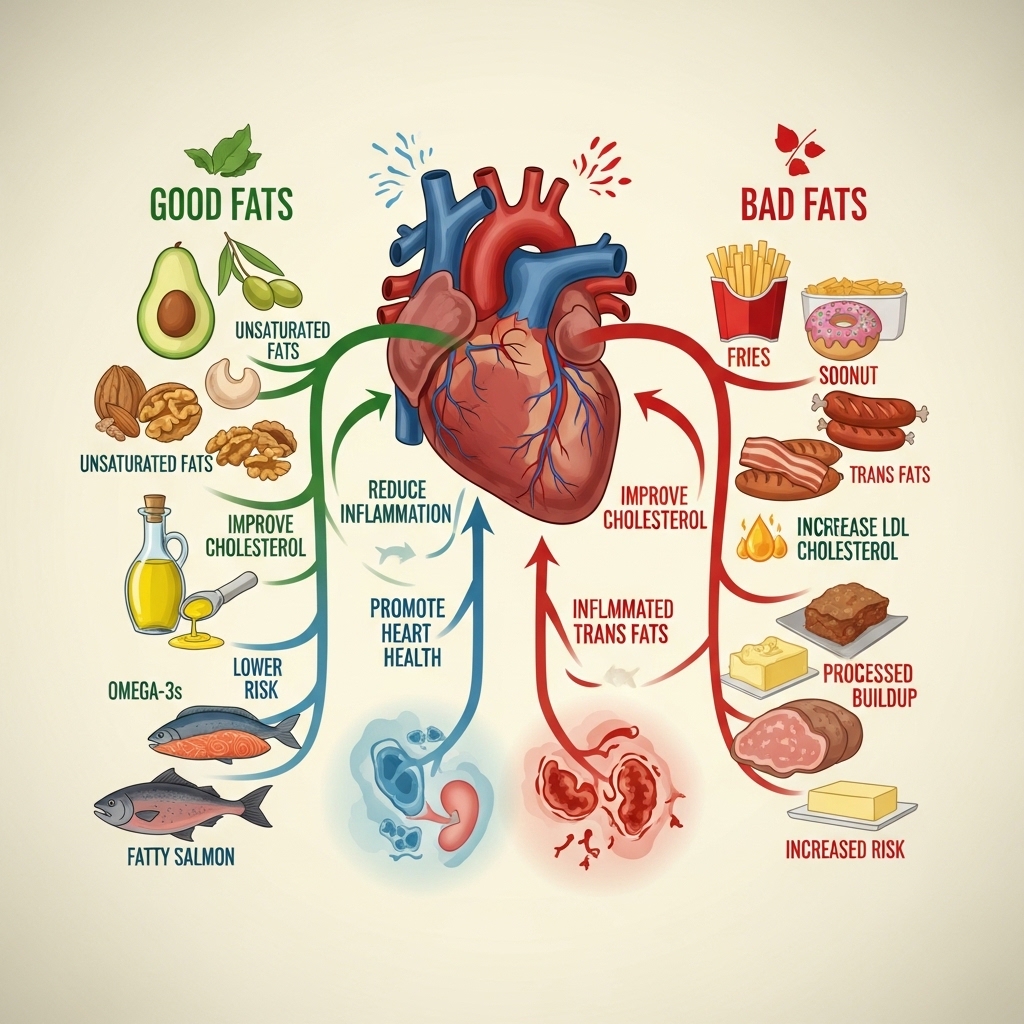
Not all fat at dinner carries the same cardiovascular outcome. Saturated fat from ultra-processed sources raises harmful cholesterol and drives arterial inflammation. Eaten regularly, this therefore contributes to plaque buildup over time.
Monounsaturated fats from olive oil and avocado produce measurably better effects on cholesterol and arterial health. So do omega-3 fats from oily fish. These fat sources actively support the cardiovascular system rather than placing additional burden on it.
The PREDIMED trial, published in the New England Journal of Medicine, found that a Mediterranean-style diet with extra virgin olive oil or nuts significantly cut the rate of major cardiovascular events. This finding is directly relevant for professionals in their forties and fifties. Many professionals in this age group already carry hidden cardiovascular disease, making fat quality at dinner a matter of clinical relevance rather than general preference.
READ ALSO: Jamaican Diet: Energizing Foods for a Restful Life
Cognitive Performance and the Dinner-to-Morning Pipeline

