Chronic postprandial gastrointestinal distress represents a significant physiological tax on executive cognitive performance, frequently manifesting as diminished executive function and accelerated biological age markers. For the high-performing professional, persistent gastric inflammation and acute abdominal discomfort are not merely inconveniences; they trigger systemic cortisol elevation and a subsequent decline in neuroplasticity. Clinical evidence suggests that recurring stomach problems after eating and digestive dysfunction disrupt the enteric nervous system’s equilibrium, directly correlating with impaired decision-making speed and reduced metabolic efficiency. Left unaddressed, these symptomatic indicators of gut barrier permeability may contribute to long-term cardiovascular risk profiles, necessitating a rigorous, data-driven diagnostic approach to preserve both immediate output and overall longevity trajectories.
Dysregulation of the Gut-Brain Axis and Executive Output
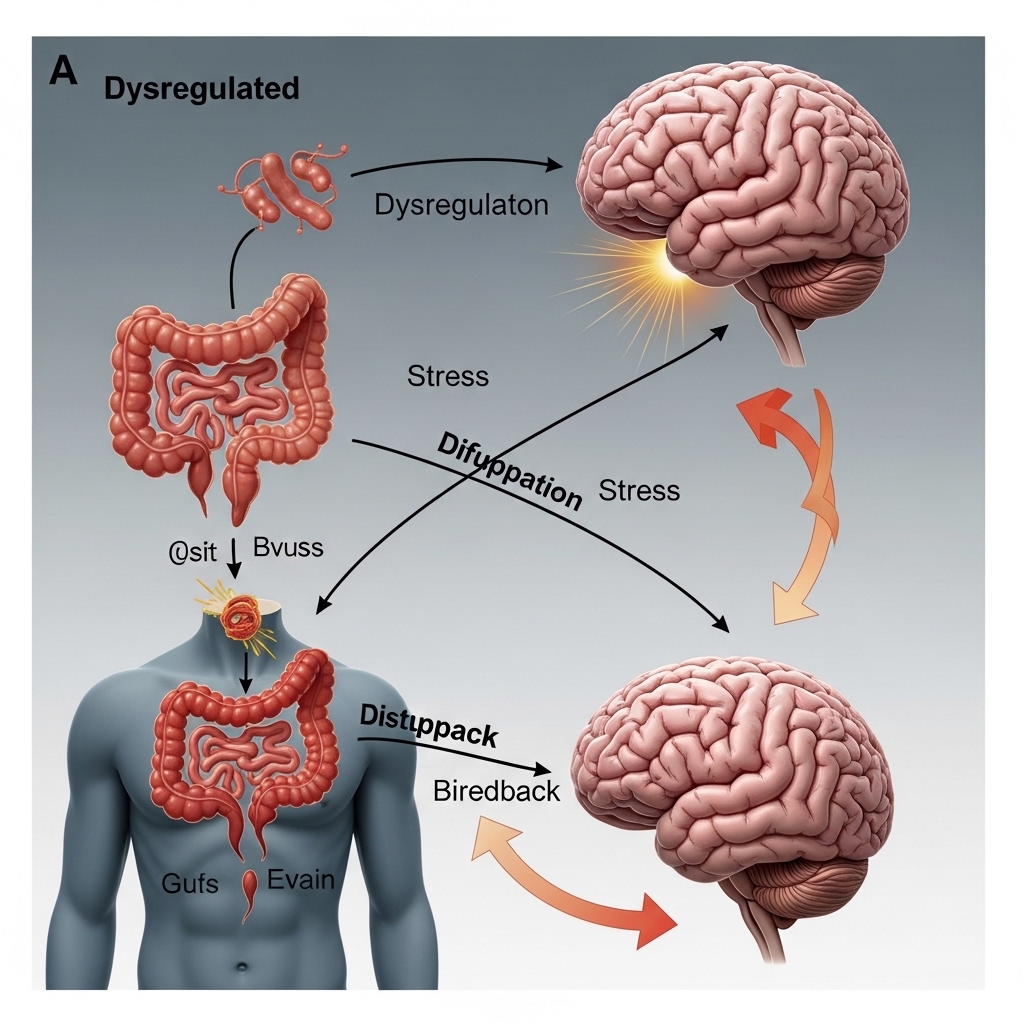
The enteric nervous system (ENS), often called the “second brain,” uses the vagus nerve to communicate with the central nervous system. When a professional feels post-meal pain or bloating, these signals disrupt the prefrontal cortex’s ability to maintain high-level focus. This shift happens because the body diverts metabolic energy and activates the sympathetic nervous system, which directly reduces cognitive speed and complex problem-solving skills.
