Chronic overactivation of the temporal lobe — the region governing memory consolidation, auditory processing, and emotional regulation — is measurably compressing cognitive longevity in high-output professionals. For executives operating under sustained decision load, this overactivation drives dysregulation of the hypothalamic-pituitary-adrenal axis, elevating baseline cortisol and accelerating hippocampal volume loss at rates clinically associated with early-onset cognitive decline. The temporal brain does not simply process experience; it encodes the biological cost of how you think. When that cost goes unmanaged, the consequences register not as burnout, but as structural neurological change.
1. The Temporal Lobe as a Biological Performance System
The temporal lobe is situated on the lateral surface of each cerebral hemisphere, just behind the frontal lobe and below the parietal lobe. Its location allows it to have direct communication with the limbic system, which is responsible for emotions and memory, and the prefrontal cortex, where executive decision-making occurs. This connectivity is vital for professionals, as it helps manage cognitive processes during high-stakes decisions and stressful meetings.
For high-performing professionals, the temporal brain plays a critical role. Every decision, strategic conversation, and unresolved issue actively engages neural networks that influence emotional and cognitive health. These brain processes come with measurable impacts on performance and mental resilience, particularly when faced with challenges that require immediate action or deep analysis.
The dual role of the temporal lobe — processing information while being vulnerable to stress — underscores why maintaining its function is crucial for professionals. Each cognitive load has biological costs that affect decision-making and mental sharpness, making it essential for executives and leaders to understand the biological dynamics at play.
2. Dual Role of the Temporal Brain: Processing Hub and Vulnerability Point

The temporal brain serves as both a processing center and a vulnerable point for stress. Within it, the hippocampus plays a pivotal role in memory and emotion regulation. However, it is also highly sensitive to stress, as it has a large number of glucocorticoid receptors, making it vulnerable to cortisol-driven damage during periods of chronic stress.
Research has shown that the hippocampus is one of the most stress-sensitive areas of the brain. When cortisol levels rise continuously due to sustained mental strain, the hippocampal neurons are at risk of atrophy. This can lead to cognitive dysfunction, affecting memory retrieval, emotional regulation, and decision-making, all of which are critical for executives under pressure.
Understanding this vulnerability is essential for professionals to manage mental load effectively. The ability to preserve hippocampal integrity can significantly impact cognitive longevity, making it a key focus for those who wish to perform at high levels consistently over time.
3. High Cognitive Demand and Its Impact on the Temporal Brain

