Chronic sebum overproduction is not a cosmetic inconvenience. For executives and founders operating under sustained high-stress conditions, dysregulated skin barrier function correlates directly with elevated cortisol, disrupted androgen signalling, and measurable acceleration of skin biological aging — outcomes that reflect systemic physiological dysfunction rather than surface-level aesthetics. The research is clear: sebaceous gland activity is a direct downstream marker of hormonal and inflammatory load. Yet most high-performing professionals address oily skin with generic over-the-counter products that compromise barrier integrity, accelerate transepidermal water loss, and worsen the underlying hormonal drivers. That approach has a biological cost. This article addresses the clinical evidence behind correcting it.
The Skin Barrier as a Physical System
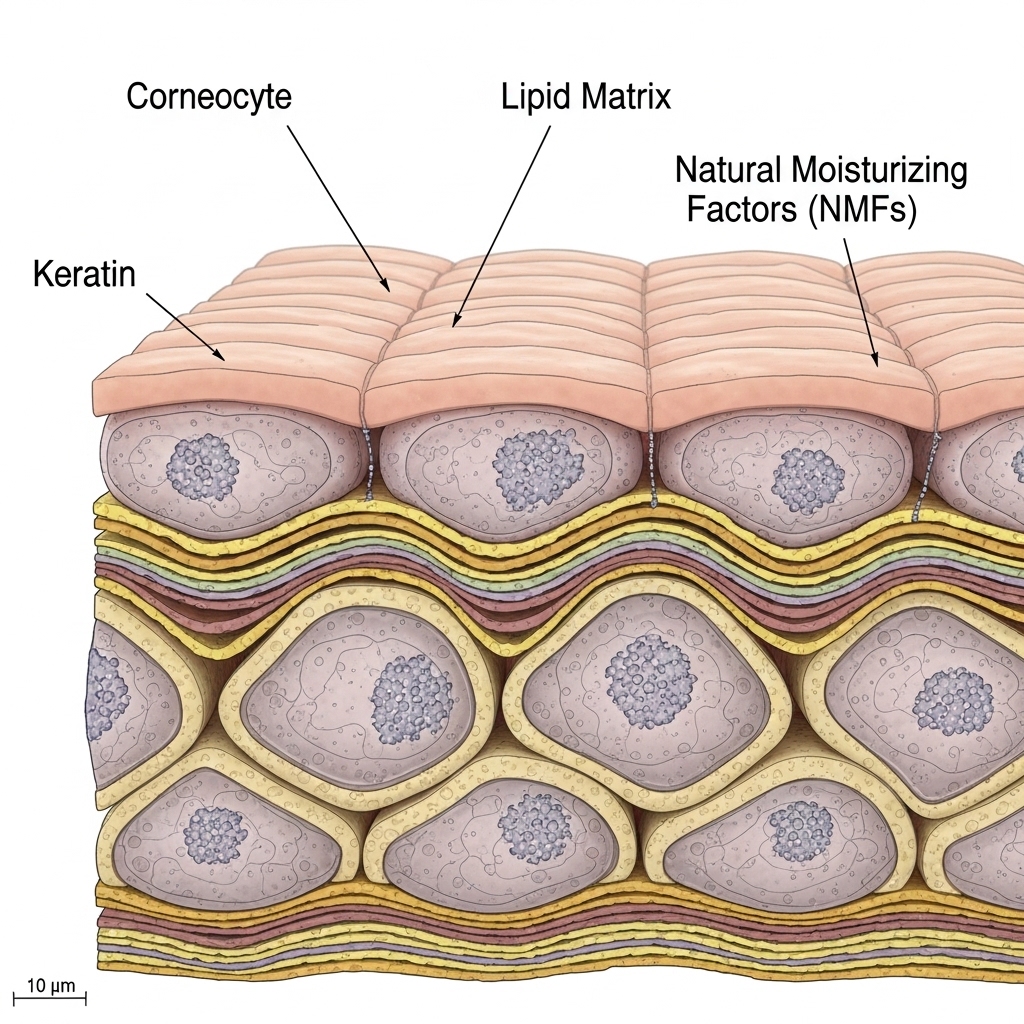
The skin is not a passive outer layer. It is an active physical system. It controls temperature, immune response, hydration, and microbial balance. The outermost layer acts as a physical and chemical barrier between the body and its environment. When intact, it blocks pathogen entry, controls water loss, and maintains the pH conditions needed for healthy microbial diversity.
