Most high-performing professionals accumulate health interventions the same way they accumulate software subscriptions — reactively, incrementally, and without a governing architecture. The result is a fragmented protocol that generates noise rather than signal, and fails to produce the measurable outcomes — reduced inflammatory burden, optimized metabolic function, decelerated biological aging — that a consolidated health plan is designed to deliver. For executives operating under sustained cognitive and physiological demand, fragmentation is not a neutral state. It accelerates allostatic load, creates gaps in recovery, and produces the kind of biological age drift that compounds silently across the fifth and sixth decades of life.
What a Consolidated Health Plan Actually Means

A consolidated health plan is not a wellness checklist. It is a structured, evidence-informed framework that brings together nutrition, recovery, movement, cognitive performance, and biomarker tracking into one governing protocol. Each element connects to and reinforces the others. No pillar operates alone.
For high-performing professionals, this distinction matters clinically. A fragmented approach — where nutrition, sleep, and exercise exist as separate, uncoordinated efforts — creates competing signals in the body. The body cannot optimize for recovery when training load, dietary timing, and sleep are pulling in different directions. A consolidated health plan resolves that conflict by creating coherence across all inputs.
The architecture of consolidation also changes how professionals read data. When health variables sit within a unified framework, patterns become legible. A drop in HRV, a shift in fasting glucose, a change in sleep staging — within a consolidated plan, these are connected signals. In a fragmented protocol, they are isolated data points with no governing context.
The Biological Cost of Fragmented Health Protocols

Fragmented health protocols carry a measurable biological cost. When health interventions lack coordination, the body's regulatory systems — the HPA axis, the autonomic nervous system, the metabolic pathways — receive inconsistent inputs. Over time, that inconsistency raises allostatic load. This is the cumulative physiological burden of adapting to competing and unresolved demands.
Allostatic load is not a theoretical construct. Research from the MacArthur Foundation Research Network on Socioeconomic Status and Health documents it as a measurable composite of biomarkers — including cortisol, inflammatory markers, cardiovascular indicators, and metabolic variables. High allostatic load in midlife consistently predicts faster biological aging, cognitive decline, and cardiovascular risk. For executives aged 35 to 60, it is one of the most consequential and most undermonitored variables in long-term health.
The irony for high-performing professionals is that fragmentation often stems from high engagement, not low engagement. They adopt interventions aggressively — cold exposure, continuous glucose monitoring, high-intensity training. But without a consolidated health plan to sequence and connect these inputs, the net effect is physiological noise rather than physiological gain.
Nutrition as the Foundation of a Consolidated Health Plan

Within any consolidated health plan, nutrition functions as the foundational regulatory layer. Dietary pattern shapes inflammatory burden, metabolic function, hormonal environment, and cognitive performance — often more directly than any other modifiable variable. For this reason, nutritional architecture is not merely a component of the plan. It is the base on which every other component rests.
The Harvard T.H. Chan School of Public Health has published extensively on the relationship between dietary pattern and long-term health outcomes, including cardiovascular risk, metabolic disease, and cognitive aging. Its research consistently shows that dietary quality — measured by adherence to whole food, anti-inflammatory patterns — predicts health trajectory more reliably than any single nutrient intervention. This finding is directly relevant to professionals who approach nutrition through supplementation rather than dietary structure.
A consolidated health plan therefore begins with dietary pattern assessment. It addresses supplementation, timing, and macronutrient targets only after that foundation is in place. The sequencing matters. Layering micronutrient protocols onto a pro-inflammatory dietary baseline adds complexity without addressing root cause. Nutrition consolidation means establishing the dietary base first, then building precision interventions on top of it.
READ ALSO: Body Sensor Network Is The Key to Optimize Your Health
Metabolic Function and the Role of Nutritional Coherence