Research from the Harvard T.H. Chan School of Public Health shows that gut inflammation can release cytokines that cross the blood-brain barrier. These chemicals impair synaptic plasticity and lead to “brain fog” or slower mental processing during high-stakes work. Over time, this chronic inflammation can cause neuroinflammation, which is a known factor in cognitive decline and reduced mental stamina.
Vagal signals from a distressed gut also affect the amygdala, which can raise stress and anxiety levels during the workday. When this gut-brain connection is broken, an executive may experience more irritability or emotional shifts that hurt leadership and team dynamics. Restoring this balance is a strategic move to protect both emotional intelligence and daily mental output.
READ ALSO: Healthy Meals For Dinner You’ll Crave All Week
Postprandial Glucose Variability and Metabolic Stability
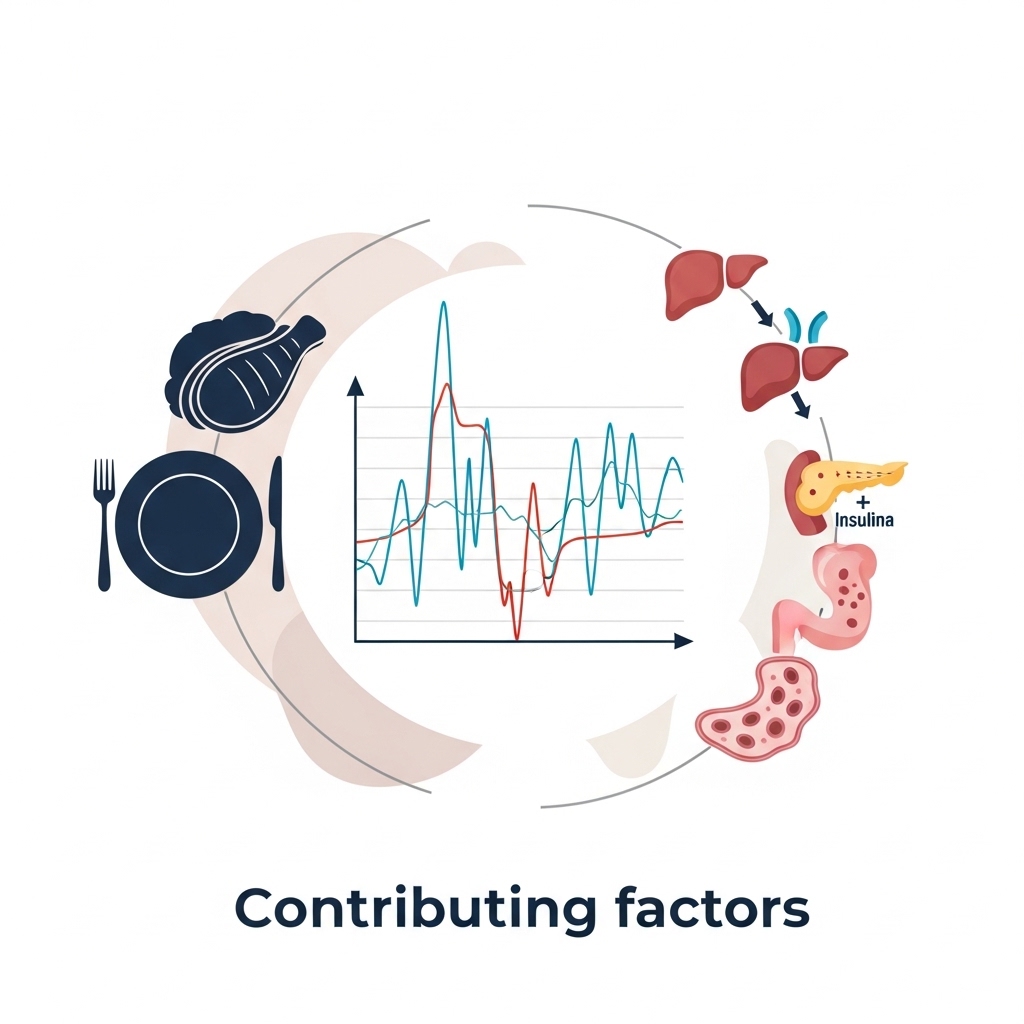
Sharp cramps or a heavy stomach feeling after eating often mean the body is not managing glucose well. Rapid blood sugar spikes followed by steep drops create metabolic instability and increase oxidative stress. This cycle forces the pancreas to pump out more insulin, leading to periods of low energy and a loss of executive drive.
