Enteric nervous system dysfunction is increasingly documented in high-performing professionals under chronic stress. It directly compromises the gut-brain axis. This disrupts serotonin synthesis and impairs the bidirectional signaling governing emotional regulation and executive decision-making. For founders and senior leaders, a dysregulated gut microbiome extends beyond digestion. It manifests as elevated neuroinflammation, degraded cognitive clarity, and measurable declines in stress resilience. Those managing complex, high-stakes environments depend on judgment and emotional precision. Understanding this axis is no longer optional.
The Enteric Nervous System: A Second Command Center
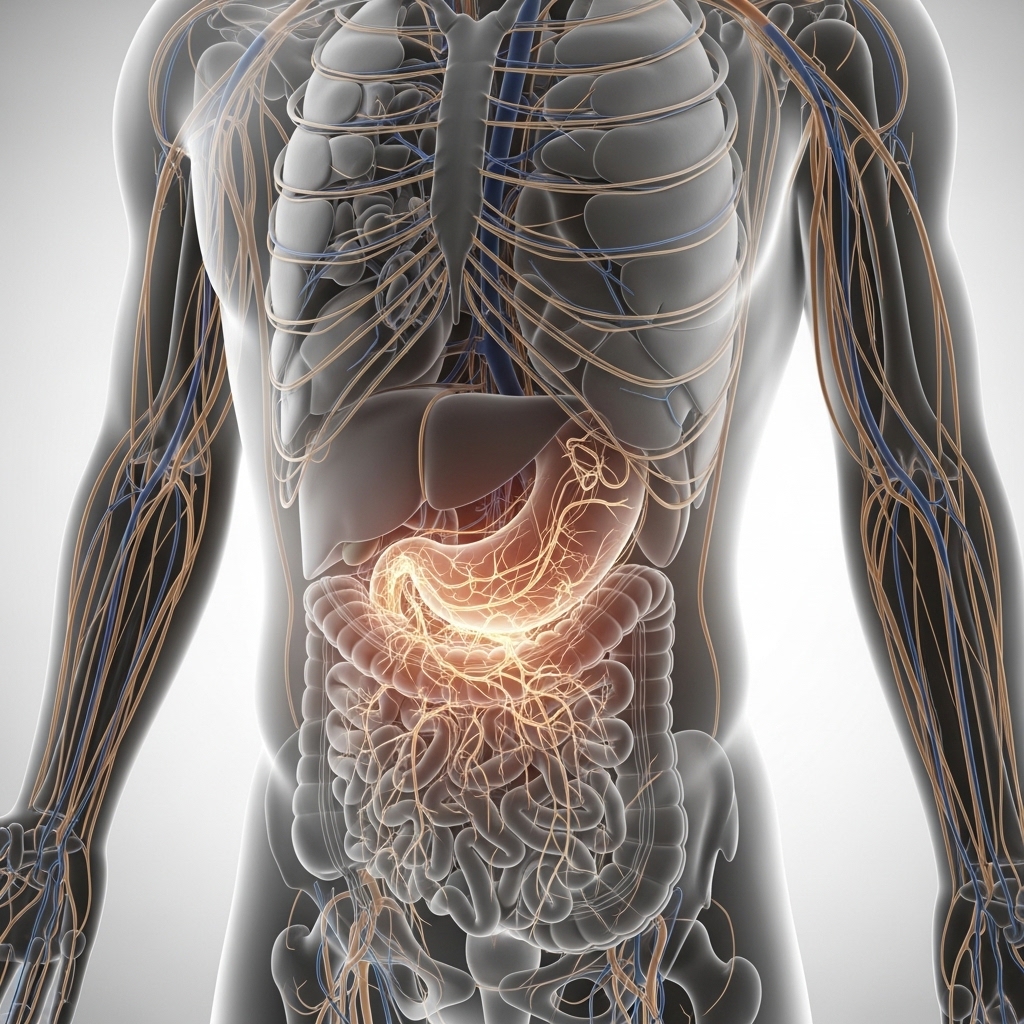
The gut contains an estimated 200 to 500 million neurons — a range reflecting variability across anatomical studies. These neurons form the enteric nervous system (ENS), an extensive neural network embedded in the gastrointestinal tract wall. The ENS operates with considerable independence from the central nervous system. It regulates digestion, monitors the gut environment, and generates signals that travel directly to the brain. Researchers, consequently, refer to it as the body's second brain — not as a metaphor, but as a functional description.
The ENS communicates with the central nervous system primarily through the vagus nerve. This bidirectional highway carries information in both directions. Based on anatomical studies of vagal fiber composition, a substantial majority of vagal fibers — estimated at roughly 80 percent in most referenced research — carry afferent signals from the body's organs, including the gut, upward to the brain. The brain, therefore, receives considerable bottom-up information through this channel. This asymmetry has significant implications for how professionals understand mood, cognition, and decision-making.
Beyond neural signaling, the ENS also produces and responds to a wide range of neurotransmitters. It manufactures acetylcholine, serotonin, dopamine precursors, and GABA — all of which influence gut and brain function. This production capacity makes the gut a neurochemically active organ, not merely a digestive one. Understanding this reframes gut health as a cognitive and emotional performance variable, not a secondary concern addressed only when symptoms appear.
Serotonin, the Gut, and Emotional Regulation

