Blunt force trauma imposes measurable physiological costs that extend well beyond the acute injury phase — costs that directly compromise the neuroendocrine stability, sleep architecture, and cognitive performance that high-performing professionals depend on. When the body absorbs significant mechanical force, the resulting HPA axis activation, inflammatory cascade, and autonomic dysregulation do not resolve when the visible injury heals. For executives and founders operating under sustained performance demand, unresolved trauma physiology accelerates allostatic load and introduces compounding risks to long-term biological age trajectories.
The Mechanical Physics of Internal Injury
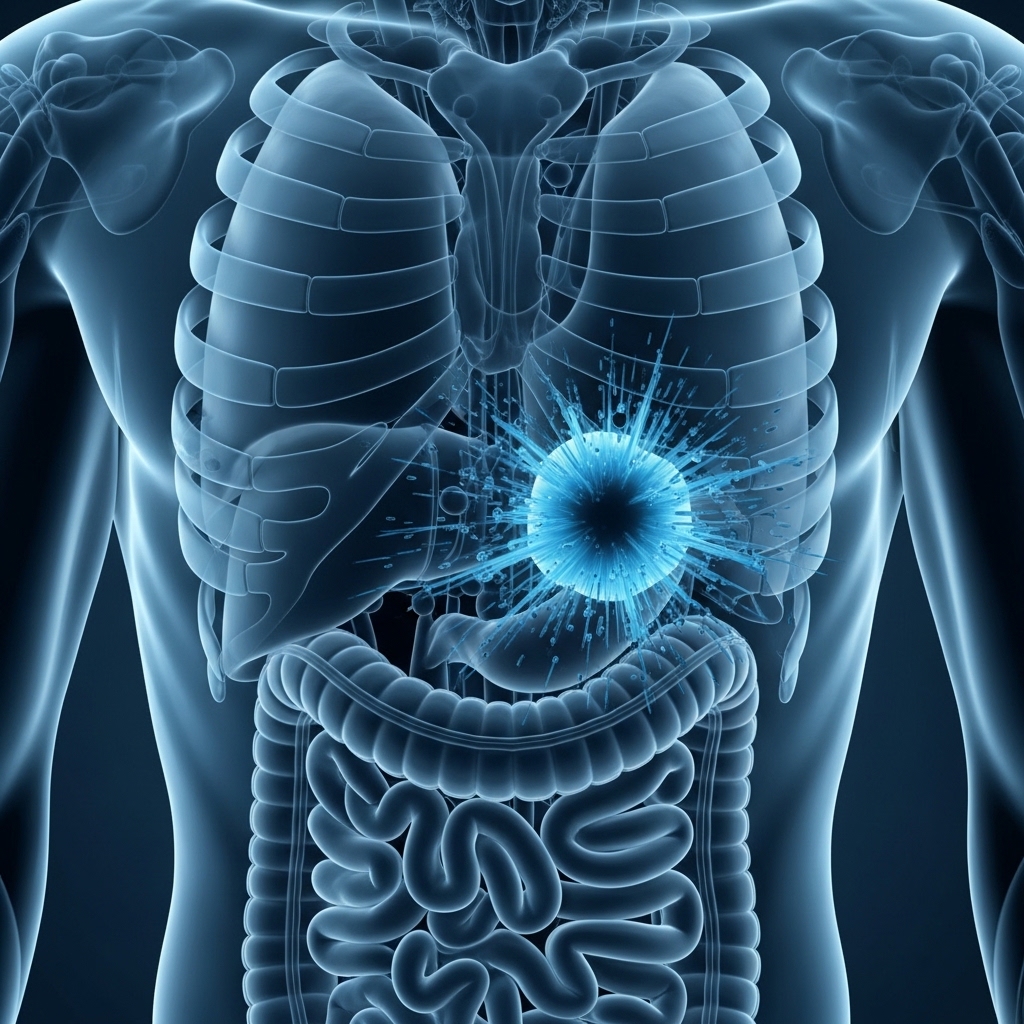
Blunt force trauma occurs when the body absorbs significant mechanical energy without skin penetration. The force travels through tissue layers, compressing, stretching, and shearing structures beneath the surface. Organs, blood vessels, and connective tissue absorb this energy in ways that external assessment cannot fully capture.