When this barrier breaks down, however, the effects move inward. Barrier breakdown triggers local and body-wide inflammatory responses. It also raises inflammatory markers in the blood. Furthermore, it switches on the body's stress hormone system — the same system that drives cortisol elevation in high-performing professionals already operating under sustained cognitive load.
READ ALSO: Salicylic Acid and Skin Barrier Integrity: What High-Stress Professionals Need to Understand
What Causes Oily Skin in High Performers

Sebum — the oily substance produced by skin glands — serves a protective function. It lubricates the skin, supports barrier integrity, and carries antioxidants to the surface. The problem is not sebum itself. Rather, the problem is disrupted sebum production, driven by a specific set of triggers that affect high-performing professionals more than most.
Chronic cortisol elevation stimulates androgen production. Androgens, in turn, directly increase oil gland activity. Disrupted sleep reduces the overnight skin repair cycle. As a result, daytime oil production rises as a balancing response. Chronic inflammation — a key feature of the professional stress profile — further makes oil glands more reactive to hormonal signals.
The result is a feedback loop. The physical consequences of high performance directly worsen sebum disruption. Therefore, addressing oily skin without addressing its upstream drivers produces only partial and short-lived results. This is why cortisol management sits at the center of any complete skin health protocol for this population.
Why Generic Cleansers Make the Problem Worse

Most facial cleansers marketed for oily skin rely on high-concentration surfactants. These are detergent-like compounds that strip sebum from the skin surface. In the short term, this produces the feeling of cleanliness. In the medium term, however, it damages the skin barrier by removing not just excess sebum but the lipids essential to barrier function.
Research published in the British Journal of Dermatology shows that aggressive cleansing with high-pH surfactants disrupts the acid mantle. The acid mantle is the slightly acidic surface environment that supports barrier integrity and microbial balance. When it is repeatedly disrupted, the skin responds by producing more sebum in response.
This means harsh cleansers targeting oily skin frequently worsen the very condition they aim to address. For high performers already managing elevated inflammatory load, this cycle adds to an existing physical burden.
The pH Factor in Cleanser Selection
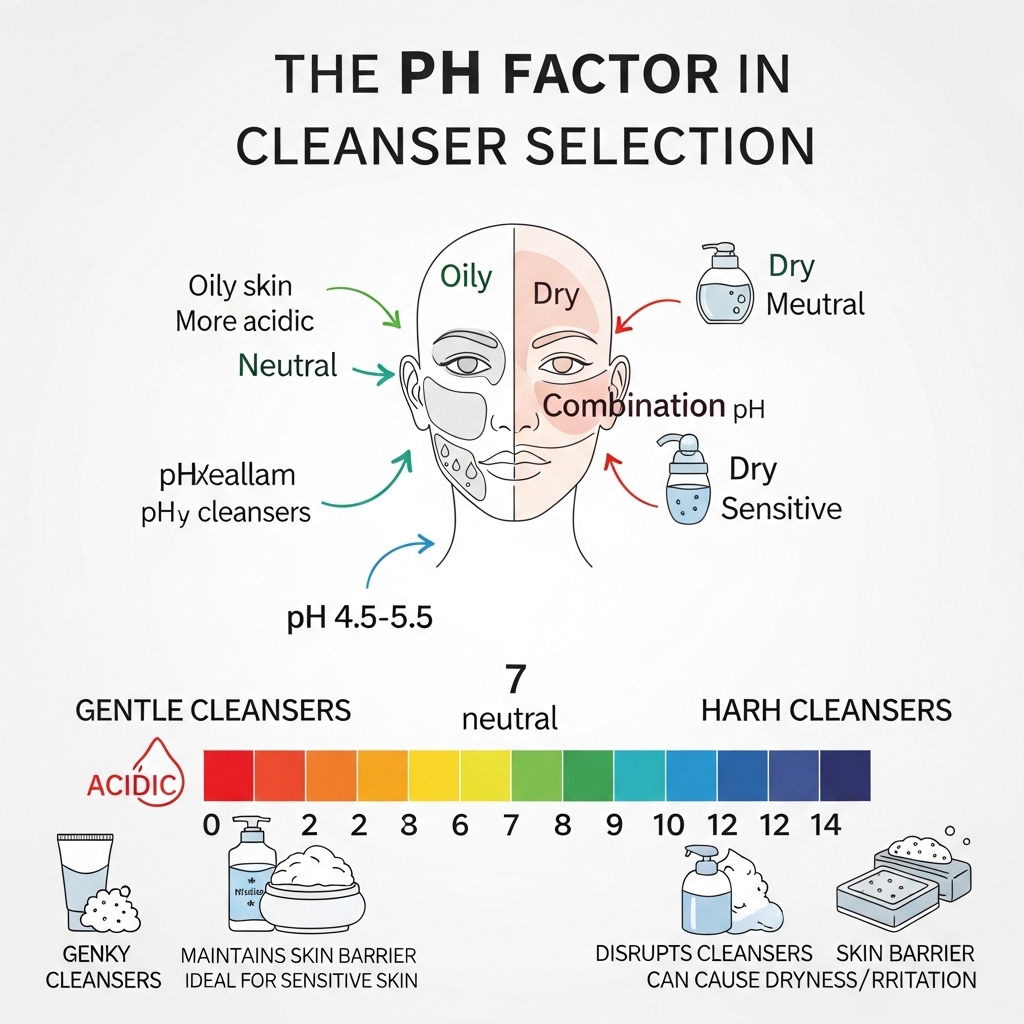