Serotonin receives considerable attention as a brain chemical linked to mood stability. What receives far less attention, however, is where most of it originates. Approximately 90 to 95 percent of the body's serotonin resides in the gastrointestinal tract, where enterochromaffin cells synthesize it in response to luminal stimuli — food, microbiota metabolites, and mechanical pressure. This peripheral serotonin pool plays a central role in gut motility and local ENS signaling.
A critical qualification applies here. Peripheral gut serotonin does not cross the blood-brain barrier. It therefore does not directly enter the brain to regulate mood. Its influence on emotional states operates indirectly — through vagal afferent signaling, local ENS modulation, and systemic effects that interact with central serotonergic systems. The gut-mood connection through serotonin is real, but the mechanism is more indirect than popular accounts suggest.
For high-performing professionals, this distinction matters practically. Disruptions in gut serotonin synthesis — driven by microbiome imbalance, chronic stress, or dietary insufficiency — alter the gut-brain signaling environment in ways that can influence mood, anxiety thresholds, and stress reactivity. Addressing gut health, therefore, remains a relevant variable in any serious framework for sustained emotional performance. The mechanism, however, operates through systems-level signaling rather than direct neurochemical transfer.
The Gut Microbiome as a Neuroactive Ecosystem

The human gut hosts trillions of microorganisms collectively referred to as the gut microbiome. This ecosystem actively produces neuroactive compounds — including short-chain fatty acids, gamma-aminobutyric acid (GABA), and serotonin precursors — that influence brain function and behavior. The microbiome, consequently, functions less like a passive digestive assistant and more like an active participant in neurological regulation.
Research supported by the NIH Human Microbiome Project, along with studies published across microbiome and psychiatric research literature, has expanded the understanding of how microbial diversity correlates with neurological and psychological outcomes. Reduced microbial diversity associates with higher rates of anxiety, depression, and cognitive impairment across multiple study populations. The directionality, however, is not fully resolved — stress also degrades microbial diversity, creating a feedback loop that research continues to characterize.
For mid-life executives operating under sustained occupational pressure, this feedback loop carries measurable risk. Chronic stress reduces microbiome diversity. Reduced diversity impairs neuroactive compound production. Impaired neurochemistry, in turn, may degrade emotional resilience and decision quality. Breaking this cycle requires addressing the gut environment as a direct component of cognitive performance strategy — not as an afterthought managed through occasional dietary adjustments.
READ ALSO: Emotional Damage: Understanding and Healing with Care
Gut Permeability, Neuroinflammation, and Cognitive Performance

Intestinal permeability describes a condition in which the gut lining loses structural integrity. When this occurs, bacterial endotoxins and other luminal contents cross into systemic circulation. The immune system responds with inflammatory signaling. This inflammation, critically, does not remain confined to the gastrointestinal tract. Research suggests it can contribute to neuroinflammatory processes, though the precise mechanisms and clinical thresholds in otherwise healthy adults remain an active area of investigation.
Neuroinflammation associates with impaired cognitive performance across multiple research lines. It reduces processing speed, degrades working memory, and disrupts prefrontal regulatory systems responsible for executive decision-making. Research published in Brain, Behavior, and Immunity links markers of systemic inflammation — including those associated with gut barrier dysfunction — to neuroinflammatory activity and cognitive deficits in adult populations. The specific biomarker relationships, however, vary across studies and populations.
For professionals who experience persistent cognitive fog, reduced decisional clarity, or unexplained mood instability, gut permeability represents an underexamined variable worth investigating through comprehensive functional health assessment. Standard cognitive evaluations do not assess it directly. Addressing gut permeability through dietary, lifestyle, and stress-reduction interventions may produce cognitive benefits, though the evidence base for specific intervention protocols in healthy high-performing adults remains developing.
The Vagus Nerve as a Performance Variable