The physics of rapid deceleration explain why motor vehicle collisions produce such complex internal injury patterns. The body stops, but internal structures continue moving briefly. That differential motion creates internal shear forces capable of disrupting vascular integrity, organ positioning, and connective tissue alignment — often without producing visible external marks.
Research published in the Journal of Trauma and Acute Care Surgery consistently documents the gap between external presentation and internal injury severity. Professionals who appear functionally stable immediately post-impact frequently present with delayed symptom onset as swelling and inflammatory processes develop over the subsequent 24 to 72 hours.
How the Body's Stress Response Activates Immediately

The body interprets mechanical trauma as an acute survival threat. Within seconds of impact, the hypothalamic-pituitary-adrenal axis activates. Cortisol and adrenaline surge. Heart rate and blood pressure elevate. Inflammatory cytokines mobilize to the injury site.
This response is biologically intelligent in the short term. It prioritizes immediate tissue protection and pain suppression. However, the same cascade that protects acutely becomes a source of systemic dysregulation when it fails to resolve. Elevated cortisol that persists beyond the acute phase suppresses immune function, degrades sleep architecture, and impairs cognitive performance.
The National Institutes of Health has documented extensively how sustained HPA axis activation — regardless of whether the original stressor is physical or psychological — produces equivalent downstream consequences. For a high-performing professional, a trauma event that keeps cortisol chronically elevated does not simply cause physical discomfort. It introduces measurable performance and longevity costs.
Inflammatory Cascade and Its Systemic Reach
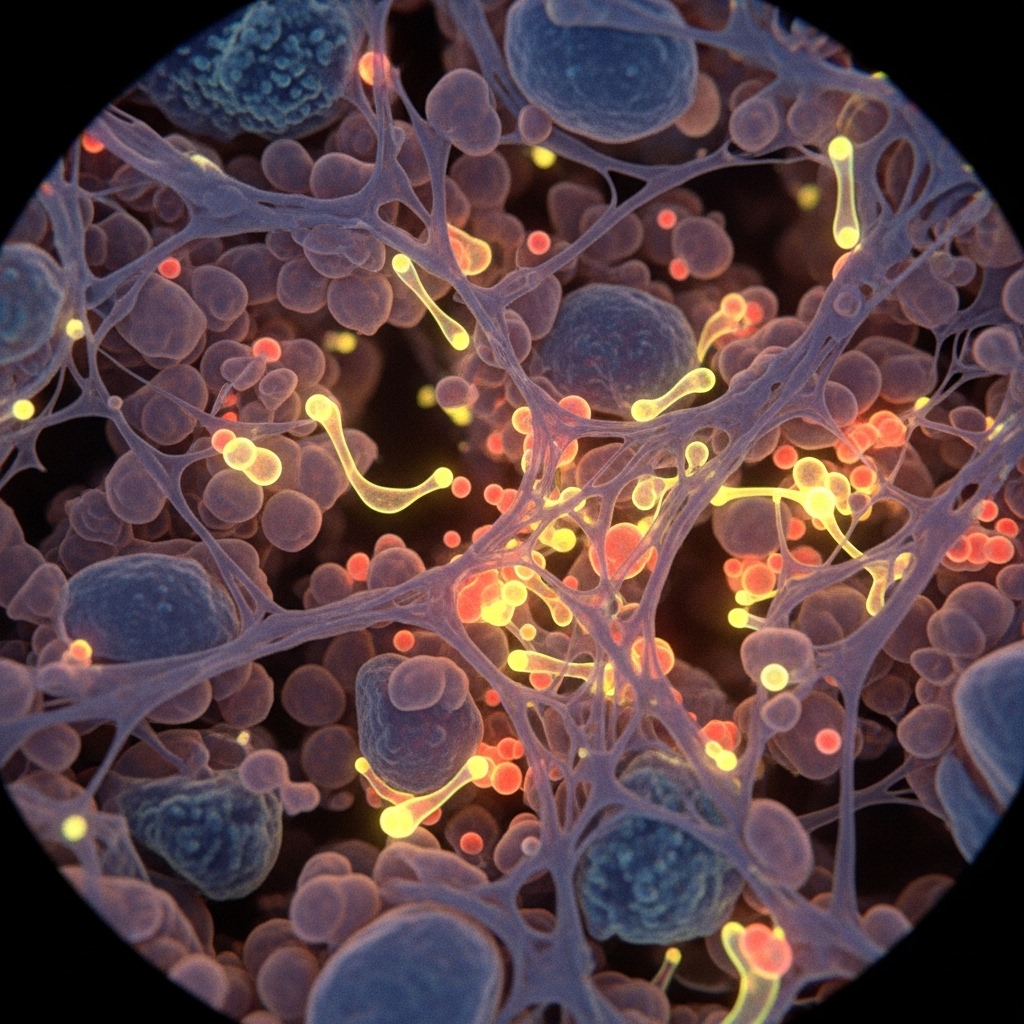
Inflammation serves as the body's primary repair mechanism following tissue injury. Pro-inflammatory cytokines, including interleukin-6 and tumor necrosis factor-alpha, mobilize to damaged regions. They signal immune cells to clear debris and initiate tissue repair. This process is necessary and, under normal circumstances, self-limiting.
