Chronic cognitive overload — the sustained neurological state of executives managing high-stakes decisions across compressed timeframes — measurably elevates cortisol, degrades prefrontal cortex function, and accelerates biological aging at the cellular level. For professionals operating at this level, resilience is not a personality trait. It is a physiological capacity with quantifiable markers, including heart rate variability, inflammatory cytokine levels, and hippocampal volume. The Mind Project addresses this directly, applying structured gratitude practice not as a wellness intervention but as a clinical tool for cortisol regulation, autonomic nervous system recalibration, and the preservation of long-term cognitive performance under sustained professional pressure.
What the Mind Project Actually Is

The Mind Project is not a mindfulness trend. Nor is it a corporate wellness program. Instead, it is a structured cognitive resilience protocol. It is built on the neuroscience of gratitude practice — the deliberate, repeated activation of neural circuits tied to positive social cognition, reward processing, and emotional regulation. This distinction matters. Unstructured positive thinking produces no measurable physiological change. Structured gratitude practice, applied consistently, produces documented shifts in cortisol output, nervous system tone, and inflammatory marker levels.
The protocol draws from converging research in psychoneuroimmunology — the study of how psychological states influence immune and nervous system function. This field has moved well beyond soft science. It now produces quantifiable, reproducible findings that connect specific mental practices to specific biological outcomes. For professionals who already track HRV, sleep quality, and cognitive performance metrics, the Mind Project offers an evidence-based intervention. It operates at the same level of biological specificity as other performance protocols.
The core mechanism is neurological. Repeated gratitude practice strengthens the connection between the prefrontal cortex — which governs executive function — and the limbic system, which governs emotional and stress responses. Over time, this strengthening shifts the default balance of this circuit toward prefrontal dominance. As a result, stress reactivity decreases, baseline cortisol drops, and the capacity to sustain high-quality cognitive output under pressure improves measurably.
The Neuroscience of Gratitude as a Clinical Tool

