Skin barrier dysfunction is not a cosmetic inconvenience — it is a measurable indicator of systemic inflammatory load. For executives operating under chronic stress, repeated use of harsh facial cleansers disrupts the stratum corneum and elevates transepidermal water loss. Additionally, it triggers localized cytokine activity that compounds whole-body inflammation. Over time, this accelerates dermal aging and compromises immune signaling at the skin level. It also correlates with elevated cortisol patterns that extend well beyond the bathroom routine. Establishing a daily gentle cleansing protocol is not a skincare preference — it is a low-cost, high-leverage intervention. This approach benefits professionals managing biological age with the same precision they apply to recovery and nutrition.
The Skin as a Systemic Organ
Dermatological research has progressively reframed the skin as an active immunological interface. It maintains direct communication pathways to systemic physiology — not a passive external surface. The stratum corneum operates as a regulated barrier. It modulates fluid retention, microbial exposure, and inflammatory signaling.
When this barrier is disrupted, the consequences extend beyond the surface. In conditions of sustained barrier compromise, localized cytokine activity can contribute to systemic inflammatory signaling — a mechanism well-documented in pathological skin conditions and increasingly studied in the context of subclinical barrier disruption.
Researchers at the National Institutes of Health have consistently linked this inflammatory activity to accelerated biological aging and increased risk of metabolic and cardiovascular disease.
What Harsh Cleansers Actually Do to the Barrier

Most commercially available facial cleansers — particularly foaming formulations — carry high surfactant concentrations and alkaline pH levels, typically ranging from 9 to 11. The skin's natural pH sits between 4.5 and 5.5, maintained by sebaceous secretions and the acid mantle. Repeated exposure to alkaline cleansers disrupts this pH gradient.
It degrades lipid-protein structures within the stratum corneum and reduces serine protease activity responsible for barrier self-repair. Multiple studies in dermatological literature — including research published in Skin Pharmacology and Physiology — have documented measurable increases in transepidermal water loss following regular use of high-pH cleansers, with barrier recovery taking between 14 and 24 hours per disruption episode.
Barrier recovery takes between 14 and 24 hours per disruption episode. Professionals cleansing twice daily with an incompatible formulation keep the barrier in a perpetual state of partial compromise.
Transepidermal Water Loss as a Measurable Variable

TEWL is a clinical indicator of barrier integrity — not simply a measure of hydration. Elevated TEWL correlates with increased permeability to environmental antigens, microorganisms, and pollutants.
Each of these independently activates toll-like receptors in the dermis and triggers innate immune responses. In individuals with intact barrier function, this activation remains minimal and self-limiting. In a high-stress professional with chronically elevated cortisol, the immune response is already primed.
Barrier disruption adds an additional inflammatory input to a system operating near capacity. Over years and decades, this cumulative input carries measurable biological cost.
READ ALSO: Facial Wash for Oily Skin Everyone’s Secretly Using
Cortisol, Stress, and the Skin's Inflammatory Threshold