The problem arises when the inflammatory response becomes chronic. Sustained cytokine elevation extends well beyond the local injury site. It crosses systemic barriers and affects neurological function, hormonal regulation, and cardiovascular stability. Research from the Harvard T.H. Chan School of Public Health links chronic low-grade inflammation directly to accelerated biological aging and increased cardiovascular risk in midlife adults.
For professionals in the 35 to 60 age range, this connection carries direct relevance. A trauma event that triggers unresolved systemic inflammation does not simply slow physical recovery. It contributes to the cumulative inflammatory burden that longitudinal research consistently associates with earlier onset of age-related disease and cognitive decline.
READ ALSO: The Role of Emotion Regulation in Reducing Cortisol Levels and Enhancing Cognitive Performance
Autonomic Dysregulation After Physical Trauma

The autonomic nervous system governs the body's baseline regulatory functions — heart rate variability, breathing rhythm, digestive function, and sleep-wake transitions. Blunt trauma disrupts this system by locking the nervous system in a sympathetic-dominant state long after the physical injury resolves.
Heart rate variability serves as one of the most sensitive biomarkers of autonomic function. Research published in journals including Frontiers in Physiology documents that trauma survivors show measurably reduced heart rate variability compared to non-trauma controls — even when the physical injury has clinically resolved. Reduced heart rate variability correlates directly with impaired cardiovascular recovery and reduced stress resilience.
For executives and founders, this matters operationally. Autonomic dysregulation degrades the physiological foundation upon which sustained cognitive performance depends. Decision quality, emotional regulation, and stress tolerance all rely on a nervous system capable of shifting fluidly between activation and recovery states. Trauma disrupts that capacity at a biological level.
Sleep Architecture Disruption and Recovery Interference

Sleep represents the body's primary restoration mechanism. Slow-wave sleep drives tissue repair and hormonal regulation. REM sleep supports memory consolidation and emotional processing. Both stages require a cortisol environment that supports neural downregulation.
Blunt trauma disrupts this environment through the cortisol pathway. Elevated evening cortisol delays melatonin onset, fragments slow-wave sleep, and compresses REM duration. The glymphatic system — the brain's overnight waste-clearance mechanism — depends on slow-wave sleep to function effectively. Disrupted sleep compromises this clearance, allowing metabolic byproducts to accumulate in cortical tissue.
The downstream consequence extends beyond fatigue. Degraded sleep architecture following trauma impairs next-day working memory capacity, increases inflammatory marker levels, and reduces the body's capacity to repair damaged tissue overnight. Recovery from blunt trauma, therefore, depends substantially on restoring sleep quality — not merely on treating the physical injury itself.
READ ALSO: Natural Remedies for Depression: A Gentle, Holistic Approach
Cognitive Performance Consequences of Trauma Physiology

Cognitive performance declines measurably when the physiological environment is destabilized by trauma. Elevated cortisol reduces prefrontal cortical activity, impairing inhibitory control, working memory capacity, and decision-making speed. These are not subjective complaints. They reflect documented neurobiological mechanisms.
The prefrontal cortex is metabolically sensitive. It requires stable glucose availability, regulated cortisol levels, and adequate overnight restoration to maintain peak function. When trauma physiology disrupts any of these inputs, executive function degrades in proportion to the severity and duration of that disruption.
For high-performing professionals, the practical consequence is direct. A trauma event that produces sustained cortisol elevation and fragmented sleep can measurably degrade the cognitive variables that define professional performance — analytical precision, strategic thinking, and interpersonal judgment — weeks beyond the point at which the physical injury appears healed.