Data from the National Institutes of Health (NIH) shows that frequent blood sugar swings predict heart issues and cellular aging better than fasting glucose levels. For those aged 35 to 60, these swings are a major factor in long-term health because they damage proteins and lower mitochondrial power. Keeping these levels steady is vital for the constant energy needed for physical and mental tasks.
Cellular stress from glucose swings can also increase advanced glycation end products (AGEs), which make tissues less elastic and age the blood vessels. This process speeds up cardiovascular aging and can reduce blood flow to the brain and other vital organs. By stabilizing blood sugar after meals, a professional can slow these aging markers and keep the body’s metabolic systems flexible.
READ ALSO: Best Vitamins and Minerals for Immunity: What You Need
The Role of Gut Permeability in Systemic Inflammation
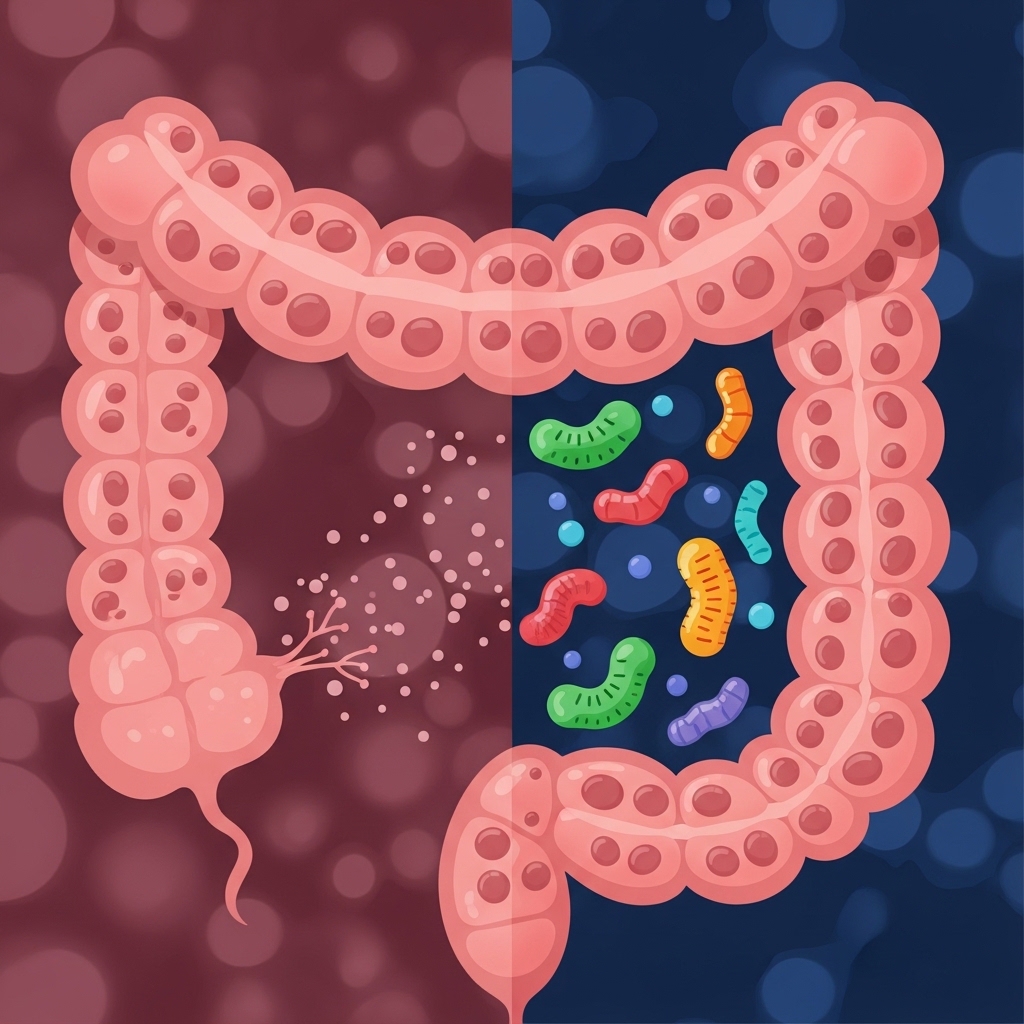
Post-meal discomfort is often a sign of a compromised intestinal barrier, a condition commonly known as “leaky gut.” When the gut lining weakens, undigested food and bacterial toxins called lipopolysaccharides (LPS) enter the bloodstream. This causes an immediate immune response that raises C-reactive protein (CRP) levels and keeps the body in a state of high alert.
Long-term data from The Lancet links chronic inflammation from gut permeability to higher risks of metabolic syndrome and brain disease. In a professional setting, this inflammatory load pulls energy away from recovery and lowers a person's daily performance ceiling. Additionally, the presence of LPS in the blood can harm insulin sensitivity, making it harder to maintain a healthy metabolism.