The evening meal is the starting point in a chain that ends with next-morning cognitive output. Deep sleep and REM sleep both depend on stable overnight glucose and low inflammation. These are the stages where the brain locks in memory and clears out waste — including amyloid-beta.
The brain also strengthens neural connections during this time. Disrupting these processes through poor dinner choices does not, therefore, just cause fatigue. It also reduces processing speed and weakens working memory.
Executive function during high-stakes decisions suffers as well. For professionals whose competitive edge is cognitive, this is not a peripheral concern. The dinner plate is consequently a direct performance tool with measurable downstream effects on next-day output.
READ ALSO: The 2026 Guide to a Healthy Grocery List (and Actually Saving Money)
Meal Timing, Overnight Fasting, and Metabolic Repair

Finishing dinner earlier extends the overnight fasting window. It does this without requiring breakfast to be skipped. This creates more time for cell recycling, glycogen use, and fat-based fuel production.
Research in Cell Metabolism on time-restricted eating showed gains in insulin sensitivity and blood pressure. Cellular stress markers also improved. These gains occurred even without cutting total calories, which makes timing itself an independent variable worth managing.
For professionals managing travel or irregular schedules, anchoring dinner timing is therefore one of the most accessible levers for metabolic consistency. It does not require a change in food choices. It requires only a shift in when those choices happen.
READ ALSO: Healthy Protein Snacks for Pizza Cravings That Protect Metabolic Function and Biological Age
Hydration, Electrolyte Balance, and Dinner Composition

Hydration status at dinner affects both digestion and overnight heart function. High-sodium processed meals raise blood pressure quickly. Over time, repeated exposure then leads to stiffer arteries and higher cardiovascular risk.
Potassium-rich whole foods — leafy greens, white beans, wild salmon — support healthy blood vessel tone and heart rhythm. They work in direct balance with sodium to regulate fluid and pressure across the cardiovascular system. Including them at dinner is therefore a practical and evidence-supported strategy.
Similarly, magnesium plays a well-documented role in sleep onset, cortisol control, and muscle relaxation. Chronic stress depletes it, and processed food patterns rarely replace it. Dinners built around dark leafy greens, pumpkin seeds, and legumes provide a meaningful dietary source without the need for supplementation.
READ ALSO: 5 Healthy Snack Recipes Perfect for Mid-Day Cravings to Energize You
Alcohol at Dinner and the Performance Cost

Routine alcohol with dinner carries a specific cost for high performers. Moderate red wine is often cited for heart benefits. The actual dose of active compounds in a single glass, however, is too small to produce a meaningful clinical effect.
The sleep disruption, by contrast, is not small. Even one to two drinks suppresses REM sleep and raises overnight heart rate. It also reduces heart rate variability and breaks up deep sleep in ways that wearable devices consistently measure.
Professionals using these devices regularly record lower readiness scores after dinners with alcohol. The cost is therefore not mainly to the liver. It is cognitive — occurring nightly, building up over time, and directly affecting the quality of decisions made the following day.
READ ALSO: The Complete Healthy Kitchen – Whole Living Eat Well
Applying the Evidence: Structured Dinner Frameworks

The research across these areas points toward a clear dinner structure rather than a rigid set of rules. Professionals may, for example, build the evening meal around a solid portion of lean protein. Non-starchy vegetables and fiber-rich legumes or whole grains work well alongside it.
Fats from olive oil, avocado, or oily fish round out the plate. Finishing dinner two to three hours before sleep then supports the overnight fasting window. It also reduces late-night glucose swings that disrupt sleep architecture and next-day metabolic function.
Additionally, limiting alcohol on high-priority nights — before key decisions, travel, or recovery periods — produces measurable gains in next-day readiness and cognitive output. These are not extreme steps. They are, instead, the direct application of existing evidence to the demands of professionals who cannot afford to treat dinner as an afterthought.
UP NEXT: Power Foods: Grapefruit – Whole Living Wellness
Consistent consumption of pro-inflammatory, high-glycemic evening meals has been linked to elevated C-reactive protein, accelerated telomere shortening, and a measurable increase in biological age of up to three years compared to those following anti-inflammatory dietary patterns. WholeLiving's Biological Age Estimation Model incorporates this factor directly — your assessment takes under five minutes.
Ready to understand how these factors are influencing your biological age right now? [Take the Biological Age Assessment →]






