Sustained visual sensory overload is a clinically underrecognized driver of executive dysfunction in high-performing professionals. When the occipital lobe receives more visual input than it can efficiently process, activation cascades across the frontal, parietal, and temporal lobes, elevating cognitive load and degrading working memory capacity. This neurological chain reaction measurably impairs decision-making speed, sustained attention, and mental clarity — the precise cognitive variables that determine performance at the highest levels. Left unaddressed, chronic visual overstimulation accelerates cortisol dysregulation and contributes to cumulative cognitive fatigue with compounding consequences for long-term brain health.
The Occipital Lobe's Role in Cognitive Load
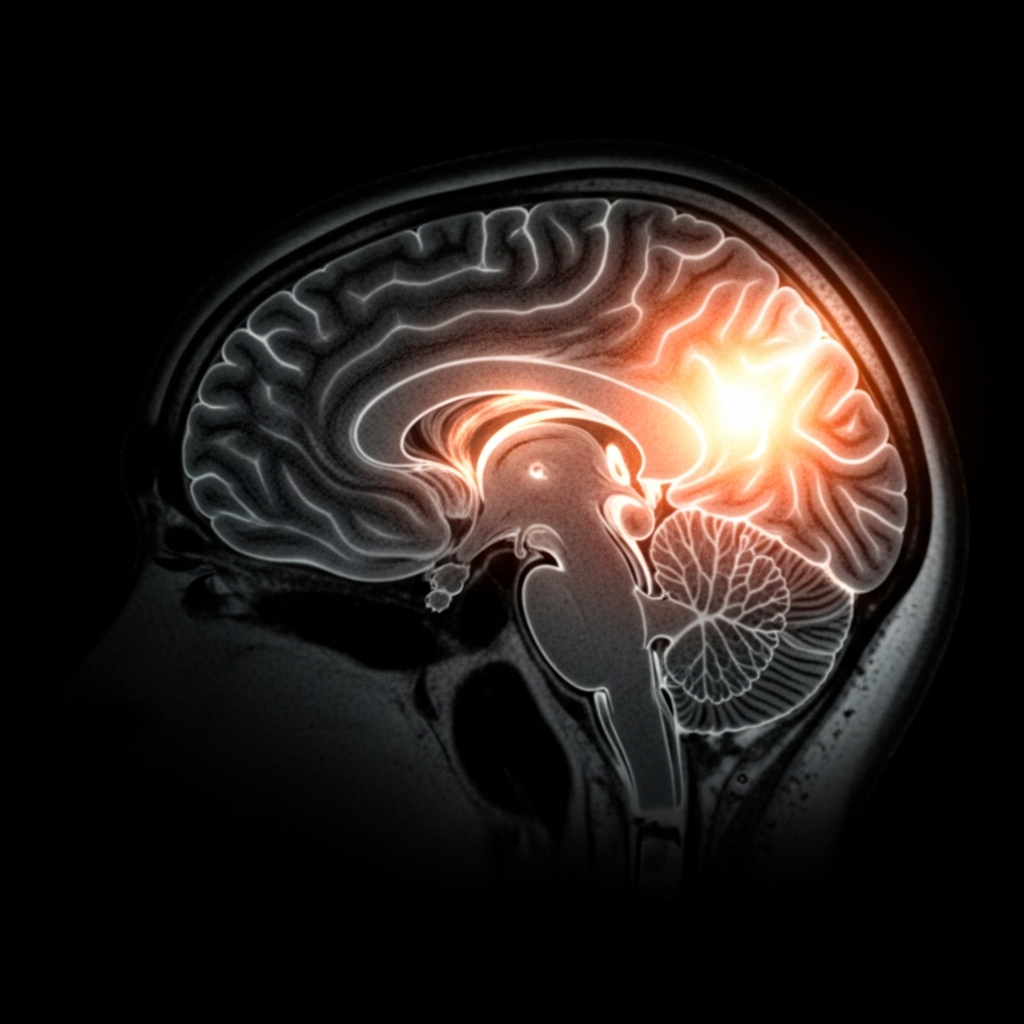
The occipital lobe sits at the posterior base of the brain and serves as the primary processing center for all visual information. It receives input directly from the retina via the optic nerve and begins decoding color, shape, contrast, and movement within milliseconds. This processing happens continuously and automatically. As a result, the brain allocates significant metabolic resources to this region, making it one of the most energy-intensive cortical areas during waking hours.