The relationship between psychological stress, cortisol secretion, and skin barrier function runs in both directions. Cortisol suppresses ceramide synthesis — the primary lipid molecules that maintain stratum corneum cohesion.
Research examining psychophysiological stress responses — including work conducted at the University of California San Francisco — has found that acute stress induction measurably slows skin barrier recovery rates in healthy adult subjects.
The physiological state characteristic of sustained executive performance — elevated cortisol, compressed recovery windows, high cognitive demand — actively degrades the skin's capacity to repair its barrier. Cleanser choice either compounds this suppression or works within it.
The pH Compatibility Principle
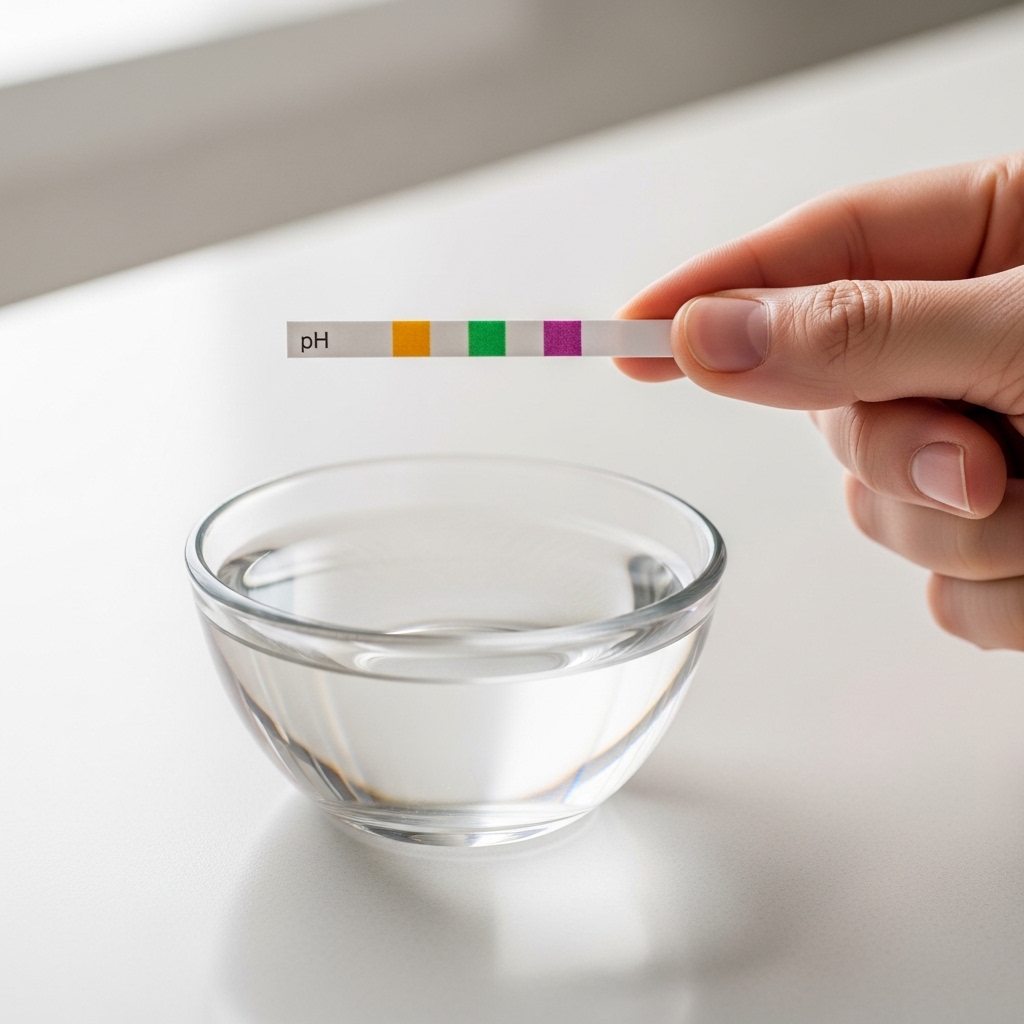
Gentle facial cleansers formulated at a pH between 4.5 and 6.5 — syndet bars or low-foaming gel formulations — preserve the acid mantle while removing sebum, oxidized lipids, and particulate matter effectively.
This distinction from conventional soap-based cleansers is measurable in post-wash TEWL, skin surface pH recovery, and microbiome composition. The cutaneous microbiome is pH-sensitive.
Alkaline disruption disadvantages beneficial colonizers such as Staphylococcus epidermidis, which produces fatty acids that reinforce acid mantle integrity. It simultaneously creates conditions more permissive to pathogenic species
The Microbiome Connection to Systemic Health

The cutaneous microbiome functions as an extension of the body's broader microbial ecosystem. It maintains functional links to immune education and inflammatory regulation. Peer-reviewed research in cutaneous immunology has outlined mechanisms by which skin-resident microbial communities communicate with resident dendritic cells and T-lymphocytes.
These interactions are understood to influence systemic immune tone, though the full clinical implications in healthy adults remain an active area of study. Repeated chemical disruption of this community — including from harsh surfactants — is not a localized event.
It represents a point of entry for dysregulated immune activation. For professionals tracking inflammatory biomarkers such as high-sensitivity C-reactive protein (hs-CRP), this input warrants inclusion in the broader picture.
READ ALSO: Salicylic Acid Face Wash Products Worth Adding to Cart
Morning vs. Evening Cleansing: Functional Distinctions

