Posterior chain weakness is not a gym problem. For executives and founders operating under sustained sedentary and high-stress conditions, the progressive loss of back muscle strength and structural integrity correlates directly with accelerated postural decline, reduced VO2 max, increased all-cause injury risk, and measurable drops in functional movement capacity — all of which compound into long-term performance deficits that no amount of cardiovascular training can offset. The research is clear: back muscle function is a primary load-bearing variable in both physical longevity and daily output. Yet most high-performing professionals ignore it entirely until pain or structural failure forces the conversation.
The Posterior Chain as a Longevity Structure
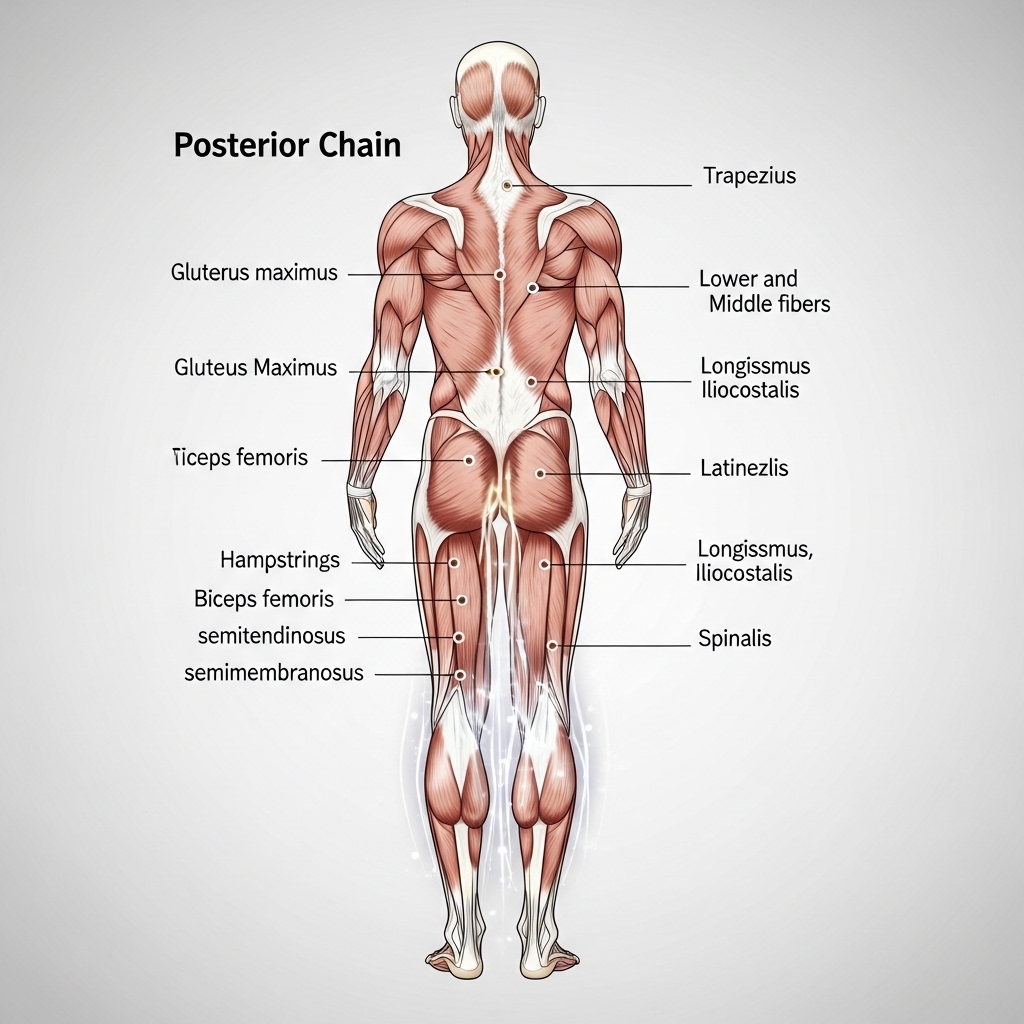
The back is not a single muscle. It is a layered system of muscles, tendons, and connective tissue. This system runs from the base of the skull to the pelvis. Doctors and researchers call it the posterior chain. It controls nearly every movement the body performs — from sitting upright at a desk to lifting, rotating, and absorbing impact.
When this system works well, it spreads load efficiently and protects the spine. It also supports the heart and the energy demands of an active life. When it begins to weaken, the effects go far beyond back pain. They influence posture, breathing, hormone balance, and long-term physical capacity.
