Approximately 30 percent of individuals with major depressive disorder do not respond to two or more antidepressant trials. This defines treatment-resistant depression clinically. For high-performing professionals, this failure point is not an abstract statistic. It represents months or years of unresolved executive dysfunction. Elevated inflammatory burden accumulates. Decision-making precision declines measurably — directly compromising the cognitive output that high-stakes professional performance demands. Sustained treatment failure also correlates with accelerated biological aging and compounding neurobiological deterioration. Advanced psychiatric interventions, including mindful health solutions, now offer clinically validated pathways beyond this threshold.
Defining Treatment-Resistant Depression Clinically

Treatment-resistant depression (TRD) is not a vague clinical term. Specifically, it describes a diagnostic situation where major depressive disorder fails to respond to at least two adequate antidepressant trials of sufficient dose and duration. This threshold matters because it shifts the clinical framework entirely. As a result, standard pharmacological approaches no longer apply.
Beyond the definition itself, TRD affects a substantial subset of the depressive population. Research from the National Institutes of Health estimates that between 30 and 50 percent of individuals with major depressive disorder experience inadequate response to initial treatment. Among high-functioning professionals, however, this figure may underrepresent true prevalence. Compensatory behavior masks symptom severity and delays accurate clinical escalation.
Consequently, the consequences of misclassifying TRD as ordinary treatment lag are significant. Clinicians who continue rotating through standard antidepressants without reassessing the diagnostic picture expose patients to prolonged neurobiological deterioration. Each additional month of unresolved depression compounds structural brain changes, inflammatory burden, and functional decline. Therefore, accurate TRD identification is the first clinical priority.
Why Standard Antidepressants Fail in TRD
Standard antidepressants — primarily SSRIs and SNRIs — target monoamine neurotransmitter systems. Specifically, they modulate serotonin, norepinephrine, and dopamine reuptake. For many patients, this mechanism produces meaningful symptom relief. For individuals with TRD, however, it does not.
Emerging research suggests TRD involves neurobiological pathways that monoamine-based medications do not adequately address. These include glutamate system dysregulation, disrupted neuroplasticity signaling, and chronic neuroinflammation. Notably, research published in Nature Medicine has identified glutamatergic dysfunction as a core feature of treatment-resistant presentations, explaining why dopaminergic and serotonergic interventions produce insufficient response.
Beyond mechanism, pharmacogenomic variation plays a compounding role. Genetic differences in cytochrome P450 enzyme activity affect how individuals metabolize antidepressant medications. Some professionals metabolize standard antidepressants too rapidly to achieve therapeutic plasma levels. Others, by contrast, experience toxicity at standard doses. Without pharmacogenomic testing, clinicians operate without critical biological data — a gap that contributes directly to treatment failure.
The Neurobiological Toll of Prolonged TRD
Every month of unresolved TRD carries measurable neurobiological cost. The HPA axis remains chronically activated, sustaining elevated cortisol. As a result, elevated cortisol suppresses BDNF, reduces hippocampal volume, and accelerates neuronal damage. These changes are not temporary — they accumulate across depressive episodes.
Furthermore, chronic neuroinflammation intensifies this process. Elevated interleukin-6 and tumor necrosis factor-alpha — inflammatory cytokines consistently elevated in TRD — disrupt synaptic function and impair neuroplasticity. Research from the National Institutes of Health links sustained neuroinflammatory states to accelerated cognitive aging and reduced response to conventional antidepressant treatment.
For professionals, the functional manifestations are equally measurable. Executive function degrades. Processing speed slows. Working memory capacity diminishes. These are not subjective complaints — neuropsychological assessment consistently documents these deficits in TRD populations. Moreover, the longer TRD remains unresolved, the deeper these deficits become, and the more difficult full cognitive recovery becomes.
READ ALSO: Natural Remedies for Depression: A Gentle, Holistic Approach
TRD and Accelerated Biological Aging