What distinguishes the occipital lobe from other sensory regions, moreover, is its direct upstream influence on higher-order cognition. Visual data does not remain contained within the occipital cortex. Instead, it travels outward along two primary pathways — the dorsal stream toward the parietal lobe and the ventral stream toward the temporal lobe. Both pathways feed directly into the networks that govern executive function, attention regulation, and working memory.
For high-performing professionals, this architecture carries a specific implication. The quality of visual input shapes the quality of cognitive output. When the occipital lobe operates under excessive load, it does not process information in isolation. Rather, it taxes the entire cortical network. That tax registers as reduced mental clarity, slower decision latency, and degraded capacity for sustained analytical thought.
How Sensory Overload Cascades Across the Brain
Visual sensory overload occurs when the volume, complexity, or rate of incoming visual stimuli exceeds the brain's current processing capacity. Modern professional environments generate this condition routinely. Open-plan offices, multi-monitor workstations, dense digital dashboards, and continuous notification streams all contribute to sustained high-volume visual input. Critically, the brain does not filter this input efficiently under prolonged exposure.
When the occipital lobe becomes overactivated, it subsequently sends amplified signals along both the dorsal and ventral streams. The parietal lobe, which manages spatial attention and visuospatial reasoning, begins competing for the same cortical resources it normally allocates to planning and analytical processing. Simultaneously, the temporal lobe increases its processing activity to interpret the meaning and emotional context of incoming visual data. The result is a system-wide escalation of cortical demand.
This cascade then reaches the prefrontal cortex — the seat of executive function. Research from the National Institutes of Health has consistently linked elevated cognitive load to measurable degradation in prefrontal cortical activity. Specifically, sustained demand reduces the prefrontal cortex's capacity for inhibitory control. This means the professional under chronic visual overload becomes less capable of filtering irrelevant information, suppressing impulsive responses, and maintaining focused attention on high-priority tasks.
The downstream consequence, therefore, is not subjective. It is functional. Decision quality declines. Error rates increase. The ability to hold multiple cognitive variables in working memory simultaneously — a core requirement of executive-level performance — diminishes in direct proportion to the duration and intensity of visual overload.
The Metabolic Cost of Visual Processing

Visual processing is metabolically expensive. The brain consumes approximately 20 percent of the body's total energy output despite representing only two percent of body weight. The visual cortex, in particular, accounts for a disproportionately large share of that consumption during periods of high visual activity. When processing demand increases, glucose consumption in the occipital region rises correspondingly.
This metabolic reality intersects directly with cognitive performance. The brain's capacity for high-quality executive function depends on stable glucose availability and efficient oxygen delivery. When visual processing draws heavily on these resources, it competes with the prefrontal cortex for the same metabolic substrate. That competition, in turn, degrades prefrontal function in real time.
Beyond glucose, sustained visual overload also activates the body's stress-response systems. The hypothalamic-pituitary-adrenal axis responds to cognitive overload by elevating cortisol output. Chronically elevated cortisol, as a consequence, suppresses hippocampal function, impairs memory consolidation, and reduces synaptic plasticity. These effects compound over time, contributing to measurable long-term cognitive decline rather than simply acute fatigue.
READ ALSO: Signs of a Brain Tumor: What to Notice Early
Cortisol Dysregulation and the Cognitive Performance Link

Cortisol elevation in response to cognitive overload follows a well-documented physiological pathway. The brain interprets sustained high-demand processing as a threat state. This interpretation triggers HPA axis activation regardless of whether the stressor is physical or cognitive. Consequently, visual overstimulation qualifies as a sufficient trigger for this response in susceptible individuals.
The relationship between cortisol dysregulation and cognitive performance decline is, furthermore, well established in the clinical literature. Chronically elevated cortisol reduces dendritic branching in the hippocampus, shrinks prefrontal gray matter volume, and impairs the neurochemical environment necessary for sustained attention. These are structural changes. They do not resolve immediately when the stressor is removed.