This state also burdens the liver, which must filter the toxins that slipped past the gut barrier. When the liver is overwhelmed, systemic toxicity rises, leading to fatigue and lower physical performance. Fixing gut permeability is a foundational step to lower the body's total stress and free up energy for demanding professional tasks.
Cortisol Dynamics and Digestive Inhibition
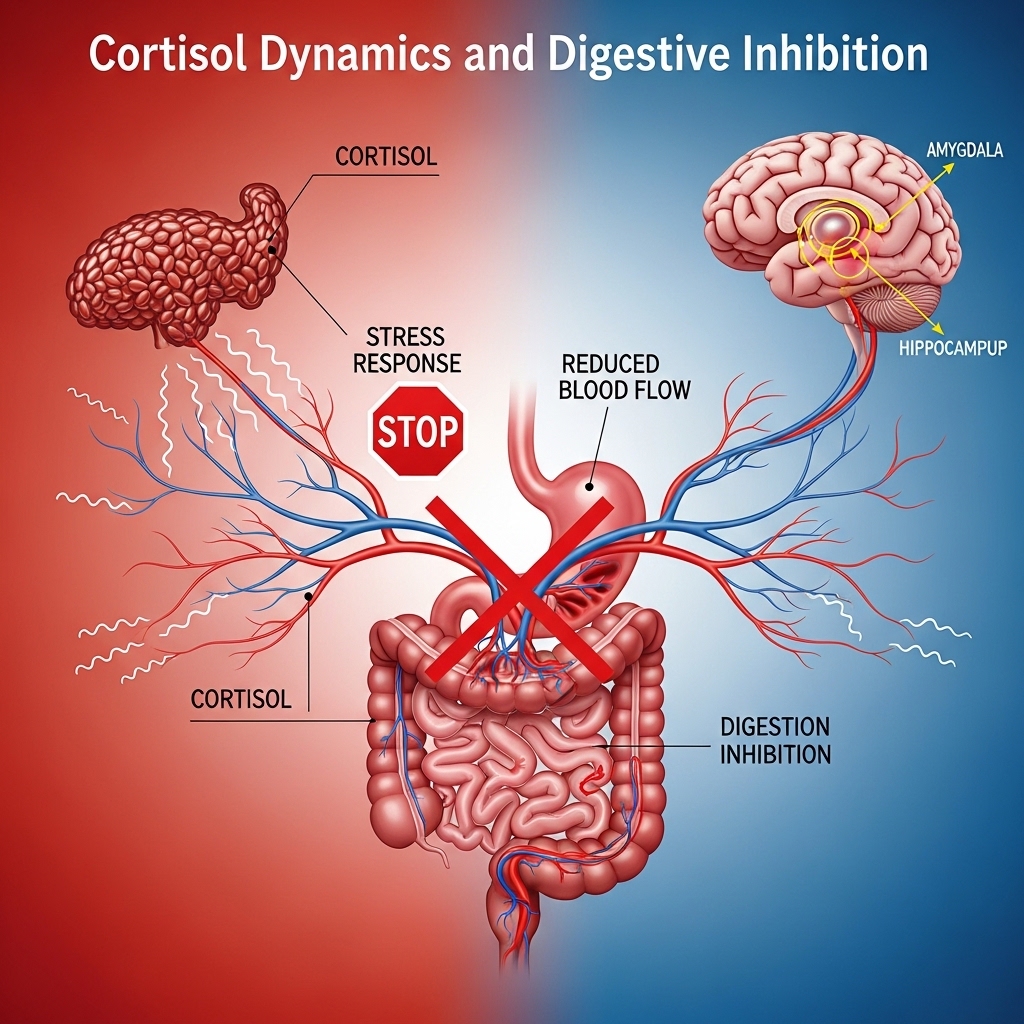
High-performing professionals often live in a state of high sympathetic nervous system activity. Eating while in this “fight or flight” mode stops the “rest and digest” response, leading to low stomach acid and fewer digestive enzymes. This mismatch means the body cannot handle the food, resulting in significant pain and chemical distress.
High cortisol levels slow down how fast the stomach empties and change the gut microbiome to favor harmful bacteria. This lack of acid results in poorly digested food reaching the small intestine, which causes sharp pain and gas. As a result, the simple act of eating becomes a source of stress rather than a way to recharge.
Chronic high cortisol also causes the body to store more fat in the visceral area around the organs. This fat produces its own inflammatory chemicals that make gut pain and systemic stress even worse. Breaking this cycle requires a deliberate move toward a calm state before and during meals to ensure proper digestive signaling.
Microbiome Diversity as a Longevity Variable

The mix of bacteria in the gut is a key part of biological age and overall resilience. A diverse microbiome makes short-chain fatty acids like butyrate, which have strong anti-inflammatory effects. These substances are essential for keeping the gut lining strong and helping the immune system react correctly to threats.