TRD does not confine its damage to the brain. Rather, it accelerates biological aging across multiple physiological systems simultaneously. Sustained cortisol elevation and chronic neuroinflammation promote telomere shortening — a direct marker of cellular aging. Research linking elevated inflammatory markers to reduced telomere length is well-established across major institutional bodies, including the Harvard T.H. Chan School of Public Health.
In addition to cellular aging, metabolic function deteriorates progressively. TRD reduces motivation for physical activity, disrupts appetite regulation, and impairs sleep architecture. These changes collectively decrease VO2 max, increase insulin resistance, and promote visceral fat accumulation. Each of these variables independently predicts accelerated biological aging and increased all-cause mortality risk.
As a further consequence, cardiovascular health faces compounding risk. Elevated IL-6 and TNF-α promote arterial inflammation and endothelial dysfunction. Professionals with prolonged TRD carry cardiovascular risk profiles that diverge significantly from their chronological age. Treating TRD is therefore not only a psychiatric priority — it is a longevity intervention with measurable impact across biological systems.
Ketamine and Esketamine: Mechanism and Clinical Evidence
Ketamine represents the most significant pharmacological advancement in depression treatment in decades. Unlike standard antidepressants, ketamine acts on the glutamate system — specifically as an NMDA receptor antagonist. This distinct mechanism produces rapid synaptic potentiation and promotes neuroplasticity through BDNF upregulation. Consequently, clinical response often occurs within hours rather than weeks.
Building on this mechanism, IV ketamine infusion therapy has demonstrated robust efficacy in TRD populations across multiple clinical trials. Research published in Biological Psychiatry documented significant antidepressant response rates in TRD patients receiving IV ketamine, with effects emerging within 24 hours of administration. For professionals unable to sustain prolonged functional impairment, this speed of action carries direct practical value.