Skin surface pH in healthy adults sits between 4.5 and 5.5. This slightly acidic environment supports the processes that maintain the outer skin layer. It also blocks the growth of harmful bacteria and preserves the diversity of the skin microbiome. Most soap-based cleansers, by contrast, have a pH between 9 and 11. This range cancels out the acid mantle with each use.
Even a single application can raise skin pH measurably. Repeated daily use therefore creates a chronically disrupted barrier environment. For professionals cleansing twice daily — a common approach for oily skin — the building barrier damage from high-pH cleansers is significant and preventable.
The clinical evidence supports pH-balanced products, typically in the 4.5 to 6.5 range. These represent the right baseline for any cleansing routine targeting sebum regulation.
Surfactant Science and Barrier-Compatible Cleansing
Not all surfactants carry equal barrier disruption risk. Sodium lauryl sulphate, one of the most common surfactants in commercial cleansers, is among the most aggressive at stripping barrier lipids and raising skin pH. Milder options — including sodium laureth sulphate and glucoside-based surfactants — produce effective cleansing with substantially less barrier disruption.
A study published in Skin Pharmacology and Physiology shows that cleansers with mild surfactants maintained significantly better skin barrier function over a four-week daily use period. Researchers measured this using water loss through the skin — a standard clinical marker of barrier integrity. Cleansers containing sodium lauryl sulphate produced measurably worse outcomes by comparison.
For professionals selecting a facial cleanser, surfactant type is therefore a more clinically relevant selection point than marketing claims about oil control. Notably, the label rarely highlights this distinction, making ingredient-level reading a necessary step.
READ ALSO: Daily Facial Toner Application Restores Skin pH Balance and Supports Barrier Integrity Under Chronic Stress
The Microbiome Dimension
The skin microbiome is the community of bacteria, fungi, and other microorganisms living on the skin surface. It plays a direct role in regulating sebum metabolism, inflammatory response, and barrier function. Cutibacterium acnes — the bacterium most associated with acne and excess sebum — exists in two distinct forms. One supports healthy skin function. The other drives inflammation when the skin environment becomes disrupted.
Aggressive cleansing shifts the skin environment in favor of the inflammatory form. Research from the National Institutes of Health's Human Microbiome Project shows that skin microbiome diversity is a marker of skin health. It also shows that diversity drops significantly with repeated use of antibacterial and high-surfactant cleansers.