For professionals in the 35-to-60 age range, this dynamic carries additional significance. Cortisol regulation becomes less efficient with age. The HPA axis loses sensitivity to negative feedback, meaning cortisol levels remain elevated longer after exposure to a stressor. As a result, this reduced regulatory efficiency amplifies the cognitive cost of visual overload in older high-performing adults relative to younger populations.
Sustained cortisol elevation, beyond its direct cognitive effects, also impairs sleep architecture. It delays sleep onset, reduces slow-wave sleep duration, and fragments REM cycles. Since sleep is the brain's primary mechanism for cognitive restoration and memory consolidation, the cortisol-sleep relationship creates a compounding loop. Visual overload drives cortisol up. Elevated cortisol then degrades sleep. Degraded sleep, in turn, reduces the brain's capacity to manage the next day's visual and cognitive demands.
Working Memory, Attention Capacity, and Visual Noise

Working memory functions as the brain's active processing workspace. It holds, manipulates, and integrates information in real time. Executive function depends on working memory capacity directly. When working memory becomes saturated, cognitive performance degrades across all domains — analytical reasoning, verbal articulation, strategic planning, and interpersonal judgment.
Visual noise is, accordingly, one of the most potent reducers of working memory capacity identified in cognitive neuroscience research. A cluttered visual field occupies working memory resources that would otherwise support higher-order processing. The brain cannot fully distinguish between visual information it has chosen to attend to and visual information it is passively absorbing. Both, therefore, consume working memory bandwidth.
Research published in the journal Psychological Science has documented that environmental visual complexity independently predicts working memory performance. Participants in visually complex environments demonstrated measurably lower scores on working memory tasks compared to those in clean, visually simplified environments. The effect was consistent across age groups and cognitive profiles.
The implication for professional performance is, consequently, concrete. A cluttered screen, a visually dense office, or a meeting environment saturated with competing visual stimuli does not merely create aesthetic discomfort. It actively reduces the cognitive resources available for the work that matters most.
READ ALSO: Parietal Brain: How It Shapes Focus and Awareness
The Dorsal and Ventral Streams Under Sustained Load
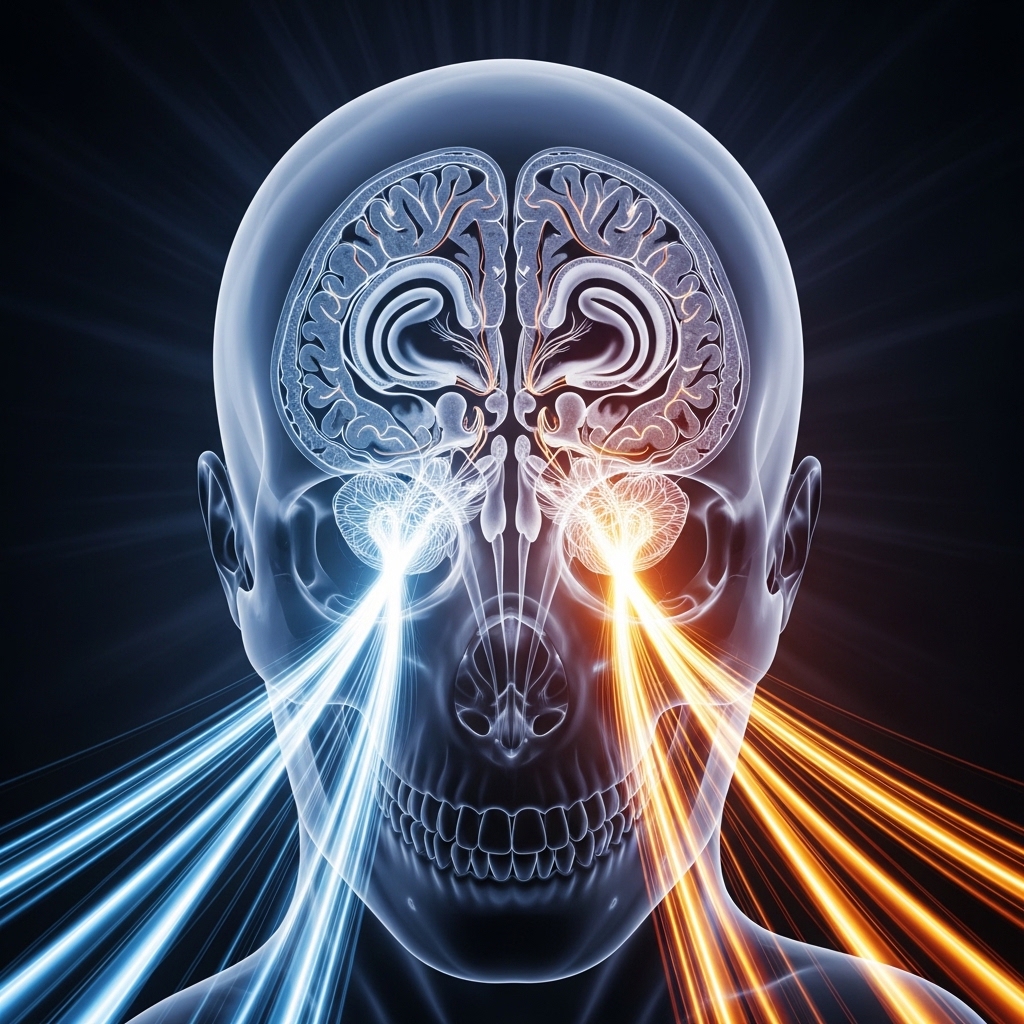
The dorsal stream connects the occipital lobe to the parietal lobe and governs spatial awareness, motion detection, and visuospatial reasoning. Under normal conditions, it operates efficiently and supports real-time environmental navigation. Under sustained visual overload, however, the dorsal stream becomes chronically active and draws processing resources away from the parietal lobe's executive support functions.