Metabolic function in midlife professionals is particularly sensitive to nutritional coherence — the degree to which dietary inputs are consistent, well-timed, and aligned with the body's regulatory rhythms. Inconsistent meal timing and erratic macronutrient distribution disrupt insulin sensitivity. They also impair the metabolic flexibility that underpins sustained cognitive and physical performance.
Research published in Cell Metabolism and related journals has examined the relationship between meal timing and metabolic regulation. Alignment between dietary intake and circadian biology significantly influences insulin sensitivity, fat use, and inflammatory status. For professionals whose schedules produce irregular eating patterns, this evidence carries direct practical weight. A consolidated health plan treats timing as a metabolic variable — not merely a logistical one.
Metabolic flexibility — the capacity to shift efficiently between glucose and fat as fuel sources — is a core performance variable for the executive demographic. It determines cognitive stamina, physical endurance, and recovery capacity. A consolidated health plan that addresses dietary pattern, meal timing, and macronutrient distribution in a coordinated way directly supports metabolic flexibility. A fragmented approach frequently undermines it through inconsistent signaling to insulin and glucagon pathways.
Inflammatory Burden and Dietary Architecture
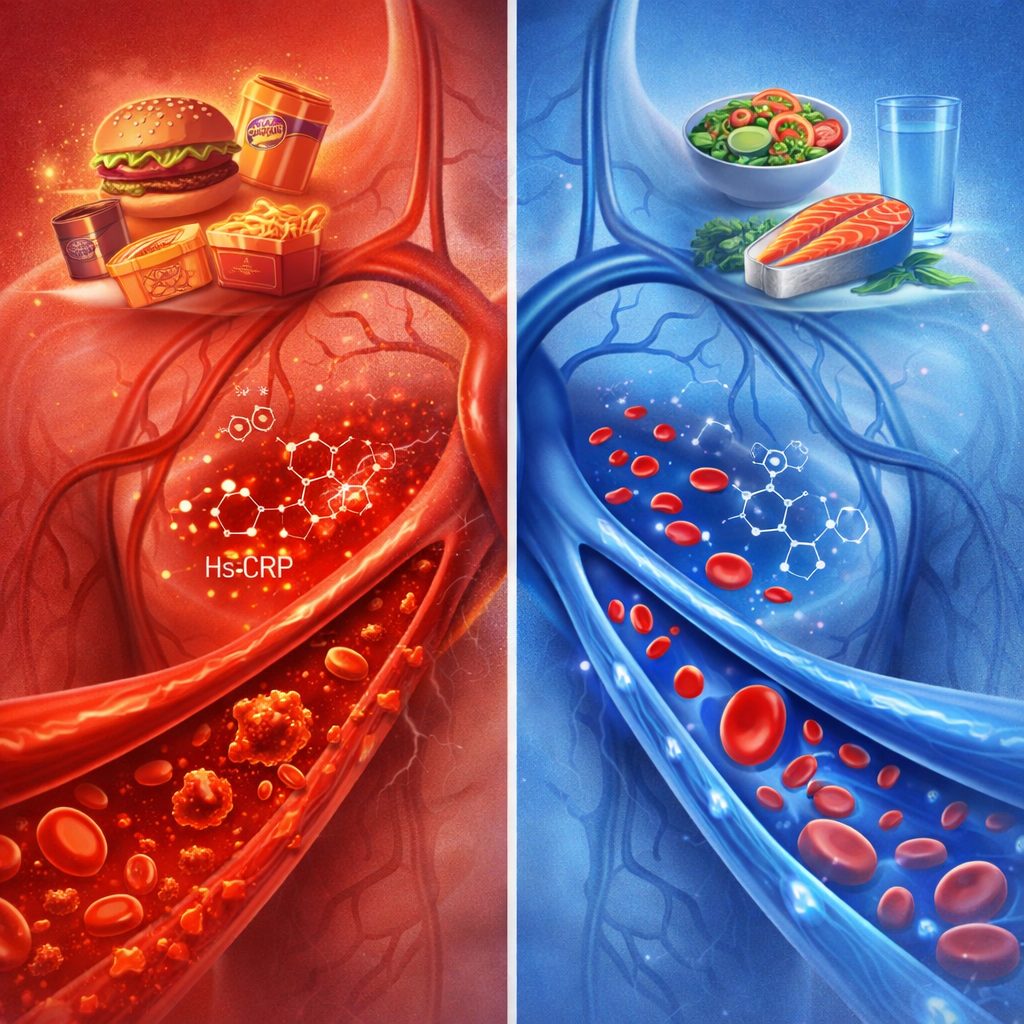
Systemic low-grade inflammation is among the most well-documented drivers of accelerated biological aging and chronic disease risk in the midlife professional demographic. Its primary dietary drivers — refined carbohydrates, industrial seed oils, ultra-processed food, excess alcohol — are well established in the research literature. What receives less clinical attention is the cumulative inflammatory effect of dietary fragmentation itself.
The American Heart Association documents the relationship between dietary pattern and systemic inflammatory markers — including hs-CRP and interleukin-6. Anti-inflammatory dietary patterns measurably reduce cardiovascular risk and support blood vessel function. For executives who monitor inflammatory biomarkers, dietary structure is the most direct lever available for moving those numbers. No supplementation protocol produces an equivalent effect without the dietary foundation in place.
A consolidated health plan addresses inflammatory burden at its source. Rather than targeting individual inflammatory markers with specific supplements, it establishes a dietary pattern that reduces the baseline inflammatory load across all systems. This structural approach produces more durable outcomes than targeted interventions. It addresses the source of the signal rather than the signal itself.
READ ALSO: Detox Living for a Healthier, More Vibrant You
Cognitive Performance and the Gut-Brain Axis