A cleansing routine that preserves microbiome diversity is therefore not a luxury consideration. It is, in fact, a clinical baseline for managing sebum disruption without worsening its underlying drivers.
READ ALSO: Daily Gentle Cleansing Reduces Cortisol-Linked Skin Barrier Degradation in High-Stress Professionals
Cortisol, Androgens, and the Hormonal Root of Oily Skin
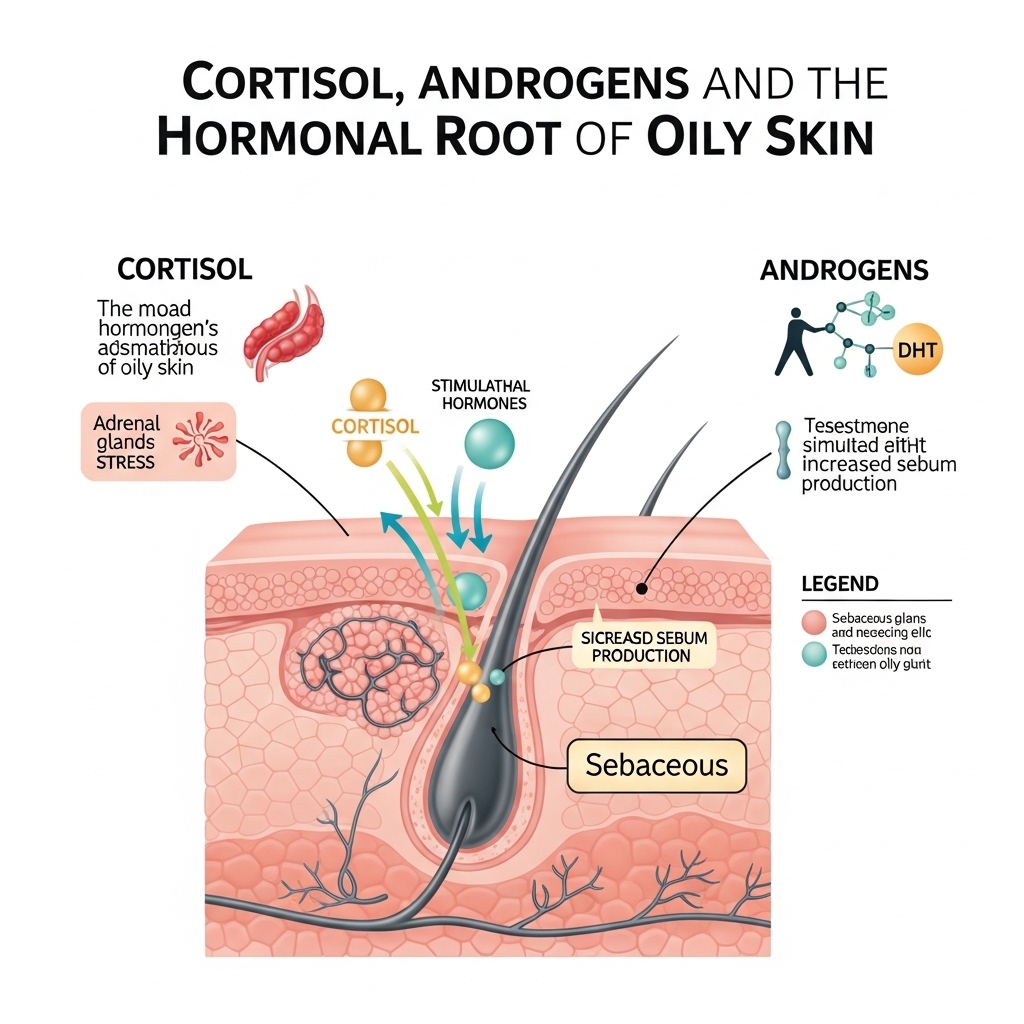
For high-performing professionals, the most significant driver of sebum disruption is not skincare routine. It is the hormonal environment created by chronic stress. Cortisol elevation stimulates adrenal androgen production. These androgens then bind to receptors in oil glands and directly increase sebum output.