Additionally, esketamine — the S-enantiomer of ketamine — received FDA approval in 2019 as the first specifically indicated treatment for TRD. Administered intranasally under clinical supervision, esketamine provides a more standardized delivery protocol than IV infusion. Both formulations require clinical monitoring and structured treatment protocols. Importantly, neither represents a standalone solution — both work most effectively within a comprehensive psychiatric care framework.
READ ALSO: Fighting Depression with Natural Remedies
Transcranial Magnetic Stimulation: Non-Pharmacological Intervention
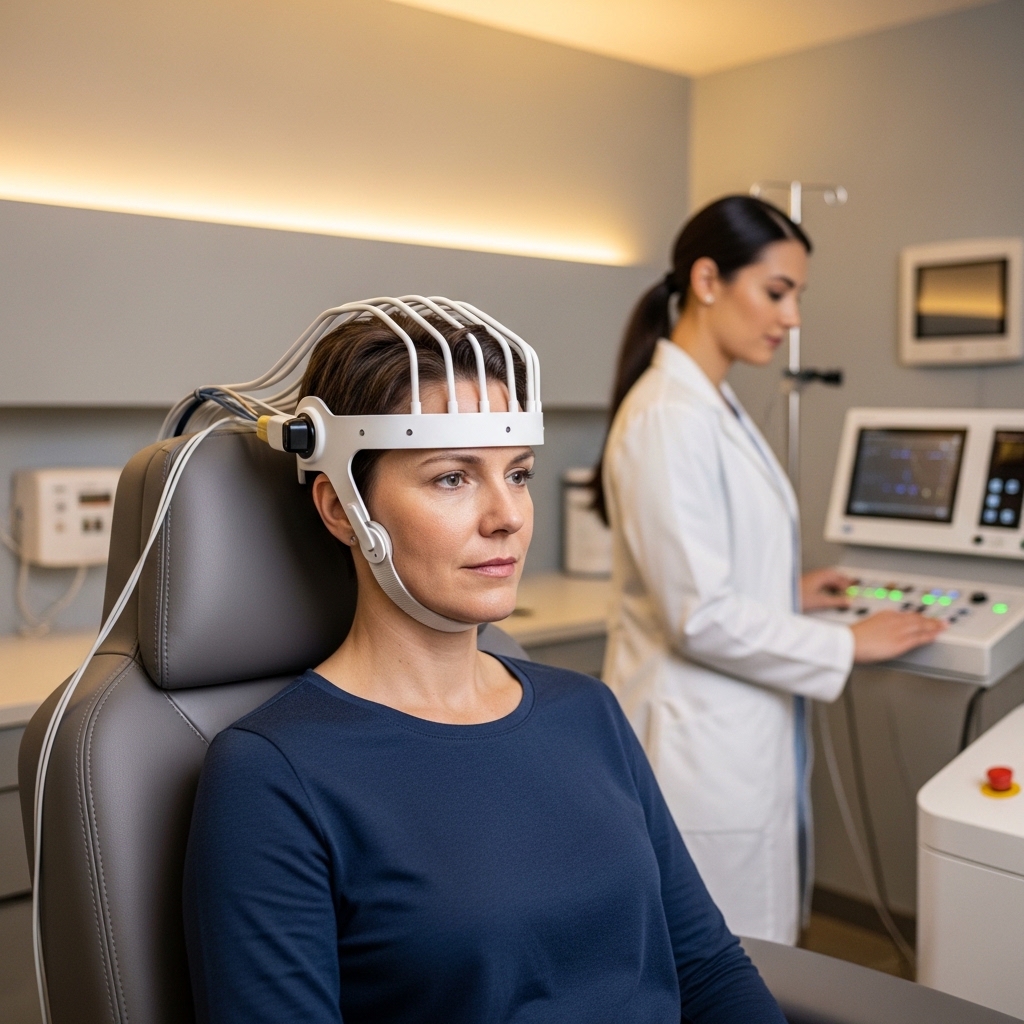
Transcranial magnetic stimulation (TMS) offers a non-pharmacological pathway for TRD. It delivers focused magnetic pulses to targeted cortical regions — primarily the left dorsolateral prefrontal cortex — to modulate neural activity in circuits disrupted by depression. Unlike pharmacological options, it does not require anesthesia and carries a favorable tolerability profile.
Since its FDA clearance for major depressive disorder in 2008, clinical evidence for TMS has continued to expand. Research published in the Journal of Clinical Psychiatry demonstrated significant response and remission rates in TRD patients undergoing TMS, including those who had failed multiple antidepressant trials. For professionals seeking effective treatment without systemic pharmacological exposure, TMS therefore presents a clinically validated option.
More recently, accelerated TMS protocols — delivering multiple sessions per day over a compressed timeframe — have emerged as an area of active clinical investigation. Stanford University's accelerated intermittent theta-burst stimulation (iTBS) protocol produced notably high remission rates in a rigorous trial published in Nature Medicine. These compressed protocols reduce overall treatment duration, which carries particular relevance for professionals managing demanding schedules.
Emerging Interventions: Psychedelic-Assisted Therapy