Gratitude activates a specific and well-mapped neural network. Neuroimaging studies show consistent activation of the medial prefrontal cortex, the anterior cingulate cortex, and the nucleus accumbens during gratitude processing. These regions govern moral reasoning, conflict resolution, and reward anticipation. Moreover, their repeated activation through structured practice produces measurable changes in neural density and connectivity — a process known as neuroplasticity.
Research published by the Greater Good Science Center at the University of California, Berkeley documents that sustained gratitude practice produces lasting changes in neural activation patterns. Critically, these changes persist beyond the practice sessions themselves. As a result, the brain begins to default toward the activated circuits. This reduces the cognitive energy required to maintain emotional regulation under stress. For executives managing sustained decision fatigue, that reduction represents a direct and measurable performance gain.
The clinical significance also extends to brain chemistry. Gratitude practice links to increased release of dopamine and serotonin — both central to mood regulation, motivation, and cognitive flexibility. Dopamine plays a key role in the brain's reward and learning circuits. Its consistent activation through gratitude practice reinforces the neural pathways that support adaptive thinking. These are the same pathways that degrade rapidly under chronic stress.
Cortisol Regulation and the HPA Axis
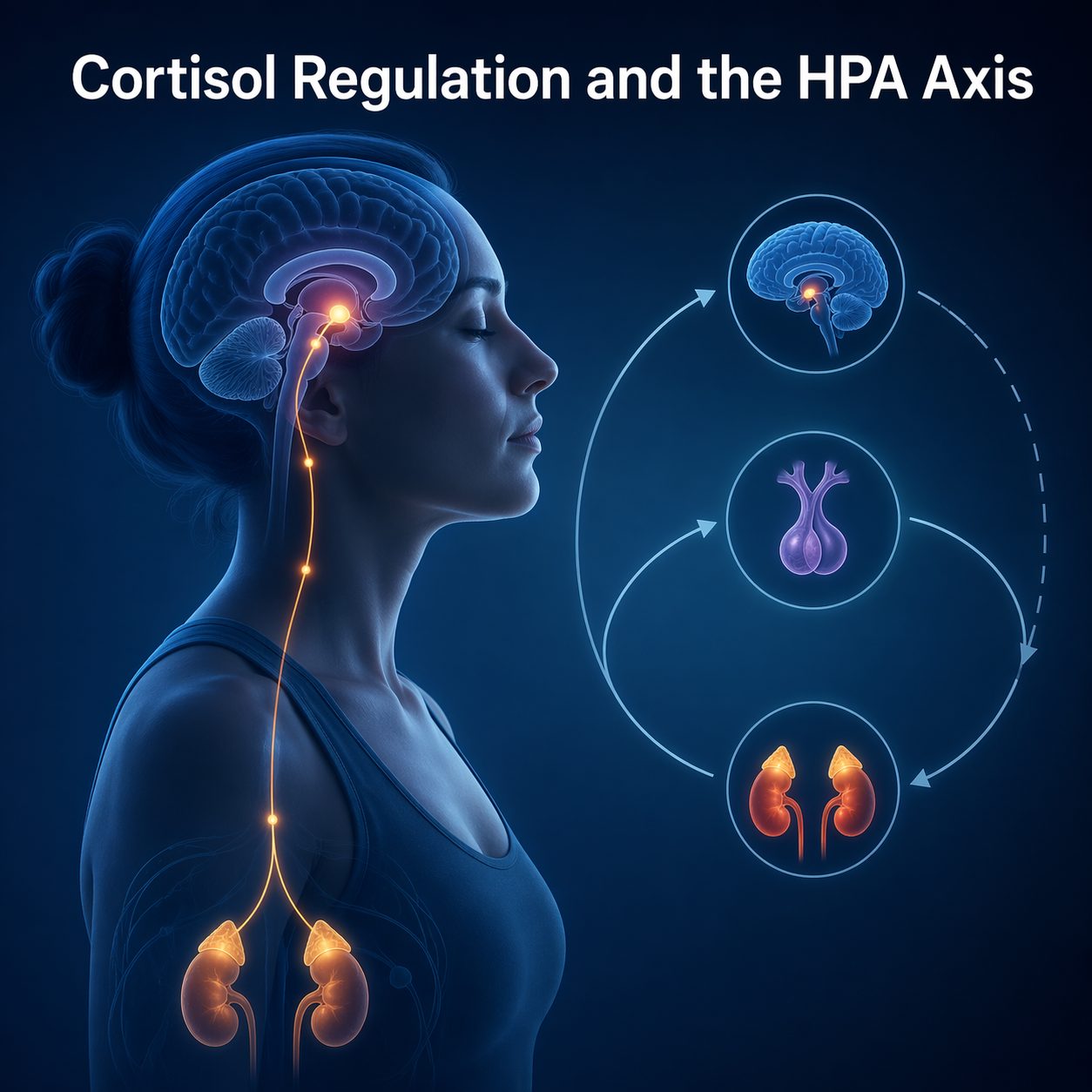
Cortisol is the primary stress hormone produced by the hypothalamic-pituitary-adrenal (HPA) axis. In short bursts, cortisol is adaptive — it sharpens alertness and mobilizes energy. In chronic elevation, however, it is destructive. Sustained high cortisol degrades memory function, impairs blood sugar regulation, and suppresses immune function. It also accelerates cellular aging through telomere shortening. These are documented biological consequences of the cortisol profiles common among high-performing professionals.
Structured gratitude practice directly modulates HPA axis activity. A study published in Psychoneuroendocrinology found that participants who engaged in regular written gratitude practice showed significantly lower cortisol levels compared to control groups. The effect size was clinically meaningful — not marginal. The mechanism involves the prefrontal cortex's inhibitory influence over the amygdala, which drives HPA activation. Strengthening this connection through repeated practice reduces both the frequency and intensity of cortisol spikes triggered by perceived threat.
For professionals operating under sustained pressure, cumulative cortisol load is one of the most significant drivers of accelerated biological aging. The Mind Project targets this load directly. By reducing baseline cortisol through structured practice, it creates conditions for biological repair — cellular maintenance, immune regulation, and tissue recovery. These are the same processes that chronic cortisol elevation actively suppresses. This is cortisol management through neurological intervention, not pharmacology.
Heart Rate Variability as a Measurable Outcome