This mechanism explains why oily skin frequently worsens during periods of intense professional pressure. It worsens regardless of what cleansing products someone uses. A facial cleanser cannot reverse this hormonal driver. What it can do, however, is manage surface sebum without adding to the barrier and microbiome disruption that makes oil glands more reactive to hormonal signals.
Addressing oily skin without acknowledging its hormonal root is therefore an incomplete clinical approach. Furthermore, it often leads to product escalation — using increasingly harsher cleansers — that deepens the underlying problem.
Inflammatory Markers and Skin Biological Aging
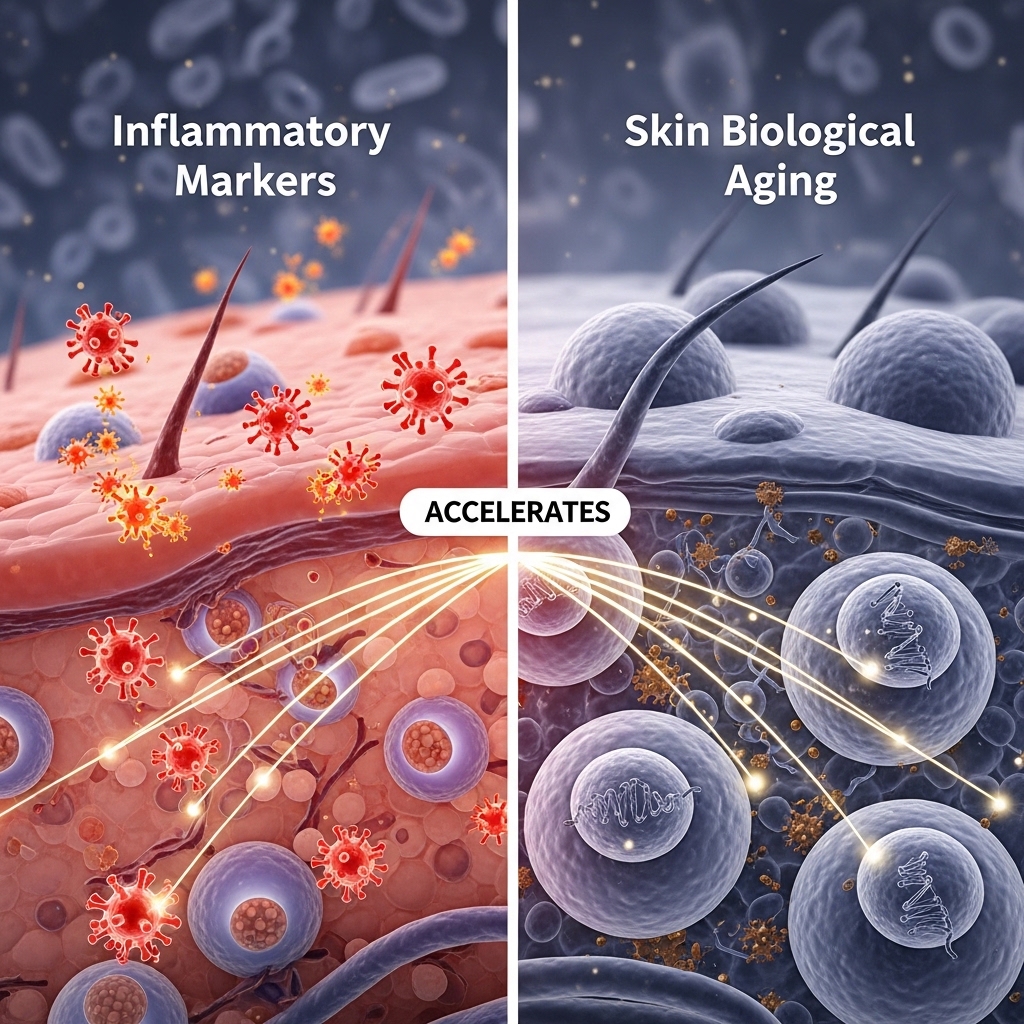
Chronic low-grade inflammation speeds up skin biological aging through a distinct but related mechanism. Inflammatory signals — including interleukin-1 and tumour necrosis factor-alpha — break down collagen and elastin. They also impair barrier repair and make oil glands more reactive to inflammatory signals.