The ventral stream, by contrast, connects the occipital lobe to the temporal lobe and supports object recognition, face identification, and semantic interpretation of visual input. In high-stimulation environments, the ventral stream processes not just intended visual targets but also ambient visual information — signage, movement, screen content, and shifting light conditions. This ambient processing load is largely invisible to conscious awareness but, nonetheless, measurable in its cortical impact.
Together, the dorsal and ventral streams create a processing bottleneck when environmental visual demand exceeds the brain's current capacity. Both streams compete for shared cortical resources. The result, therefore, is reduced efficiency in both pathways. Spatial reasoning and object recognition both degrade simultaneously. This dual-stream degradation contributes directly to the experience of mental fog, slowed thinking, and difficulty maintaining focused attention that professionals identify as cognitive fatigue.
Inflammatory Markers and Chronic Cognitive Overload
Chronic cognitive overload, including that driven by persistent visual overstimulation, produces measurable changes in systemic inflammatory markers. The relationship between psychological stress and inflammation is bidirectional. Sustained cognitive demand elevates pro-inflammatory cytokines, including interleukin-6 and tumor necrosis factor-alpha. These cytokines, moreover, cross the blood-brain barrier and directly influence neurological function.
Elevated neuroinflammation, as a result, impairs synaptic transmission efficiency, reduces neurotransmitter availability, and degrades the speed and accuracy of cortical processing. The Harvard T.H. Chan School of Public Health has documented associations between chronic psychological stress, elevated inflammatory biomarkers, and accelerated cognitive aging in midlife adults. Visual overstimulation, as a sustained stressor, contributes directly to this inflammatory burden.
Importantly, neuroinflammation does not reset immediately when the stressor resolves. Pro-inflammatory cytokine levels can remain elevated for extended periods following chronic stress exposure. This means the cognitive cost of visual overload accumulates over time rather than dissipating between exposures. For professionals who operate in high-stimulation environments daily, therefore, the inflammatory burden compounds across weeks and months.
Sleep Architecture Disruption and Visual Overstimulation

The brain's restoration cycle depends critically on sleep architecture. Slow-wave sleep drives glymphatic clearance — the process by which the brain removes metabolic waste products accumulated during waking neural activity. REM sleep, additionally, supports memory consolidation and emotional regulation. Both stages require a cortisol environment conducive to neural downregulation.