A study in Nature Medicine found that people who live to 100 or have high “healthspans” share specific microbial patterns. For an executive, keeping this bacterial diversity is necessary for steady performance and slowing age-related decline. On the other hand, gut pain often points to an imbalance where bad bacteria take over and drain the body's energy.
The microbiome also produces important chemicals like serotonin and GABA, which help regulate mood and stress. An imbalanced gut can lead to chemical gaps that show up as higher anxiety or a lower ability to handle high-pressure careers. Investing in gut health is an investment in the mental resilience needed for long-term career success.
Impact on Nocturnal Recovery and Sleep Architecture
Gut distress after dinner has a measurable negative effect on sleep, especially deep sleep and REM cycles. The metabolic work of processing food under stress raises core body temperature and keeps the heart rate high. Without a drop in temperature, the brain cannot enter the deep sleep stages needed for memory and emotional health.
When the body is busy handling gut inflammation, it cannot start the “cleaning” process the brain needs to remove toxins. This means the professional wakes up with lower mental clarity, creating a cycle where poor sleep makes digestion even worse the next day. Over time, this cycle can lower physical capacity and VO2 max.
Late-night digestive stress also disrupts the release of growth hormone, which is vital for repairing tissue and muscle. This hormonal shift can lead to slower recovery from exercise and a higher risk of getting injured. Prioritizing gut comfort in the evening is a key part of any plan that views sleep as the best recovery tool.