For high-performing professionals, the posterior chain is one of the most overlooked physical factors in their overall health profile. Many executives invest heavily in heart metrics, metabolic testing, and sleep tracking. Yet the structural system most responsible for long-term physical durability often receives little attention until pain or injury forces the issue.
The Major Muscles and What They Do
The back can be divided into three functional layers. The outer layer includes the trapezius and the latissimus dorsi. These are large, visible muscles that control shoulder movement, pulling strength, and upper-body stability. They are the muscles most commonly trained in the gym. Yet they represent only one part of a much deeper system.
The middle layer includes the serratus posterior muscles. These muscles support breathing by helping the ribs lift during inhalation. This layer rarely receives attention in performance health discussions. Yet its function directly affects breathing efficiency and, in turn, heart output during both exercise and sustained mental work.
The deepest layer is the most important for long-term spinal health. It includes the erector spinae group and the multifidus. These muscles run along the spine and manage extension, rotation, and fine control between individual vertebrae. Another muscle, the quadratus lumborum, connects the lower back to the pelvis and helps stabilise the body from side to side while transferring load between the upper and lower body.
Knowing which layer is underperforming is essential when building an effective training programme. Surface-level strength training mainly targets the outer layer but often leaves the deeper stabilising muscles undertrained. As a result, a professional may appear physically strong while carrying hidden spinal weakness beneath the surface.
READ ALSO: Latissimus Muscle: The Secret to a Stronger, Leaner Back
The Multifidus: The Most Overlooked Muscle in Performance Medicine
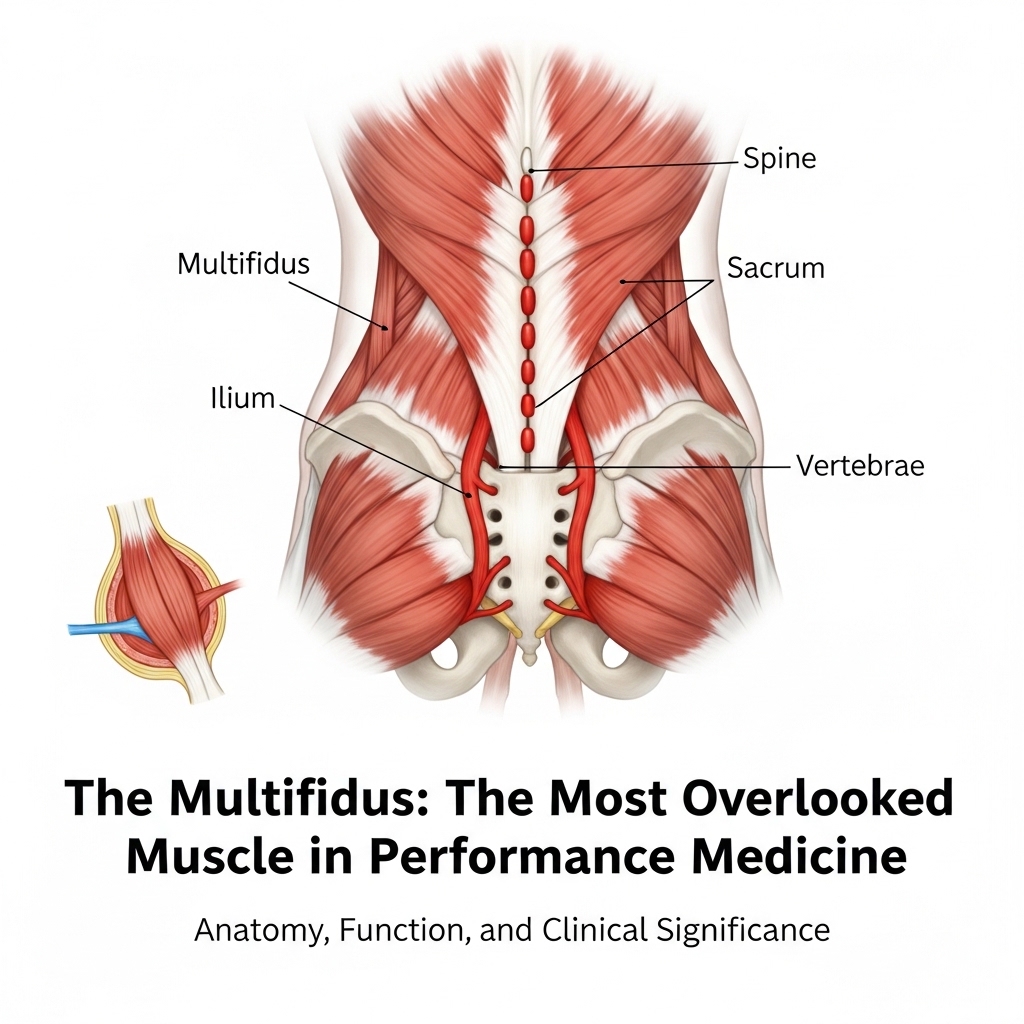
Of all the back muscles, the multifidus receives the least attention in general fitness programmes. Yet it receives the most attention in clinical research. This deep spinal muscle attaches directly to each vertebra and provides precise, segment-by-segment stability that larger muscles cannot deliver.