The functional rationale for cleansing differs between morning and evening. Evening cleansing removes accumulated residue — urban pollution, oxidized sebum, and topical product application. These inputs continue low-level inflammatory activity against the barrier if left overnight.
The skin undergoes its primary regenerative activity during sleep, with circadian research indicating that barrier lipid synthesis and cellular turnover accelerate during nocturnal rest periods — the precise timing varying with individual sleep architecture. Barrier lipid synthesis accelerates during this window and cellular turnover increases.
Removing barrier-disrupting residues beforehand optimizes repair conditions. Morning cleansing addresses sebum and perspiration from sleep — a lighter load. Many individuals with normal to dry skin find water alone sufficient for the morning routine.
Inflammation, Biological Age, and the Compounding Effect

Biological age — estimated through epigenetic clocks such as the Horvath DNAm clock — has shown stronger associations with certain health outcomes than chronological age alone in several longitudinal studies, though the field continues to refine how these measurements translate to clinical prediction.
Chronic low-grade inflammation ranks among the most consistently identified drivers of epigenetic age acceleration. The mechanisms include oxidative stress-induced DNA methylation changes and mitochondrial dysfunction. Telomere attrition represents a parallel aging biomarker — distinct from epigenetic clock measures but similarly sensitive to cumulative inflammatory load.
The framework of allostatic load positions every source of inflammatory input as relevant. Skin barrier disruption occurring twice daily across years is not a trivial input in this calculus.
What the Research Does Not Yet Quantify

The boundaries of current evidence deserve acknowledgment. Direct longitudinal studies linking cleanser pH to systemic inflammatory biomarkers or epigenetic aging outcomes in human subjects remain limited.
Most mechanistic data derives from in vitro barrier models, short-duration clinical trials, or studies examining atopic dermatitis where barrier dysfunction is already pathological. Extrapolating to the healthy but high-stress executive requires inference.
What the evidence establishes clearly is the mechanism: barrier disruption increases inflammatory signaling, that signaling under chronic stress is systemically consequential, and pH-compatible cleansers measurably reduce disruption. The logical chain holds even where endpoint data remains incomplete.
READ ALSO: Dry Skin Moisturizer Tips for Soft, Nourished Skin
Formulation Criteria Worth Evaluating

Beyond pH compatibility, several formulation variables affect barrier outcomes. Fragrance — synthetic and natural — ranks among the most common sources of contact sensitization. It activates immune responses that elevate local cytokine levels even without visible irritation.
Sulfate-based surfactants, including sodium lauryl sulfate, produce measurable barrier disruption at concentrations common in commercial cleansers. These are functional components with documented roles in barrier maintenance — not cosmetic additions.
Formulations containing glycerin and panthenol have demonstrated capacity to partially offset surfactant-induced TEWL in clinical settings. Niacinamide contributes to barrier support through a distinct pathway — stimulating ceramide synthesis — which over time reinforces stratum corneum cohesion.
Evidence-Based Options for Daily Practice

Professionals applying this evidence have several well-supported options. Transitioning to a syndet-based or low-foaming gel cleanser with a pH between 4.5 and 6.5 represents the most direct intervention the barrier research supports.
Avoiding fragrance and sulfate surfactants reduces the two most common sources of chemical barrier insult. Limiting morning cleansing to water or a minimal formulation — particularly for those with normal to dry skin — reduces cumulative daily disruption without compromising hygiene.
For individuals tracking inflammatory biomarkers such as hs-CRP or using epigenetic age testing within a longevity protocol, documenting cleanser selection as a variable allows more granular assessment of its contribution over time.
UP NEXT: Body Wash for Slowing Down in a Fast Morning
Repeated disruption of the skin barrier through daily use of high-pH cleansers sustains a low-grade inflammatory state that contributes to epigenetic age acceleration — placing an otherwise manageable daily habit among the modifiable inputs that longevity-focused biomarker tracking is designed to detect. WholeLiving's Biological Age Estimation Model incorporates this factor directly — your assessment takes under five minutes.
Ready to understand how these factors are influencing your biological age right now? [Take the Biological Age Assessment →]