Cognitive performance in high-performing professionals is not solely a function of sleep, stress management, or cognitive training. Emerging research on the gut-brain axis has established a direct two-way communication pathway between the gut microbiome and the central nervous system. Dietary pattern is the primary modifiable driver of microbiome composition. Microbiome composition, in turn, directly influences brain inflammation, neurotransmitter production, and cognitive function.
Research published in Nature Neuroscience and related journals has examined the relationship between gut microbiome diversity, dietary fiber intake, and cognitive outcomes. Diets high in fermentable fiber and low in ultra-processed food support microbiome diversity. They reduce brain inflammatory signaling and associate with better cognitive performance across age groups. For executives whose competitive edge depends on cognitive output, this is a nutritional variable with direct performance consequence.
A consolidated health plan integrates gut health as a cognitive performance variable — not as a digestive health afterthought. Dietary choices are evaluated not only for their macronutrient profile and caloric contribution, but for their prebiotic value and their effect on gut barrier integrity. That level of integration is only achievable within a consolidated framework.
READ ALSO: Precision Nutrition and Hydration for Optimal Health
Sleep Quality and Nutritional Timing

Sleep quality and nutritional timing are more closely connected than most executive health protocols acknowledge. Late caloric intake, high glycemic evening meals, and alcohol consumption — all common in the professional demographic — disrupt sleep architecture. They raise core body temperature, suppress melatonin secretion, and fragment slow-wave sleep. These effects show up in sleep staging data and carry direct consequences for recovery and next-day cognitive performance.
Research in behavioral sleep medicine has established that the timing and composition of evening nutrition significantly influences sleep onset, sleep efficiency, and the proportion of restorative slow-wave sleep achieved. For professionals using wearable sleep tracking devices, nutritional timing is one of the most actionable levers available. A consolidated health plan creates explicit connections between these variables rather than treating them as separate concerns.
Slow-wave sleep is where the body conducts its most intensive physical repair — including protein synthesis, immune regulation, and metabolic waste clearance in the brain. Nutritional choices that protect slow-wave sleep are therefore not simply dietary decisions. They are recovery decisions with consequences for biological aging, immune function, and cognitive longevity. A consolidated health plan makes this connection explicit and operational.
Cardiovascular Health and Dietary Pattern Coherence