Research published in the journal Spine shows that the multifidus shrinks quickly after even a single episode of lower-back pain. Importantly, this shrinkage does not reverse on its own, even after the pain disappears. Professionals who return to normal activity without targeted rehabilitation may carry ongoing weakness without realizing it.
The effects of multifidus weakness extend beyond back pain. When fine spinal control decreases, movement patterns throughout the body change. Extra load shifts to the hips, knees, and shoulders. Over time, this pattern increases joint wear and raises injury risk in areas far from the lower back itself.
Identifying multifidus weakness usually requires clinical assessment rather than standard gym testing. A movement physiotherapist or sports medicine specialist can evaluate spinal control through specific movement tests. For professionals who have never had this layer assessed, doing so fills an important gap in their overall physical health profile.
Sarcopenia, Muscle Mass, and the Ageing Back
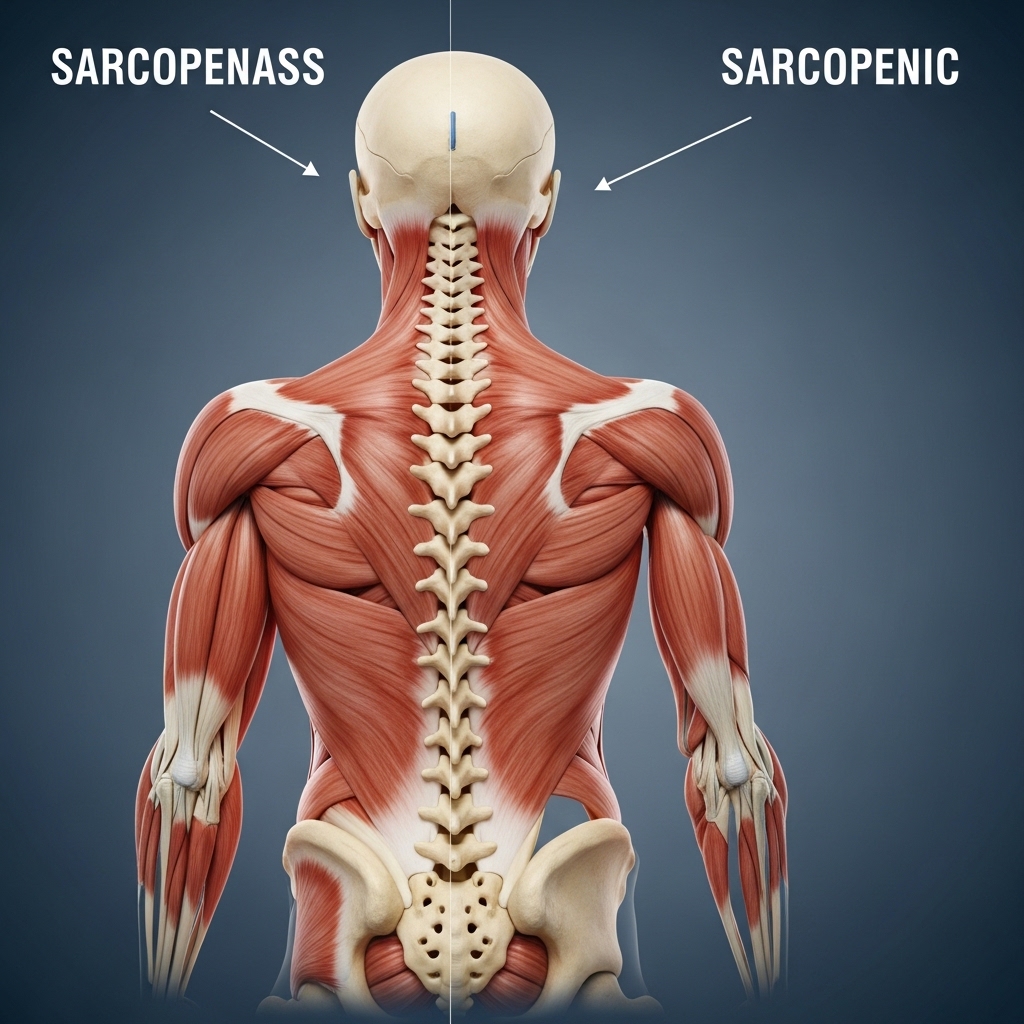
Sarcopenia refers to the age-related loss of muscle mass and strength. The posterior chain is not immune to this process. In fact, the deep spinal stabilizer are often among the first muscles to decline with age. This happens partly because standard exercise programmers rarely train them and partly because sedentary work reduces the low-level activity these muscles need to remain strong.