Visual overstimulation disrupts this architecture through the cortisol pathway described earlier. Beyond that, high-intensity visual input in the hours before sleep — including screen use, bright artificial lighting, and visually dense content — delays melatonin secretion and postpones sleep onset. The brain requires a gradual reduction in visual stimulation to initiate the neurochemical transition toward sleep.
When sleep architecture is disrupted, the glymphatic system consequently clears less metabolic waste from the brain overnight. Accumulated waste products, including beta-amyloid and tau proteins associated with neurodegenerative risk, build up in cortical tissue. Sustained disruption of glymphatic clearance over time, therefore, represents a measurable risk factor for long-term cognitive decline. Visual overstimulation, by extension, connects directly to neurodegeneration risk through its downstream effects on sleep quality.
READ ALSO: Left Brain vs Right Brain: How Both Sides Work Together
Biological Age and the Compounding Cost of Cognitive Load

Biological aging in the brain is not determined solely by chronological age. It reflects the cumulative impact of lifestyle variables on cellular and neurological function. Chronic cortisol elevation, sustained neuroinflammation, degraded sleep architecture, and reduced glymphatic clearance all, collectively, accelerate brain biological aging beyond what genetics alone would predict.
Visual sensory overload contributes to each of these mechanisms. It elevates cortisol, drives neuroinflammation, disrupts sleep. and reduces the brain's overnight restoration capacity. Each of these effects independently accelerates biological brain age. Together, however, they compound into a pattern of accelerated cognitive aging that longitudinal research links to earlier onset of measurable cognitive decline.
For the professional aged 35 to 60, this compounding effect is particularly significant. This is the decade in which the gap between chronological and biological brain age is most plastic — most responsive to environmental modification. Reducing visual cognitive load during this period, therefore, represents a concrete, evidence-supported lever for preserving long-term cognitive performance and slowing neurological aging.
Structural Vulnerability of the Aging Visual Cortex

The occipital lobe, like all cortical regions, undergoes structural changes with age. Gray matter volume in the visual cortex declines gradually from midlife onward. Myelination of visual processing pathways becomes less efficient. As a consequence, processing speed slows. These changes are normal features of cortical aging, but they increase the brain's vulnerability to visual overload.
An aging visual cortex that processes the same volume of environmental visual input as a younger brain must work harder to achieve equivalent results. The metabolic cost per unit of visual processing increases. The threshold at which overload triggers cascade activation across connected cortical regions decreases. This means, in practical terms, that the cognitive cost of the same level of environmental visual complexity is higher for a 50-year-old professional than for a 30-year-old in the same environment.
This structural reality suggests, therefore, that environmental visual management becomes increasingly important — not less — as professionals advance through their careers. The professional who optimizes their visual environment at 45 is making a neurologically meaningful investment in their cognitive longevity. The evidence does not frame this as a lifestyle preference. Rather, it frames it as a direct input into the trajectory of brain aging.
Translating Evidence Into Practice

The research supports several structural approaches for professionals managing cognitive performance under high visual demand. Reducing ambient visual complexity in primary work environments — through screen organization, controlled lighting, and minimized peripheral movement — directly lowers occipital processing load. Scheduling blocks of low-visual-stimulation time during peak cognitive demand periods preserves working memory resources for high-priority tasks. Limiting high-intensity screen exposure in the 90 minutes before sleep supports melatonin onset and protects slow-wave sleep architecture. Additionally, exposure to natural visual environments — open landscapes, natural light, and low-complexity visual fields — has been documented to reduce cortisol and support prefrontal restoration. These are evidence-based environmental modifications, not behavioral prescriptions, and their neurological rationale is grounded in the mechanisms described throughout this article.
UP NEXT: Emotional Brain Training Practices to Lift Your Mood Daily
Chronic visual sensory overload — from excessive screen exposure, cluttered environments, and unrelenting digital stimulation — forces the occipital lobe into a state of sustained high-frequency activation that dysregulates cortisol rhythms, fragments restorative sleep architecture, and accelerates neuroinflammatory processes, collectively shown to add measurable years to biological age in studies tracking allostatic load and cellular aging markers. WholeLiving's Biological Age Estimation Model incorporates this factor directly — your assessment takes under five minutes.
Ready to understand how these factors are influencing your biological age right now? [Take the Biological Age Assessment →]