Functional Hypochlorhydria in the 35–60 Demographic
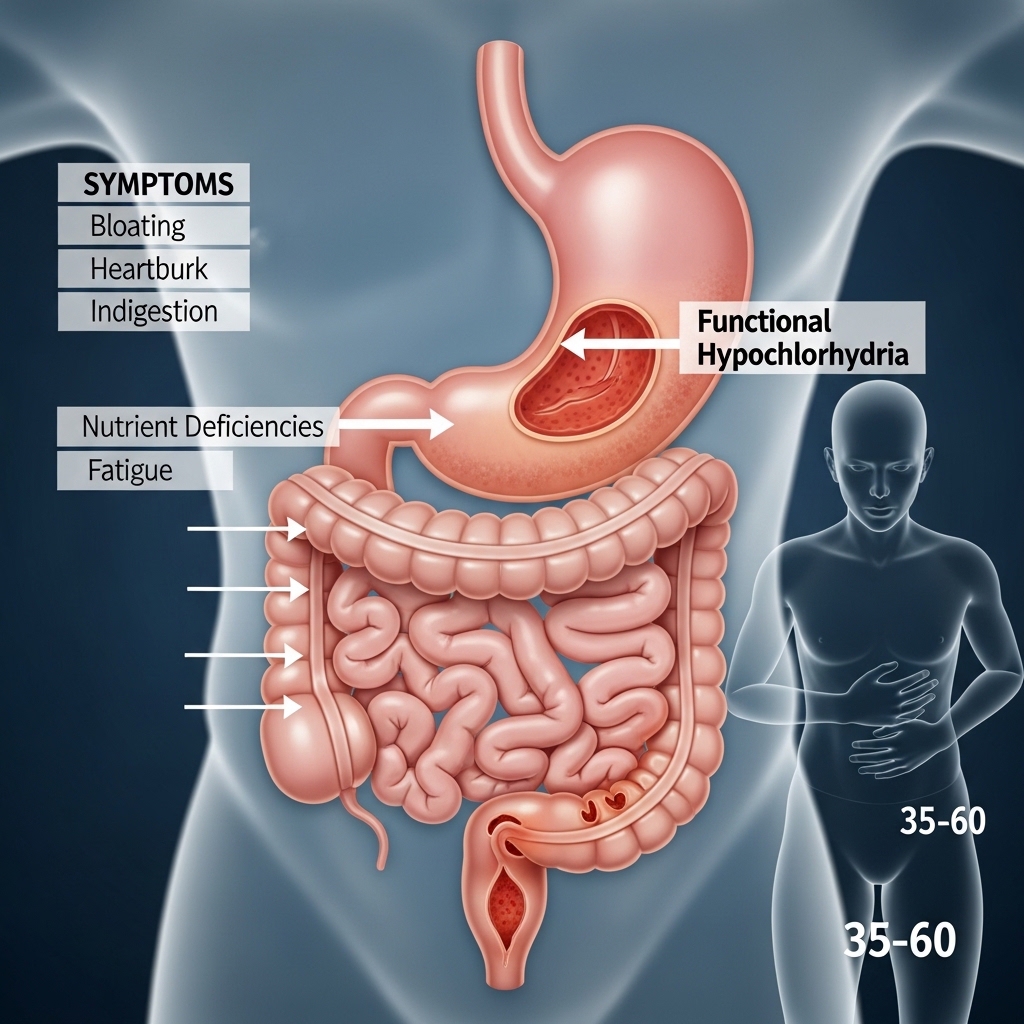
As professionals reach their 40s and 50s, the body often produces less stomach acid, a condition called hypochlorhydria. This change means meals that used to be fine now cause heaviness and bloating. The stomach’s ability to kill germs in food also drops, raising the risk of bacterial overgrowth in the small intestine.
Low stomach acid stops the body from breaking down proteins and absorbing vital nutrients like B12, magnesium, and zinc. These nutrients are required for energy production, DNA repair, and a strong immune system. Missing these building blocks, even with a good diet, creates a hidden barrier to peak performance and a long life.
Lack of acid also means enzymes like pepsin do not activate properly to digest protein. This leads to large, undigested food particles moving into the intestine where they trigger immune reactions and inflammation. For the professional, fixing low stomach acid is essential to turn food into real biological energy.