The vagus nerve functions as the primary communication channel between the gut and the brain. Its tone — the degree to which it actively engages parasympathetic signaling — determines much of the body's capacity for stress recovery, emotional regulation, and inflammatory control. High vagal tone associates with greater resilience, faster physiological recovery, and more stable emotional states. Low vagal tone, by contrast, correlates with chronic stress reactivity, impaired gut function, and elevated inflammatory markers across multiple research cohorts.
Vagal tone is not fixed. Peer-reviewed research in autonomic neuroscience demonstrates that vagal tone responds to targeted interventions. Slow diaphragmatic breathing, aerobic exercise, and certain cold exposure protocols show associations with measurable vagal tone improvements in controlled studies. These interventions, therefore, directly engage the gut-brain communication pathway — not merely the nervous system in abstract terms.
For high-performing professionals, vagal tone represents a tractable performance variable. It links gut health, stress physiology, emotional regulation, and cognitive performance within a single measurable system. Heart rate variability provides a practical proxy measure for vagal tone and autonomic function. Professionals who already track HRV for recovery purposes are, consequently, already monitoring a key indicator of gut-brain axis function — whether or not they recognize it in those terms.
Cortisol, Stress Physiology, and Gut Function

Chronic stress dysregulates the gut-brain axis through multiple pathways simultaneously. Elevated cortisol increases intestinal permeability, alters gut motility, and suppresses the diversity and activity of the gut microbiome. These changes, in turn, reduce the gut's capacity to produce neuroactive compounds and maintain stable upward signaling to the brain. The result is a stress-induced degradation of the very system that participates in stress regulation.
This bidirectional relationship creates compounding vulnerability. A stressed gut produces fewer stabilizing neurochemicals. Fewer stabilizing neurochemicals may amplify the brain's stress response. An amplified stress response generates more cortisol. The cycle, therefore, does not self-correct without deliberate intervention. Research across psychoneuroimmunology consistently documents associations consistent with this pattern — particularly in populations experiencing sustained occupational or psychological pressure.
For executives and founders, recognizing this cycle reframes the relationship between stress management and gut health. Managing cortisol load is not only a neurological or cardiovascular intervention. It simultaneously affects gut microbiome composition, gut permeability, and the signaling environment for serotonin synthesis. Addressing stress physiology at its source, consequently, produces downstream effects across the gut-brain system — effects that targeted gut supplements or dietary changes alone are unlikely to fully replicate.
READ ALSO: Mindfulness Practices for Burnout: Simple Ways to Recover
Decision-Making and the Gut Signal

The concept of a gut feeling carries more physiological precision than the phrase suggests. The body generates interoceptive signals — internal sensory information from organs, muscles, and the gut — that the brain integrates into decision-making processes. Neuroscientist Antonio Damasio's somatic marker hypothesis proposes that the brain relies on body-based signals to guide decisions under uncertainty. This remains an influential and widely cited theoretical framework, though aspects of it continue to be tested and debated in the cognitive neuroscience literature.
Interoceptive accuracy — the ability to perceive and correctly interpret internal body signals — shows associations with decision quality, particularly in high-stakes, time-pressured environments. Research across cognitive neuroscience literature links higher interoceptive sensitivity to performance on risk assessment tasks and emotional regulation under pressure. These associations are consistent across multiple studies, though individual variability is substantial and the field continues to refine its measurement approaches.
Chronic gut dysfunction may degrade interoceptive clarity. When the gut generates dysregulated signals — driven by microbiome imbalance, inflammation, or permeability — the brain may receive distorted interoceptive input. Decision-making under these conditions can become less reliable, not necessarily because of discrete cognitive deficits, but because the body-based signal system that supports judgment has been compromised. Restoring gut health, as a result, represents a plausible pathway for supporting the quality of executive decision-making, though direct clinical evidence in professional populations remains limited.
Inflammatory Markers, the Gut, and Biological Age

The gut plays a central role in systemic inflammatory regulation. A healthy gut lining and a diverse microbiome actively suppress pro-inflammatory signaling. A compromised gut, conversely, contributes to the chronic low-grade inflammation increasingly recognized as a primary mechanism of biological aging — a process researchers term inflammaging. This process associates with accelerated cellular wear, impaired mitochondrial function, and degraded tissue integrity across multiple organ systems.
Elevated inflammatory markers — including C-reactive protein, IL-6, and TNF-α — associate with both gut dysbiosis and accelerated biological age across longitudinal research cohorts. NIH-affiliated research programs studying aging have increasingly examined gut microbiome composition as a contributor to inflammatory aging trajectories, though the field continues to characterize the relative magnitude of this contribution against other variables. This places gut health within the biological age management framework as a relevant, if not yet fully quantified, variable.
For professionals in their late thirties through fifties, this connection represents a meaningful intervention window. The inflammatory trajectory established during this period influences cognitive health, cardiovascular risk, and metabolic function in the decades that follow. Addressing gut-driven inflammation during this window, therefore, offers leverage that becomes progressively more difficult to achieve later. Gut health, in this context, extends well beyond digestive function — it operates as a longevity variable with systemic reach.
READ ALSO: Pause & Breathe: Your Daily Mindfulness Practice
Sleep Quality and the Gut-Brain Overnight Relationship