Skin biological age — measurable through biological markers and barrier function metrics — diverges from actual age in direct relation to inflammatory load. For professionals whose internal inflammatory environment is already elevated through stress, disrupted sleep, and metabolic strain, the skin reflects this burden visibly and measurably. WholeLiving's guidance on inflammatory markers and longevity covers the broader systemic picture in detail.
Managing skin barrier integrity through appropriate cleansing is therefore not cosmetic maintenance. It is, instead, part of a broader anti-inflammatory approach with measurable biological age consequences.
The Role of Water Temperature and Cleansing Frequency

Two cleansing variables that rarely receive clinical attention — water temperature and frequency — carry measurable effects on barrier function and sebum regulation. Hot water speeds up lipid removal from the outer skin layer. It also increases water loss through the skin and triggers a balancing sebum production response. Lukewarm water, by contrast, produces effective cleansing without these barrier effects.
Cleansing frequency is equally relevant. Twice-daily cleansing is standard guidance for oily skin. However, a third or fourth cleanse — common among professionals who exercise during the day or travel across time zones — adds to barrier disruption without proportional benefit.
The clinical evidence therefore supports twice-daily cleansing as the appropriate frequency ceiling for most sebum regulation routines. Water temperature should be kept at or below body temperature to avoid unnecessary barrier stress.
Ingredients That Support Sebum Regulation Without Barrier Compromise
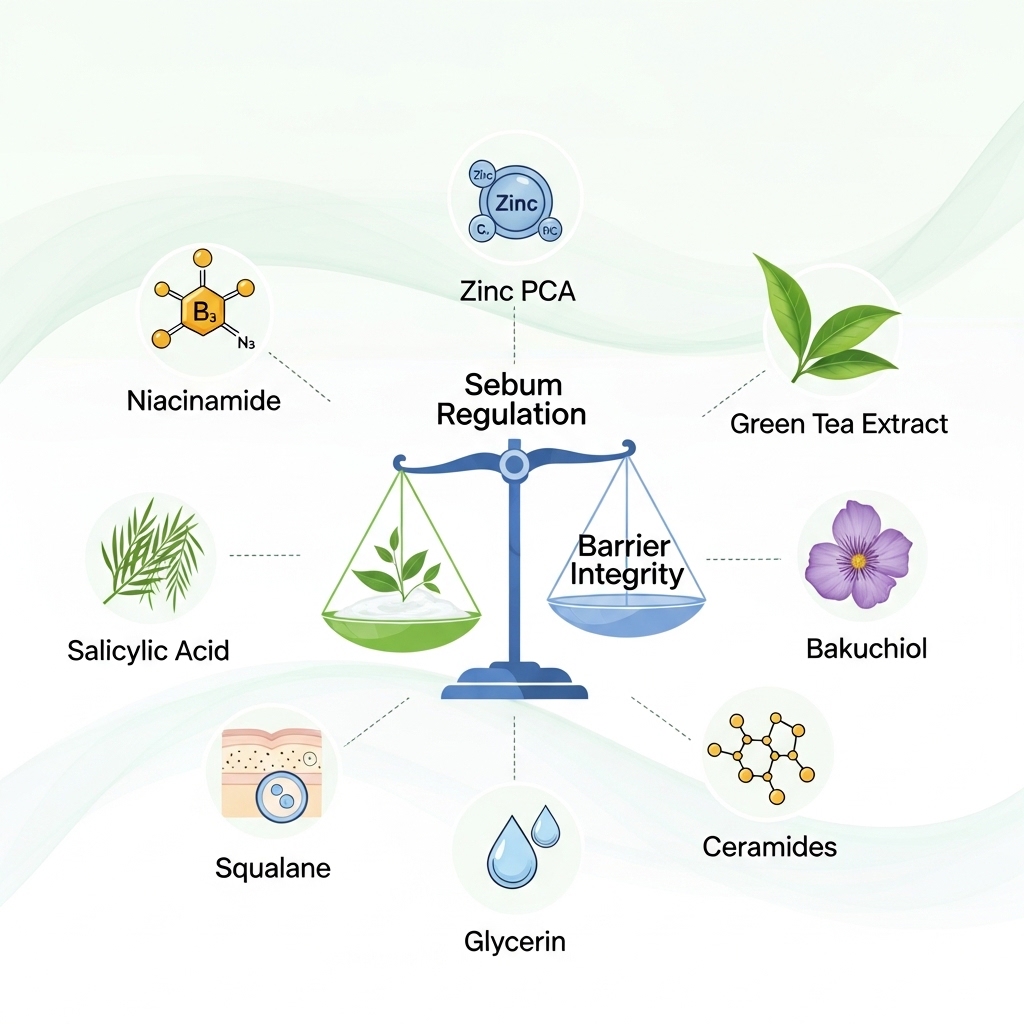
Several ingredients carry clinical evidence for sebum regulation that does not depend on barrier disruption. Niacinamide — a form of vitamin B3 — reduces sebum production by blocking the transfer of lipids to the skin surface. It at the same time supports barrier function and reduces inflammatory activity.
Salicylic acid penetrates the pore lining to dissolve excess sebum and reduce blocked pore formation. It does this without the aggressive barrier disruption linked to physical scrubbing. Zinc compounds, particularly zinc gluconate and zinc pyrithione, reduce oil gland activity through androgen receptor control. They also carry recorded anti-inflammatory effects.
Selection should be based on skin barrier status rather than sebum volume alone. Furthermore, combining multiple actives without assessing barrier tolerance is a common source of unintended barrier damage in self-managed skincare routines.
Sleep, Body Clock, and Overnight Skin Repair