Research from the National Institute on Aging links spinal muscle loss with reduced functional capacity and a higher risk of falls. It also connects this decline with faster loss of physical independence in later life. These findings are not limited to older adults. The process begins in the fourth decade of life and continues steadily without deliberate action.
For professionals between 35 and 60, the window to build and preserve posterior chain muscle is both open and gradually closing. Muscle loss accelerates after age 60. This makes midlife the most important period for physical investment. Every year of inactivity during this time creates structural weakness that becomes harder to reverse later.
There is also a metabolic side to posterior chain muscle loss. Muscle tissue drives the body's resting metabolic rate. As muscle mass declines, energy output drops and insulin sensitivity decreases. Over time, this raises the risk of metabolic problems. For this reason, maintaining posterior chain strength supports both structural and metabolic health.
READ ALSO: Stretching Exercise for Lower Back Pain You Can Do in Bed
Posture, Breathing, and Cardiovascular Efficiency
The link between back muscle function and heart performance is mechanical. The mid-back region directly affects rib cage movement. The erector spinae and rhomboid muscles help control this area. When the mid-back works well, the rib cage expands fully during inhalation. This allows the lungs to take in more air with each breath.
When mid-back mobility becomes restricted — from weakness or constant forward bending — rib expansion decreases. Less air moves with each breath. The body compensates by breathing faster, which reduces efficiency and can raise resting heart rate. Over time, this pattern can limit VO2 max.
For professionals tracking heart performance through wearable devices, unexplained plateaus in VO2 max may sometimes come from mid-back dysfunction rather than the heart itself. Improving mid-back mobility and strength can occasionally raise cardiovascular metrics without increasing aerobic training volume. This is a frequently missed performance lever in an otherwise optimized health program.
The rhomboids and mid-trapezius help pull the shoulder blades back and stabilize them. These muscles maintain the posture required for full rib expansion. When they become weak, the shoulders roll forward and the chest collapses slightly, leaving less space for lung expansion. Strengthening this region therefore supports both posture and breathing efficiency.
The Cortisol Connection: Pain, Posture, and Stress Physiology

Ongoing lower-back tension and poor posture can activate the body's stress response. When the posterior chain carries constant mechanical load — from prolonged sitting or inefficient movement — low-level pain signals reach the nervous system. These signals contribute to a steady rise in baseline cortisol.
This pattern differs from the short cortisol spikes that occur during exercise or acute stress. Instead, it represents a slow and persistent increase tied to ongoing physical strain. Chronically elevated cortisol is associated with abdominal fat accumulation, weakened immunity, and disrupted sleep. For professionals already managing high cognitive stress, this physical source of cortisol adds another layer of strain that most cortisol management protocols do not address.
Improving posterior chain strength can therefore reduce more than physical discomfort. It can also help regulate stress physiology. Many professionals who improve back strength report better sleep, improved energy levels, and lower day-to-day fatigue. These are all downstream effects of reduced baseline cortisol.
The relationship also works in the opposite direction. High cortisol levels increase the nervous system's sensitivity to pain. As a result, stress can make physical discomfort feel worse. Breaking this cycle — either by reducing physical strain or lowering cortisol levels — can produce meaningful improvements in both comfort and performance.