When professionals face high cognitive demands for long periods without adequate recovery, the temporal lobe experiences persistent activation. This is not the productive engagement of a flow state but a form of dysregulated activity that leads to oxidative stress at the cellular level. This form of stress impairs brain function over time, resulting in a range of cognitive issues.
Neuroimaging studies have shown measurable changes in temporal lobe gray matter density in individuals exposed to chronic stress. These changes are visible in brain scans and reflect the long-term effects of cognitive overload. The implications are significant for high-level decision-making, as these brain areas directly impact memory retrieval, auditory processing, and emotional decision-making.
For executives and high-level professionals, the consequences of sustained cognitive overload are not theoretical. They result in slower recall under pressure, a diminished ability to read interpersonal dynamics, and poorer overall decision quality as the day progresses. This makes managing cognitive load a critical skill for long-term professional success.
4. Stress, Cortisol, and the Hippocampus
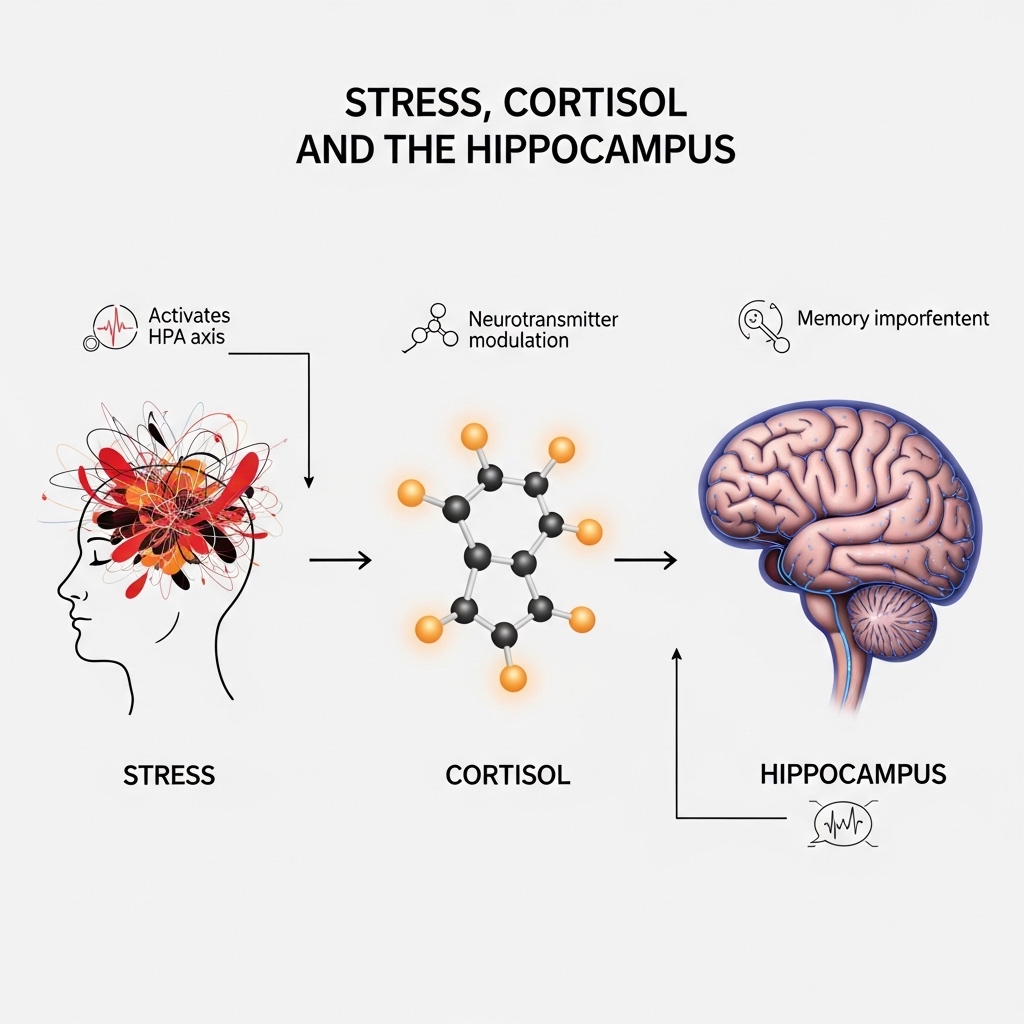
The relationship between stress and the hippocampus is particularly important. Chronic stress elevates cortisol levels, which in turn can cause significant damage to hippocampal neurons. Studies show that prolonged exposure to high cortisol can lead to accelerated hippocampal volume loss, a phenomenon that negatively impacts memory, spatial awareness, and emotional regulation.
This volume loss has serious consequences. A smaller hippocampus is linked to cognitive issues such as memory impairment and poor decision-making. It also increases vulnerability to mental health conditions like anxiety and depression. For professionals, this means that excessive stress can diminish the very cognitive abilities needed to perform effectively in high-pressure environments.
The impact of cortisol-driven hippocampal damage is compounded as professionals age. For those in their 40s and 50s, hippocampal shrinkage accelerates, leading to faster cognitive decline. By understanding this, executives can take proactive measures to reduce stress and protect their cognitive health, which is essential for sustained performance throughout their careers.
READ ALSO: Parietal Brain: How It Shapes Focus and Awareness
5. The Effects of Cortisol on Professional Performance

Cortisol’s impact on professional performance goes beyond memory issues. Chronic stress causes sustained high cortisol levels, which can degrade overall brain function. This leads to faster cognitive aging, which is particularly noticeable in high-performing professionals who manage complex decisions on a daily basis.
The loss of hippocampal volume due to prolonged cortisol exposure leads to quicker cognitive decline than what would be expected from normal aging alone. This is especially relevant for professionals in midlife, as their cognitive performance may decrease faster than they anticipate. High decision load, poor sleep, and social demands all contribute to the acceleration of this process.
The clinical implications for high-level professionals are clear. The effects of sustained cortisol release on cognitive performance aren’t just about memory loss; they encompass overall decision-making, emotional regulation, and cognitive flexibility, all of which are essential in executive roles. Managing these stressors effectively can preserve cognitive function and performance in the long term.
READ ALSO: Signs of a Brain Tumor: What to Notice Early
6. The Role of Sleep in Temporal Brain Recovery