Heart rate variability (HRV) — the variation in time between consecutive heartbeats — is one of the most sensitive available markers of autonomic nervous system health and stress resilience. High HRV reflects flexible, adaptive autonomic function. Low HRV, by contrast, reflects chronic sympathetic dominance — the sustained fight-or-flight state that marks cortisol overload. HRV is now tracked routinely by executives using wearable devices. Its correlation with cognitive performance, cardiovascular health, and biological age is well established.
Gratitude practice measurably improves HRV. Research from the HeartMath Institute documents consistent HRV improvements in participants who engage in structured positive emotion practices, including gratitude. The mechanism involves vagal tone — the activity level of the vagus nerve, which connects the brain to the heart, lungs, and digestive system. Gratitude practice activates the parasympathetic nervous system. In doing so, it directly increases vagal tone and produces the HRV improvements that reflect genuine autonomic recalibration.
For professionals who monitor HRV as a performance metric, the Mind Project provides a trackable intervention with a clear physiological pathway. HRV improvements from structured gratitude practice are not immediate — they build over weeks of consistent practice. Unlike acute relaxation techniques that produce temporary HRV shifts, however, gratitude practice produces structural changes in autonomic regulation. These changes persist across high-stress periods, making it a more reliable resilience tool for professionals who cannot control their external stress load.
Inflammatory Markers and Biological Age
Chronic low-grade inflammation — measured through markers including C-reactive protein (CRP), interleukin-6, and tumor necrosis factor-alpha — is one of the most robust predictors of accelerated biological aging and age-related disease risk. The National Institutes of Health has documented the central role of inflammatory imbalance in cardiovascular disease, metabolic dysfunction, cognitive decline, and muscle loss. Professionals with chronically elevated inflammatory markers age biologically faster than their chronological age suggests.
Psychological stress is a primary driver of this inflammatory imbalance. Both the HPA axis and the sympathetic nervous system stimulate pro-inflammatory signaling when chronically activated. Gratitude practice, by reducing HPA and sympathetic activation, creates downstream reductions in inflammatory output. Research published in Brain, Behavior, and Immunity documents inverse relationships between positive psychological states — including gratitude — and circulating inflammatory marker levels in adult populations.
The implication for biological age is direct. Reducing chronic inflammatory load is one of the most evidence-supported strategies for slowing biological aging at the cellular level. Furthermore, the Mind Project's effect on cortisol, autonomic tone, and inflammatory signaling positions it as a genuine biological age intervention — not a mood management tool. For professionals who track biological age markers, structured gratitude practice represents a low-cost, high-leverage addition to their longevity protocol.
READ ALSO: Magic Mind: Unlock Your Full Potential with Mindfulness
Sleep Quality and Cognitive Recovery

Sleep is the primary biological mechanism through which the brain clears metabolic waste, consolidates learning, and repairs cellular damage. Slow-wave sleep and REM sleep — the stages most critical to cognitive restoration — are highly sensitive to cortisol levels and autonomic state at sleep onset. Professionals with elevated evening cortisol and low HRV consistently show compressed slow-wave and REM duration, regardless of total sleep time.
Gratitude practice performed in the evening measurably improves both sleep onset and sleep quality. A study published in the Journal of Experimental Psychology found that participants who wrote about things they were grateful for before sleep fell asleep faster. They also reported better sleep quality than those who wrote about worries or neutral topics. The mechanism involves the shift from sympathetic to parasympathetic dominance that gratitude practice produces. Reduced cortisol and improved vagal tone at sleep onset then create the biological conditions that support deeper, more restorative sleep.
For executives who struggle with the transition from high-activation professional mode to restorative sleep, the Mind Project's evening gratitude practice addresses the precise physiological bottleneck at play. The intervention does not require extended time. Structured written gratitude practice of five to ten minutes, performed consistently before sleep, produces measurable changes in sleep onset and slow-wave sleep duration. These changes accumulate over weeks of regular practice.
READ ALSO: The Theory of the Mind: Unlock Your Mental Potential
Cognitive Performance Under Sustained Pressure