Cardiovascular Implications of Chronic Gastric Distress
New research shows a “gastrocardiac” link where gut swelling and inflammation can cause heart rhythm issues or blood pressure shifts. For those focused on heart health, ignoring gut pain might mean missing a hidden cause of cardiac strain. A bloated stomach can even put physical pressure on the diaphragm and the heart's position.
The American Heart Association has noted that inflammation from the gut often overlaps with markers that predict heart disease. Managing gut health is a core part of protecting the heart for those in high-stress roles. Chronic gut inflammation can damage blood vessel linings, which is a primary cause of high blood pressure and other age-related issues.
The stress response from recurring gut pain also releases hormones that tax the heart by raising the heart rate. Over time, these small stresses can hurt overall heart health and lower a person's VO2 max. Protecting the heart requires a broad view that sees the digestive system as a potential source of cardiovascular stress.
Sarcopenia and Protein Assimilation Efficiency
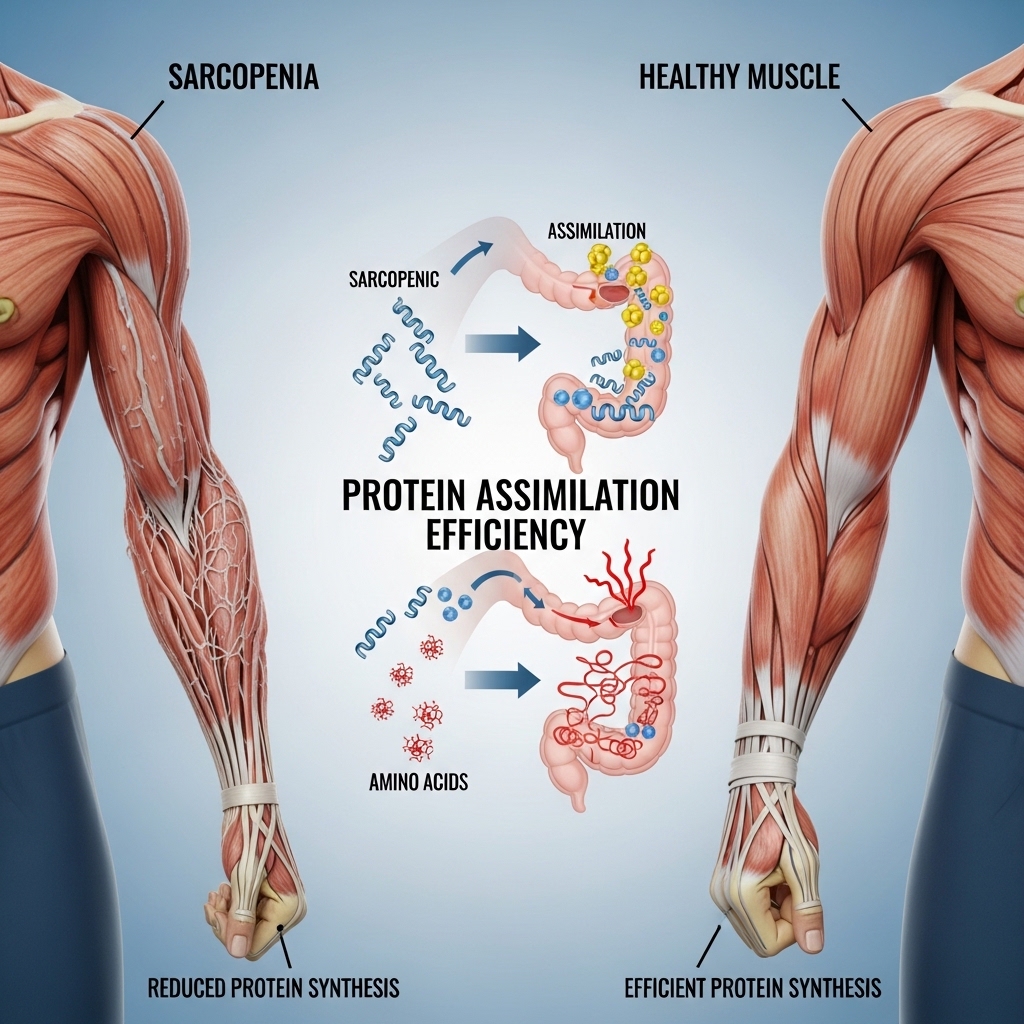
Keeping muscle mass is a main pillar of a long life, but it depends entirely on how well the body uses protein. Professionals with gut pain often eat less protein to avoid discomfort, which leads to a deficit in the amino acids needed for muscle. This avoidance can speed up the loss of lean tissue, which is vital for a healthy metabolism as we age.