The Body's Emotional Memory: Somatic Storage of Trauma

The body stores the physiological signature of traumatic events in muscle tension patterns, breathing habits, and autonomic reactivity. This is not metaphorical. Research from neuroscientists including Bessel van der Kolk, whose work is documented extensively in peer-reviewed literature, demonstrates that traumatic memory encodes in subcortical brain structures — particularly the amygdala — independently of conscious narrative recall.
This encoding produces physiological reactivity to environmental cues associated with the original trauma. The nervous system interprets these cues as renewed threat signals, triggering HPA axis activation in contexts that do not warrant it. The result is a pattern of dysregulated stress response that persists as a functional state even when the original event has resolved.
For professionals, this mechanism carries specific implications. Subcortical trauma encoding can produce sustained sympathetic activation, reduced emotional regulation capacity, and heightened anxiety responses — all of which impair the cognitive and interpersonal performance that executive roles demand.
Biological Age and the Accumulation of Trauma Load

Biological age reflects the cumulative impact of physiological stressors on cellular and organ-level function. Chronic cortisol elevation, sustained neuroinflammation, disrupted sleep, and autonomic dysregulation each independently accelerate biological aging. Blunt trauma that triggers all four mechanisms simultaneously introduces a compounding accelerant into the biological aging trajectory.
Allostatic load — the cumulative physiological cost of adapting to chronic stressors — rises measurably following significant trauma events. Research linking high allostatic load to accelerated telomere shortening, impaired immune regulation, and elevated cardiovascular risk is well-established in the epidemiological literature. These are not remote long-term risks. They represent measurable biological shifts that begin acutely and compound over time.
For a high-performing professional in midlife, the window between chronological and biological age is most responsive to environmental and physiological inputs. An unresolved trauma response that sustains elevated allostatic load during this window adds measurable biological years at a stage when that acceleration carries the greatest long-term consequence.
The cardiovascular system bears significant secondary burden following blunt trauma. Sustained sympathetic nervous system activation elevates resting heart rate, raises blood pressure, and increases myocardial oxygen demand. These effects compound existing cardiovascular risk factors common in high-stress professional demographics.
READ ALSO: Seasonal Trauma Symptom Expression and Its Impact on Cortisol Regulation Sleep Disruption and Cognitive Performance
Cardiovascular Implications of Sustained Trauma Physiology
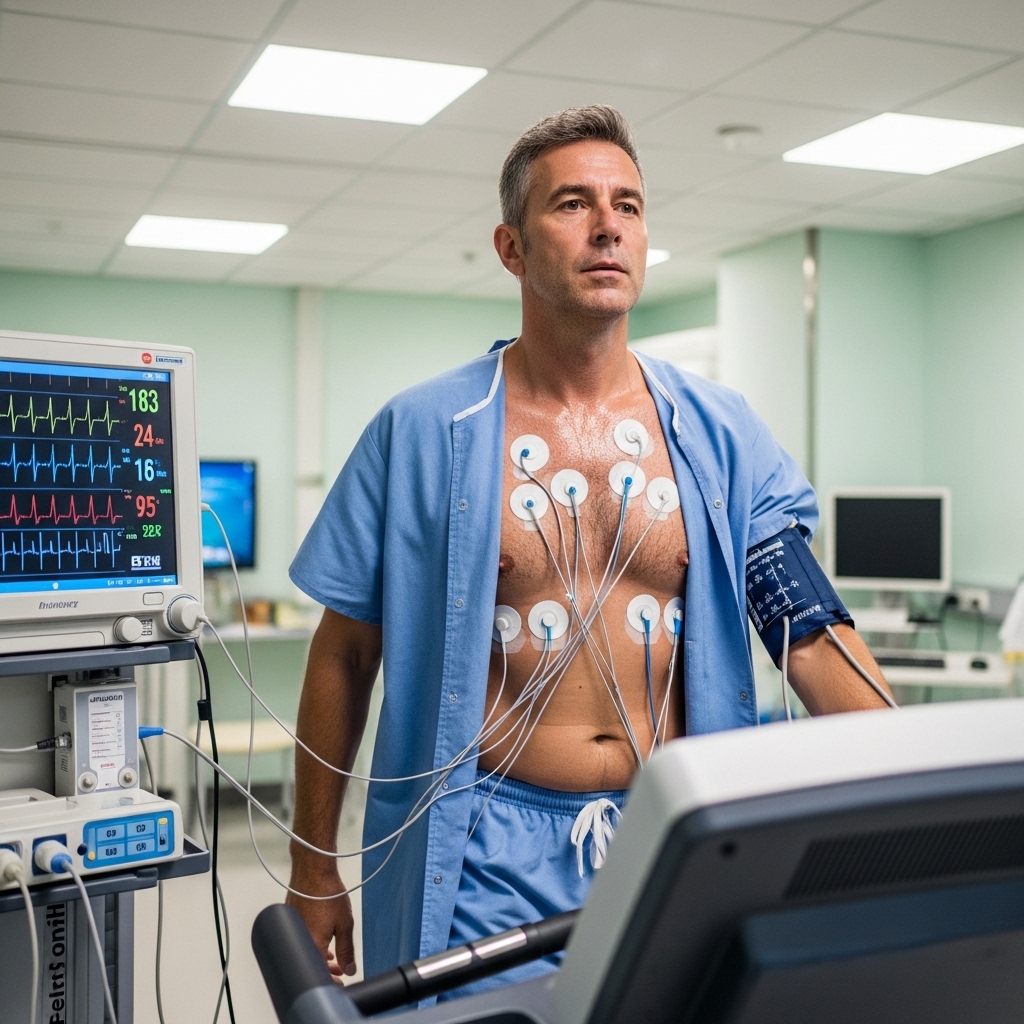
Blunt cardiac injury — the direct mechanical disruption of myocardial tissue — represents a more acute risk in severe chest trauma. However, the subtler cardiovascular consequences of sustained post-trauma physiology receive less clinical attention despite accumulating over a longer timeframe. The Framingham Heart Study's longitudinal data consistently links chronic sympathetic dominance and elevated inflammatory markers to increased cardiovascular event risk in midlife adults.