Sleep is a critical component of temporal lobe recovery, yet it is often the first thing professionals sacrifice during busy periods. The relationship between sleep and the temporal brain is vital for memory consolidation and overall cognitive health. During slow-wave sleep, the hippocampus consolidates new memories, preparing the brain for the next day’s challenges.
When sleep is disrupted — whether by stress, irregular hours, or time zone differences — the consolidation process is incomplete. This results in impaired memory, reduced pattern recognition, and weakened verbal memory. These effects are particularly noticeable in professionals who must perform under pressure, as their ability to recall important information and make decisions decreases.
Chronic sleep deprivation creates a feedback loop that worsens cognitive function. Poor sleep leads to diminished hippocampal function, which in turn leads to higher emotional reactivity and impaired decision-making. This loop can be broken by prioritizing sleep quality, as it directly impacts cognitive performance the following day.
7. The Impact of Neuroinflammation on the Temporal Brain
Neuroinflammation, or chronic low-grade inflammation within the brain, accelerates the structural decline of the temporal lobe. Inflammatory markers like CRP and IL-6 have been associated with decreased gray matter volume in the temporal and prefrontal regions, which affects overall cognitive function.
For high-performing professionals, neuroinflammation is a result of various factors, including poor sleep, unhealthy diets, and chronic psychological stress. These factors contribute to an inflammatory burden that negatively impacts brain health. Over time, this leads to impaired decision-making, memory, and emotional regulation, all of which are vital for effective leadership.
Managing neuroinflammation involves addressing lifestyle factors such as diet, exercise, and stress management. By tracking inflammatory markers and making targeted changes, professionals can preserve brain function and reduce the risk of cognitive decline.
READ ALSO: Emotional Brain Training Practices to Lift Your Mood Daily
8. Cardiovascular Fitness and Brain Health

Cardiovascular fitness plays a crucial role in preserving temporal lobe health. Research has shown that higher levels of cardiovascular fitness are associated with greater hippocampal volume and better cognitive function. Regular aerobic exercise improves cerebral blood flow, allowing for better oxygen and glucose delivery to brain tissue.
Higher VO2 max, which is a measure of aerobic fitness, has been directly correlated with hippocampal volume in adults between the ages of 35 and 65. This correlation suggests that physical fitness not only benefits heart health but also plays a key role in maintaining cognitive performance, particularly in high-stakes professional environments.
For professionals in midlife, cardiovascular fitness is a protective factor against cognitive decline. By maintaining regular aerobic exercise, they can preserve hippocampal function and cognitive performance, which are essential for long-term professional success and brain health.
9. Default Mode Network Interference and Cognitive Performance

The Default Mode Network (DMN) is active during rest and self-referential thinking. It involves key components of the temporal lobe, and its interference with task-focused cognitive activities is a major challenge for professionals with high cognitive loads. Functional MRI research has shown that the DMN fails to deactivate properly, leading to interference that reduces cognitive efficiency.
This interference occurs when professionals are unable to fully disconnect from their thoughts, resulting in decreased task performance and decision-making accuracy. For high-level executives, the inability to properly switch between tasks and contexts is a significant performance bottleneck. The result is slower cognitive switching and less effective decision-making.
To counteract DMN interference, professionals need structured periods of cognitive rest. These breaks allow for the normalization of the DMN, which is necessary for maintaining cognitive flexibility and high-level performance. Resting the brain isn’t a withdrawal; it’s an essential input for sustained professional success.
READ ALSO: Left Brain vs Right Brain: How Both Sides Work Together
10. Structured Cognitive Rest: A Key to Preserving Brain Function

Structured cognitive rest is a vital component of maintaining high-level performance. The temporal brain needs regular low-demand periods to clear synaptic buildup, consolidate memories, and normalize the DMN. Professionals who fail to incorporate these breaks into their schedules risk eroding their cognitive function over time.
The evidence is clear: brain function deteriorates when professionals are consistently overloaded without proper rest. Taking time for structured cognitive rest helps prevent burnout, improves decision-making, and preserves long-term cognitive health. High-level performers need to view rest as an active investment in their performance, rather than a passive break.
Incorporating structured cognitive rest is a key strategy for maintaining mental resilience. Professionals who prioritize rest, alongside managing stress, sleep, and exercise, can sustain their cognitive function and improve performance in high-stakes environments over time.
UP NEXT: The Gut-Brain Axis Shapes Executive Decision-Making and Emotional Resilience Under Pressure
Chronic stress and poor sleep significantly affect the temporal brain, accelerating cognitive aging and increasing biological age. WholeLiving's Biological Age Estimation Model incorporates this factor directly — your assessment takes under five minutes.
Ready to understand how these factors are influencing your biological age right now? [Take the Biological Age Assessment →]