If the stomach cannot break down protein correctly, the body does not get the signals it needs to build and maintain muscle. This leads to “functional protein malnutrition,” where a person eats enough protein but their cells cannot use it. Without these building blocks, the body cannot repair itself from hard workouts or daily physical wear and tear.
Low protein absorption also hurts the health of joints and skin, which need amino acids for collagen. For the professional focused on longevity, this can mean a higher risk of injury and faster visible signs of aging. Efficient protein digestion is a must for keeping the body strong and active as the years pass.
READ ALSO: 10 Signs of an Unhealthy Gut You Shouldn’t Ignore
Oxidative Stress and Mitochondrial Performance
Digestion naturally creates some stress, but pain and poor absorption make the body produce too many harmful free radicals. These radicals damage mitochondria, the “power plants” of the cells that drive professional performance. When these power plants are damaged, energy levels drop and markers of cellular aging begin to rise.
Research from the Framingham Heart Study suggests that systemic oxidative stress is linked to faster cellular aging and chronic disease. By fixing the root causes of post-meal pain, a professional reduces this internal “friction” and allows for better energy production. Lowering this stress is critical for protecting high-demand tissues like the heart and the brain.
Damaged mitochondria also signal the immune system to stay active, leading to a state of “inflammaging.” This cycle of damage and inflammation can shorten a professional's healthy years and reduce their ability to work. Optimizing gut function helps clear out this internal debris and keeps cellular energy high.
Diagnostic Precision and Biomarker Tracking
For the high-performing professional, a data-driven approach to gut health goes beyond just tracking symptoms. Using advanced tests like fecal calprotectin can measure gut inflammation, while breath tests can check for bacterial overgrowth. These metrics create a clinical map that allows for precise fixes rather than general wellness advice.
Continuous glucose monitors (CGM) are another tool to see how the body reacts to specific foods. This data helps move from managing symptoms to optimizing the body’s performance. By measuring the gut’s response, a professional can tailor their lifestyle to ensure their diet supports long-term health goals.
Regular blood tests for markers like hs-CRP and insulin can show how gut health affects the whole body. Combining these data points allows for a sophisticated level of health management. Precision diagnostics take the guesswork out of nutrition, giving the professional the same control over their body that they have in their career.
Evidence-Based Strategies for Physiological Optimization

Fixing post-meal distress requires a plan that restores balance to the nervous system and enzymes. High-performing professionals can start with “cephalic phase” activation—using deep breathing before eating to trigger the body's natural acid production. Monitoring heart rate variability (HRV) can also help identify the best times to eat when the body is ready to digest.
Research suggests that the order of food matters; eating greens and proteins before carbs can lower blood sugar spikes and gut pain. Working with a clinical team to test for food sensitivities and checking stomach acid levels are the standard for long-term mental and physical health. These steps ensure that the body is absorbing the fuel it needs for high-level output.
Finally, a short walk after a meal can help the body move food through the system and improve blood sugar. These small, consistent changes can lead to better mental clarity and better health markers over time. By treating digestion as a high-performance system, an executive can turn every meal into a tool for a longer, healthier life.
UP NEXT: Probiotics for Leaky Gut: A Natural Fix
Persistent postprandial distress and the systemic inflammation it triggers are clinically linked to accelerated cellular senescence, often adding several years to an individual's biological age through sustained oxidative stress. WholeLiving's Biological Age Estimation Model incorporates this factor directly — your assessment takes under five minutes.
Ready to understand how these factors are influencing your biological age right now? [Take the Biological Age Assessment →]