The implications extend to exercise capacity as well. Autonomic dysregulation following trauma impairs the cardiovascular adaptations that support VO2 max maintenance. For professionals who rely on aerobic fitness as a cognitive and metabolic performance foundation, unresolved trauma physiology represents a direct threat to that capacity.
The Role of Nervous System Rehabilitation in Physical Recovery

Physical rehabilitation following blunt trauma traditionally focuses on tissue repair — restoring range of motion, rebuilding muscle function, and managing pain. These are necessary goals. However, they address only one layer of the recovery requirement.
Nervous system rehabilitation addresses the autonomic dysregulation that persists beyond tissue healing. Approaches including breathwork protocols, vagal nerve stimulation techniques, and structured somatic therapies work directly on the physiological mechanisms that maintain the body in sympathetic dominance. These interventions reduce HPA axis reactivity, restore heart rate variability, and support the parasympathetic environment necessary for genuine recovery.
The distinction matters because physical rehabilitation without autonomic recovery leaves the professional functioning in a physiologically destabilized state. Tissues may heal while the nervous system continues generating inflammatory signals, disrupting sleep, and degrading cognitive performance. Comprehensive recovery requires addressing both dimensions.
Translating Evidence Into Practice

The research supports several structured approaches for professionals managing recovery from blunt force trauma. Prioritizing sleep quality through cortisol management — including limiting high-intensity stimulation in the two hours before sleep — directly supports the restoration processes that trauma disrupts. Engaging evidence-based somatic or autonomic rehabilitation alongside standard physical therapy addresses the nervous system layer of recovery that physical treatment alone does not resolve. Monitoring inflammatory biomarkers and heart rate variability during recovery provides objective data on physiological stabilization that symptom reporting alone cannot supply. For professionals in the 35 to 60 age range, treating trauma recovery as a biological age variable — not merely a physical inconvenience — aligns the recovery process with the longitudinal evidence on what the event actually costs.
UP NEXT: The Role of Emotion Regulation in Reducing Cortisol Levels and Enhancing Cognitive Performance
Unresolved blunt force trauma triggers a compounding physiological cascade — sustained HPA axis activation, systemic neuroinflammation, and disrupted sleep architecture — that measurably accelerates biological aging by elevating allostatic load, shortening telomere length, and degrading the cellular repair mechanisms that longitudinal research consistently links to earlier onset of cardiovascular disease and cognitive decline. WholeLiving's Biological Age Estimation Model incorporates this factor directly — your assessment takes under five minutes.
Ready to understand how these factors are influencing your biological age right now? [Take the Biological Age Assessment →]