Cardiovascular health in the executive demographic is shaped by a complex interaction of genetic factors, stress physiology, and lifestyle variables — with dietary pattern carrying substantial independent weight. The Framingham Heart Study, one of the longest-running cardiovascular longitudinal studies in existence, has consistently shown that dietary quality, lipid profile, inflammatory status, and blood pressure trajectories are tightly linked in midlife adults.
Dietary pattern coherence — the consistency and quality of nutritional inputs over time — predicts cardiovascular risk more reliably than any single dietary intervention. This finding has direct implications for professionals who approach cardiovascular health through targeted supplementation or periodic dietary cleanses. A consolidated health plan replaces episodic intervention with a coherent, ongoing nutritional strategy. It maintains cardiovascular protective factors across time rather than cycling them on and off.
For executives who monitor cardiovascular biomarkers — including LDL particle size, apolipoprotein B, homocysteine, and triglyceride-to-HDL ratio — dietary pattern is the most direct and durable lever for moving those markers in a clinically favorable direction. A consolidated health plan ensures that cardiovascular nutritional strategy integrates with the broader protocol rather than sitting apart from it.
Muscle Mass, Protein Distribution, and the Sarcopenia Risk Window
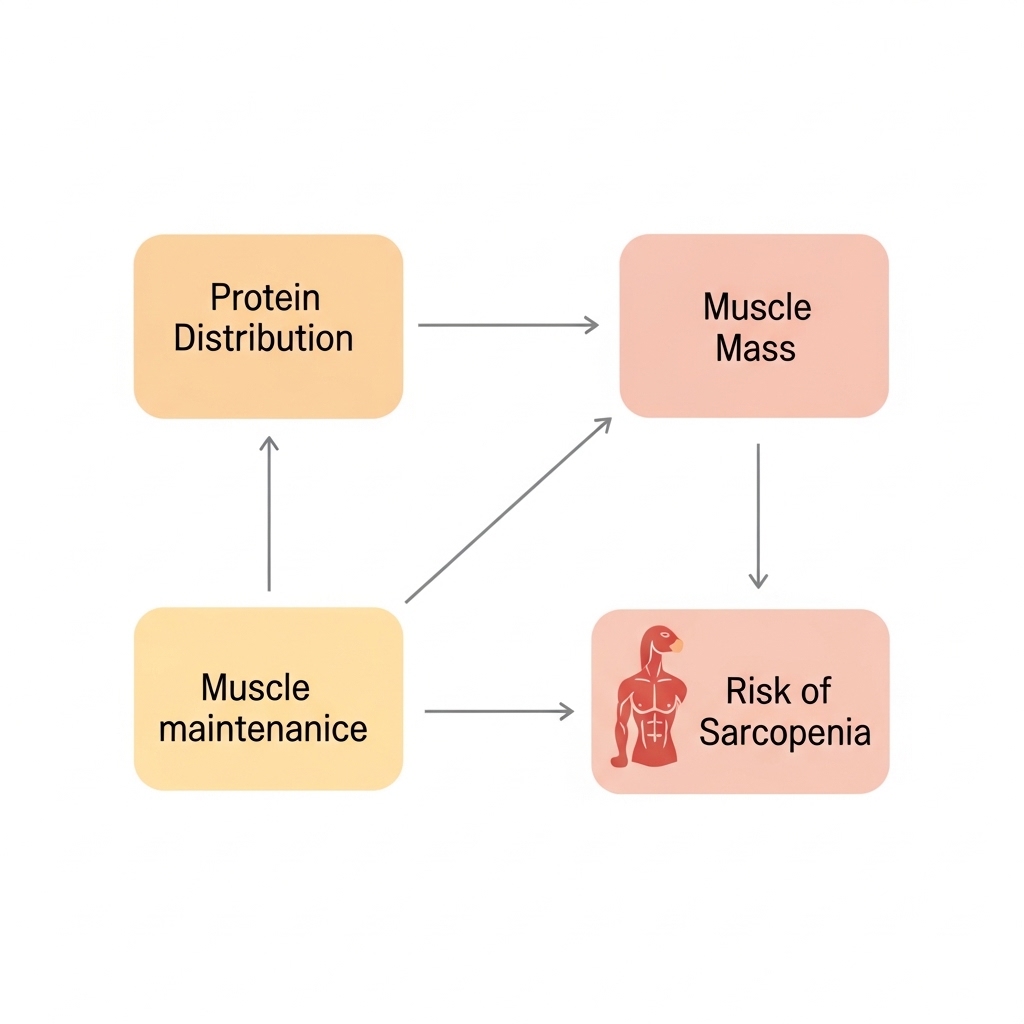
Sarcopenia — the age-related loss of muscle mass and function — begins earlier than most professionals expect. Without deliberate intervention, adults lose between three and eight percent of muscle mass per decade after age 30. The rate increases after 60. For executives in the 35-to-60 demographic, nutritional decisions made now directly shape muscle mass over the following two decades.
Protein distribution across the day — not just total protein intake — is among the most well-supported nutritional variables for preserving muscle mass. Research published in the American Journal of Clinical Nutrition has established that spreading protein intake across meals, rather than concentrating it in one or two sittings, maximizes muscle protein synthesis throughout the day. A consolidated health plan treats this distribution as a core nutritional variable, not a secondary consideration.
Within an integrated framework, muscle preservation connects to metabolic health, insulin sensitivity, and cognitive function. Skeletal muscle is the body's primary site of glucose disposal. Maintaining its mass and metabolic activity directly supports insulin sensitivity and reduces metabolic disease risk. A consolidated health plan that addresses protein distribution as both a performance and a longevity variable addresses multiple downstream outcomes at once.
Biomarker Monitoring Within a Consolidated Health Plan