Psilocybin-assisted therapy represents an emerging intervention for TRD with a rapidly growing evidence base. Research from Johns Hopkins University and Imperial College London has documented significant antidepressant effects following supervised psilocybin administration in clinical settings. Notably, response rates in TRD populations have been substantial, with effects persisting weeks to months following a small number of sessions.
Mechanistically, psilocybin acts on serotonin 5-HT2A receptors and promotes neuroplasticity through pathways distinct from both conventional antidepressants and ketamine. It produces rapid shifts in default mode network activity — a brain network consistently dysregulated in depression. This distinct mechanism may explain why it reaches patients who have not responded to glutamatergic or monoaminergic interventions.
Despite this promise, regulatory status for psilocybin-assisted therapy varies by jurisdiction and remains an active area of clinical development. It is not yet widely available within standard psychiatric practice. However, clinical trial access and approved treatment centers exist in select jurisdictions. Professionals exploring this option therefore require specialist guidance and rigorous clinical screening before consideration.
The Role of Precision Medicine in TRD Management

Precision medicine reframes TRD treatment from a trial-and-error process into a data-driven clinical strategy. Specifically, pharmacogenomic testing identifies genetic variants that affect drug metabolism, receptor sensitivity, and treatment response prediction. This information allows clinicians to select interventions based on individual biological profile rather than population-level averages.
Building further on this framework, biomarker-informed treatment selection is an expanding area of TRD research. Inflammatory marker panels, neuroimaging data, and HPA axis function assessments can each contribute to a more precise understanding of a patient's neurobiological state. Some TRD presentations are driven predominantly by neuroinflammation. Others, by contrast, reflect glutamatergic dysregulation or HPA hyperactivation — each profile pointing toward different intervention strategies.
For high-performing professionals accustomed to data-driven decision-making, precision medicine represents a logical framework for psychiatric care. It replaces ambiguity with measurable clinical information and reduces time spent on ineffective treatments. Ultimately, it aligns mental health management with the same evidence-based rigor applied to other aspects of executive health optimization.
READ ALSO: Severe Depression, Executive Function Impairment, and the Evidence-Based Protocols That Support Recovery
Integrating Advanced Interventions With Psychotherapy

Advanced biological interventions produce stronger and more durable outcomes when integrated with structured psychotherapy. Specifically, ketamine and TMS both promote neuroplasticity — creating a biological window during which the brain is more receptive to cognitive and behavioral change. Psychotherapy delivered within this window directly leverages the intervention's neurobiological effect.
In this context, cognitive-behavioral therapy and acceptance-based approaches provide structured frameworks for addressing maladaptive thought patterns that sustain depressive states beyond the biological trigger. Research consistently demonstrates that combined treatment — biological intervention plus psychotherapy — reduces relapse rates and extends remission duration compared to either approach alone.
For professionals in TRD recovery, psychotherapy additionally addresses the occupational and relational consequences of prolonged illness. Extended depressive episodes damage professional relationships, erode self-efficacy, and create avoidance patterns that persist even after biological symptoms remit. As a result, structured psychotherapy targets these residual functional deficits directly, supporting full rather than partial recovery.
Monitoring Recovery: Objective Metrics Over Subjective Report

Recovery from TRD requires objective monitoring. Subjective self-report alone provides insufficient clinical data — particularly in high-performing professionals who tend to overestimate functional recovery and return to occupational demands prematurely. Validated assessment tools, therefore, provide a more accurate and actionable picture.
Specifically, neuropsychological testing quantifies changes in executive function, processing speed, and working memory across treatment. These metrics track cognitive recovery independently of mood symptom scores. A professional may report improved mood while neuropsychological testing reveals persistent executive function deficits — a pattern that predicts relapse if occupational demands escalate before full cognitive recovery occurs.
In addition to cognitive metrics, inflammatory biomarker panels and cortisol assessments provide critical biological data points. Tracking IL-6, TNF-α, and morning cortisol levels across treatment reveals whether the neurobiological drivers of TRD are responding alongside symptomatic improvement. Professionals who apply the same data discipline to psychiatric recovery that they apply to other health domains consistently achieve more durable outcomes.
Evidence-Based Pathways for High-Performing Professionals With TRD

Formal reassessment by a psychiatrist specializing in treatment-resistant presentations is the appropriate starting point for professionals who have not responded to standard antidepressant treatment. From there, pharmacogenomic testing can clarify whether biological factors contributed to prior treatment failure. Building on this foundation, a structured escalation protocol — incorporating ketamine, esketamine, TMS, or emerging options within clinical trial frameworks — can be developed based on individual neurobiological profile. Integrating psychotherapy alongside biological intervention, monitoring recovery with validated neuropsychological tools, and tracking inflammatory and cortisol biomarkers transforms TRD management into a measurable, data-informed process. The evidence strongly favors early escalation to advanced interventions over continued rotation through inadequate standard treatments.
UP NEXT: The Role of Psychotherapy in Managing Postpartum Depression
Professionals with unresolved treatment-resistant depression carry measurably elevated inflammatory cytokines, sustained cortisol dysregulation, and accelerating telomere shortening — a convergence of biological mechanisms that can advance biological age by several years beyond chronological age, compounding longevity risk across cardiovascular, metabolic, and cognitive systems simultaneously. WholeLiving's Biological Age Estimation Model incorporates this factor directly — your assessment takes under five minutes.
Ready to understand how these factors are influencing your biological age right now? [Take the Biological Age Assessment →]