The gut-brain axis does not rest during sleep. The microbiome follows circadian rhythms that align with the body's sleep-wake cycle. Disrupted sleep associates with changes in microbiome composition and reduced microbial diversity. A less diverse microbiome, in turn, may impair the overnight neurochemical and inflammatory regulation that healthy sleep depends on. Research in this area, however, continues to develop, and causal directionality between specific microbiome changes and sleep architecture outcomes has not been fully established.
Research published in Cell Host and Microbe — including work by Eran Segal and colleagues — documents circadian oscillations in gut microbial populations and links circadian disruption to measurable microbiome composition changes. Circadian misalignment, common in executives managing global teams or irregular schedules, associates with microbiome disruption and impaired serotonin signaling. The downstream effects on sleep architecture represent an active area of ongoing research rather than a fully resolved mechanistic pathway.
For high-performing professionals managing demanding schedules, this gut-sleep interaction represents an underrecognized variable in sleep optimization strategies. Improving sleep hygiene variables without addressing gut microbiome health may produce limited results when underlying dysbiosis contributes to disrupted overnight neurochemical regulation. Treating the gut-sleep relationship as a systems problem, rather than addressing either variable in isolation, offers a more complete investigative framework.
Metabolic Function and Gut-Brain Signaling
The gut-brain axis also participates in metabolic regulation. Gut-derived hormones — including GLP-1, ghrelin, and peptide YY — signal satiety, energy availability, and metabolic state to the brain. These signals influence appetite regulation, glucose metabolism, and energy expenditure. When gut-brain axis function is compromised, the precision of these hormonal signals may degrade, potentially contributing to disrupted energy balance — though the degree to which this occurs in otherwise healthy adults under occupational stress has not been precisely quantified.
Chronic stress and gut dysbiosis both associate with impaired production and signaling of these metabolic hormones. NIH-affiliated metabolic research programs link gut microbiome composition to insulin sensitivity and metabolic risk variables across multiple study designs. Dietary intake and other lifestyle factors, however, represent significant confounders in this literature, and the independent contribution of microbiome composition to metabolic outcomes continues to be characterized.
For executives who maintain structured nutrition and exercise protocols but observe persistent metabolic resistance, gut-brain axis dysfunction represents a plausible and frequently underexamined contributing variable. Addressing microbiome health, reducing gut permeability, and restoring vagal tone may support metabolic outcomes — though the evidence base for this as a standalone intervention in healthy professionals is still developing. The gut-brain metabolic signal system, when functioning well, participates in the metabolic regulation that professionals work to optimize through conventional means.
Evidence-Based Options for the High-Performing Professional

The research base on the gut-brain axis supports several evidence-informed approaches for professionals seeking to engage this system. Dietary strategies that support microbial diversity — including increased dietary fiber, fermented food consumption, and reduced ultra-processed food intake — show consistent associations with improved microbiome composition across clinical trials, though optimal protocols vary by individual. Vagal tone interventions, including slow diaphragmatic breathing practiced consistently, produce measurable HRV improvements in controlled research. Stress physiology management — addressed through structured recovery practices — directly reduces cortisol-driven microbiome degradation and gut permeability. Consistent circadian alignment in sleep and meal timing supports microbiome rhythmicity. Comprehensive functional health assessments that include gut permeability and microbiome markers provide objective baseline data for individualized decisions. Each represents an evidence-supported entry point, with effect sizes and individual responses varying meaningfully across populations.
UP NEXT: Emotional Brain Training Practices to Lift Your Mood Daily
Disruptions to the gut-brain axis — including chronic gut inflammation, poor microbiome diversity, and dysregulated interoceptive signaling — are associated with elevated cortisol, systemic low-grade inflammation, and impaired autonomic function, all of which are key drivers of accelerated biological aging and can add measurable years beyond your chronological age. WholeLiving's Biological Age Estimation Model incorporates this factor directly — your assessment takes under five minutes.
Ready to understand how these factors are influencing your biological age right now? [Take the Biological Age Assessment →]