A consolidated health plan is not static. It evolves in response to biomarker data — the objective, measurable signals that indicate whether the protocol is producing its intended physiological outcomes. Without biomarker monitoring, a health plan operates on assumption. With it, the plan becomes an adaptive, evidence-driven system.
The biomarkers most relevant to nutritional optimization in the executive demographic include fasting insulin, HbA1c, hs-CRP, lipid particle analysis, ferritin, homocysteine, vitamin D, and omega-3 index. Together, these markers provide a clear picture of metabolic function, inflammatory status, cardiovascular risk, and nutritional sufficiency. Tracking them over time within a consolidated framework reveals trends that single time-point measurements cannot capture.
Biomarker data also allows for precise nutritional adjustment. When inflammatory markers shift, dietary inputs can be modified in response. When metabolic markers improve, the protocol can be refined to maintain and extend that progress. This adaptive feedback loop — only possible within a consolidated health plan — transforms nutrition from a static dietary prescription into a dynamic, responsive system.
Stress Physiology and Nutritional Strategy Under Cortisol Burden

Chronic cortisol elevation — common in professionals managing sustained high-demand environments — directly alters nutritional metabolism. Cortisol drives preferential storage of visceral fat, promotes muscle breakdown, impairs protein synthesis, and increases cravings for high-calorie, low-nutrient food. Nutritional strategy must account for these physiological realities directly.
A consolidated health plan addresses cortisol burden through nutritional architecture that supports HPA axis regulation. Adequate dietary magnesium, consistent blood sugar regulation through balanced macronutrient distribution, and the avoidance of stimulant-driven appetite suppression during high-cortisol periods are all nutritional variables with documented relevance to cortisol physiology. These connections are only visible — and only actionable — within a consolidated framework.
The interaction between stress physiology and nutrition also runs in reverse. Poor nutritional choices — irregular meal timing, high glycemic intake, alcohol consumption — raise cortisol and amplify the stress burden the executive already carries. A consolidated health plan breaks this feedback loop by designing nutritional inputs that support rather than worsen the body's stress response systems.
Translating the Evidence Into a Consolidated Health Plan

Professionals who seek to reduce biological age trajectory, protect cognitive performance, and build durable cardiovascular and metabolic health have a clear evidence-based pathway available. A consolidated health plan — one that brings together dietary pattern, nutritional timing, protein distribution, inflammatory management, and biomarker monitoring into one coherent framework — is the structural tool that makes those outcomes achievable.
Practically, this means beginning with a comprehensive biomarker assessment to establish a baseline. It means engaging a clinical nutrition professional who works within a performance longevity framework. It also means mapping current health interventions against a unified protocol to identify gaps, overlaps, and conflicts.
Establishing a quarterly review cycle that adjusts the plan in response to evolving biomarker data closes the loop. The goal is not perfection at any single data point. It is a coherent, adaptive system that builds its benefits across years and decades — and a consolidated health plan is the architecture that makes that possible.
UP NEXT: 2026 Whole Living Action Plan: 28 Day Challenge
Professionals who lack a consolidated health plan accumulate fragmented physiological inputs — elevated allostatic load, unmanaged inflammatory markers, and disrupted metabolic signaling — a combination that research consistently links to a biological age three to seven years above chronological age in midlife adults. WholeLiving's Biological Age Estimation Model incorporates this factor directly — your assessment takes under five minutes.
Ready to understand how these factors are influencing your biological age right now? [Take the Biological Age Assessment →]