Executive function — the cluster of cognitive capacities that includes working memory, cognitive flexibility, inhibitory control, and planning — is the professional's primary performance asset. It is also acutely sensitive to cortisol elevation and inflammatory load. Chronic stress does not merely create subjective feelings of mental fatigue. Rather, it produces measurable declines in prefrontal cortex function. These declines reduce decision quality, slow processing speed, and increase cognitive error rates.
Gratitude practice protects executive function through multiple pathways. By reducing cortisol, it removes one of the most direct neurological suppressants of prefrontal activity. By improving sleep quality, it supports the overnight restoration of working memory and cognitive flexibility. Additionally, by increasing dopamine and serotonin activity, it enhances the motivational and attentional systems that underpin sustained cognitive effort. Together, these effects produce a measurable improvement in cognitive resilience — the ability to maintain executive function output under sustained pressure.
Research from Harvard Medical School has documented the relationship between positive psychological states and preserved cognitive function in high-stress adult populations. The consistent finding is that individuals with higher baseline positive affect show slower cognitive aging and better working memory performance. They also show lower rates of stress-induced cognitive impairment. For professionals whose decision quality directly determines financial and organizational outcomes, these findings carry direct operational relevance.
The Role of Consistency and Protocol Structure

The clinical benefits of gratitude practice are dose-dependent and protocol-sensitive. Occasional or unstructured practice produces weak and inconsistent effects. Consistent, structured practice — applied at regular intervals with specific cognitive focus — produces the neural adaptation, cortisol modulation, and autonomic recalibration that the research documents. In short, the distinction between structured and unstructured practice separates a genuine intervention from a habit with no measurable outcome.
Effective gratitude protocols share several structural features. Written expression, rather than passive reflection, engages additional neural circuits that deepen processing and strengthen memory consolidation. Directing attention toward specific, concrete experiences — rather than abstract positive sentiment — produces stronger and more durable neural activation. Furthermore, performing the practice consistently at the same time each day aligns it with the body's internal clock. This alignment reinforces the neural pathways through repetition.
The Mind Project applies these structural principles directly. The protocol is designed to be performed in under ten minutes. This makes it compatible with demanding professional schedules. Its clinical value does not come from duration. Rather, it comes from specificity, consistency, and the deliberate engagement of the neural circuits that govern cortisol regulation, autonomic tone, and cognitive resilience. Volume does not drive the outcome — precision and repetition do.
READ ALSO: Consciousness Anesthesia: Mindful Moments in Recovery
Psychological Safety and High-Performance Culture

The adoption of practices like the Mind Project within high-performance professional culture has historically faced resistance. The prevailing perception has been that emotional or psychological practices are incompatible with high-stakes, analytical work. This perception, however, is not supported by the evidence. The neurological mechanisms that gratitude practice engages — prefrontal strengthening, HPA modulation, autonomic recalibration — are the same mechanisms that underpin elite cognitive and physical performance across domains.
Research from the field of positive organizational psychology, including work published through institutions such as the Wharton School of Business at the University of Pennsylvania, documents that executives who engage in structured positive psychological practices show higher cognitive flexibility and better team decision outcomes. They also show lower rates of burnout-related performance decline. These are not soft outcomes. Rather, they are measurable performance variables with direct organizational and financial consequences.
The Mind Project reframes gratitude practice within this evidence base — not as a wellness add-on, but as a cognitive performance protocol grounded in neuroscience. For professionals who apply the same analytical rigor to their psychological health as they do to their physical performance metrics, this reframing removes the cultural barrier that has historically limited adoption. Evidence-based mental resilience tools belong in high-performance environments. The research now makes that case clearly.
Evidence-Based Application for High-Performing Professionals

The research supporting the Mind Project points toward a structured, consistent, and specific approach to gratitude practice as a genuine clinical intervention. It targets cortisol regulation, HRV improvement, inflammatory load reduction, and cognitive resilience preservation. Professionals seeking measurable outcomes benefit most from written gratitude practice performed at consistent times — particularly in the evening, where the parasympathetic shift it produces directly supports sleep architecture. Pairing the practice with HRV tracking allows professionals to monitor autonomic adaptation over weeks and validate the biological response the research predicts. For those already tracking inflammatory markers or biological age markers, incorporating the Mind Project as a longitudinal variable offers a credible, low-resource option for assessing its contribution to the broader longevity protocol.
UP NEXT: Mindfulness Practices for Burnout: Simple Ways to Recover
How This Affects Your Biological Age
Chronic psychological stress and the cortisol dysregulation it produces are among the most well-documented drivers of accelerated biological aging, with sustained HPA axis overactivation linked to telomere shortening, elevated inflammatory markers, and an estimated two to four additional years of biological age in population-level research. WholeLiving's Biological Age Estimation Model incorporates this factor directly — your assessment takes under five minutes.
Ready to understand how these factors are influencing your biological age right now? [Take the Biological Age Assessment →]