The skin's repair cycle follows the body's natural daily rhythm. Between approximately 11pm and 4am, cellular repair processes peak. Collagen production accelerates, barrier lipids replenish, and oil gland activity decreases. Disrupted sleep compresses this repair window. As a result, the barrier stays under-replenished and oil glands become more reactive during waking hours.
For high-performing professionals with irregular sleep schedules, this mechanism contributes directly to daytime oiliness and barrier vulnerability. It is therefore a physical variable that no topical product can fully compensate for. Consequently, sleep quality functions as an upstream skin health variable in the same way it functions as an upstream cortisol variable.
A cleansing routine that accounts for the skin's natural daily repair process aligns with how the skin actually works. Gentle evening cleansing to remove daytime sebum, followed by barrier-supportive ingredients overnight, works with this cycle rather than against it.
Evidence-Based Options for the High-Performing Professional

The evidence reviewed here supports several cleansing and skin management approaches that align well with demanding schedules. Selecting a pH-balanced facial cleanser — formulated between 4.5 and 6.5 with mild, non-sulphate surfactants — addresses barrier integrity without sacrificing cleansing effectiveness. This is the most core change available, with immediate measurable impact on water loss through the skin.
Adding niacinamide or salicylic acid as post-cleansing actives targets sebum regulation through mechanisms that do not compromise barrier function. Limiting cleansing frequency to twice daily and using lukewarm water removes two common sources of building barrier damage that most standard routines overlook.
For professionals whose oily skin worsens under sustained professional pressure, addressing upstream cortisol and sleep quality through the broader WholeLiving framework targets the hormonal drivers that no topical routine can fully correct in isolation. Each of these approaches targets a documented physical variable and can be tracked against measurable skin outcomes over time — including barrier function, inflammatory marker trends, and biological age assessments.
UP NEXT: Best Vitamin C Serum for Gentle Radiance
Consistent use of a facial wash for oily skin helps reduce chronic skin inflammation and sebum-related irritation, factors that have been linked to accelerated cellular aging and higher biological age in dermatological studies. WholeLiving's Biological Age Estimation Model incorporates this factor directly — your assessment takes under five minutes.
Ready to understand how these factors are influencing your biological age right now? [Take the Biological Age Assessment →]