READ ALSO: Cobra Posture: Gentle Alignment for Strength and Nourishment
Spinal Load Distribution and Injury Risk
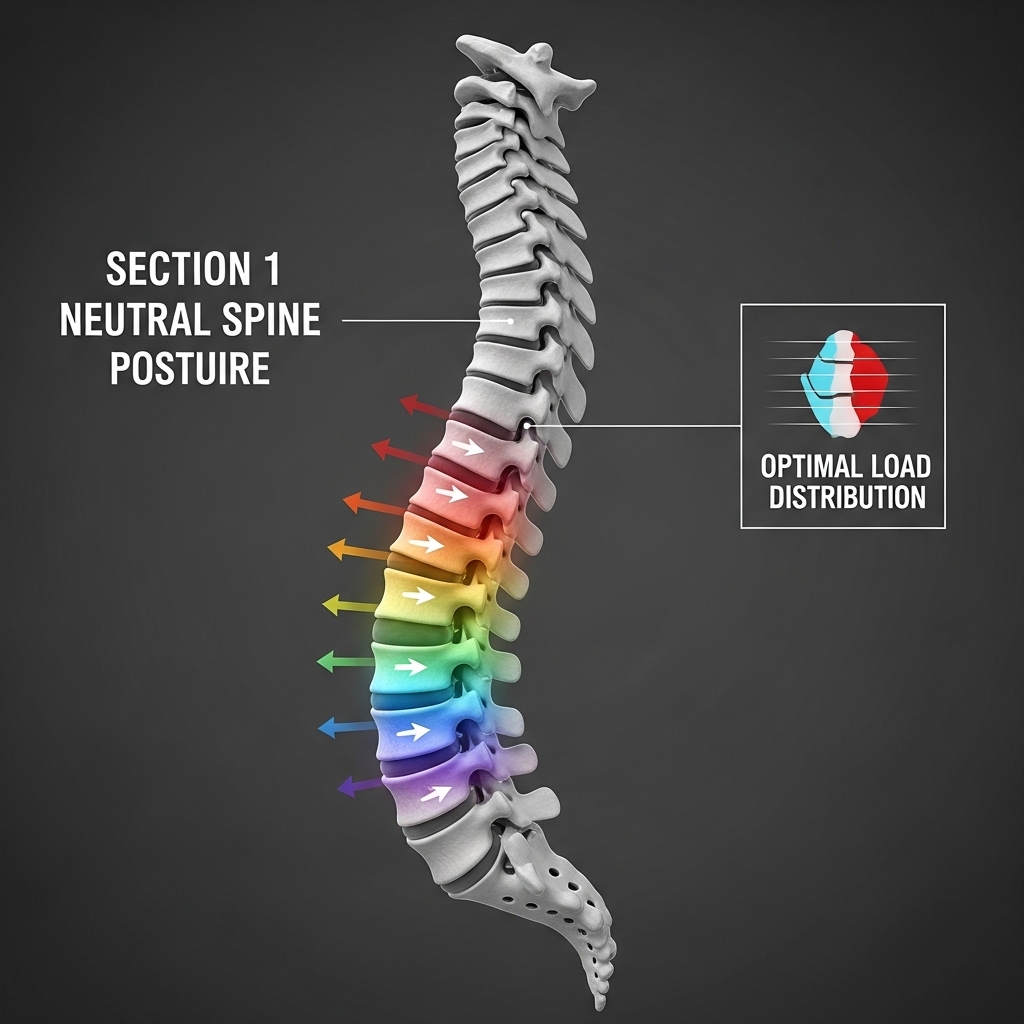
The lower back carries more pressure than any other part of the spine during both sitting and standing work. In a healthy posterior chain, this load spreads across several muscles, spinal discs, and joints. When the system functions properly, no single structure absorbs excessive stress.
When posterior chain muscles weaken, this balance changes. Passive structures such as spinal discs and ligaments begin to absorb forces they were not designed to handle over long periods. The result is faster disc degeneration, increased joint wear, and a higher risk of injury during everyday movements. Simple actions — lifting a suitcase, reaching overhead, or bending to pick up a child — place greater strain on a weakened system.
For professionals who travel often and spend long hours seated, this imbalance is not theoretical. It develops gradually over years of desk work and frequent flights. Research in workplace health repeatedly identifies prolonged sitting as a major contributor to increased disc pressure and reduced spinal muscle activity.
Many acute back injuries do not occur during heavy lifting. Instead, they happen during small, unexpected movements — twisting, reaching, or standing quickly from a chair. These movements challenge the deep stabilizing muscles under sudden conditions. Training these stabilizers improves resilience and reduces injury risk during daily life.
The Latissimus Dorsi and Upper Body Output
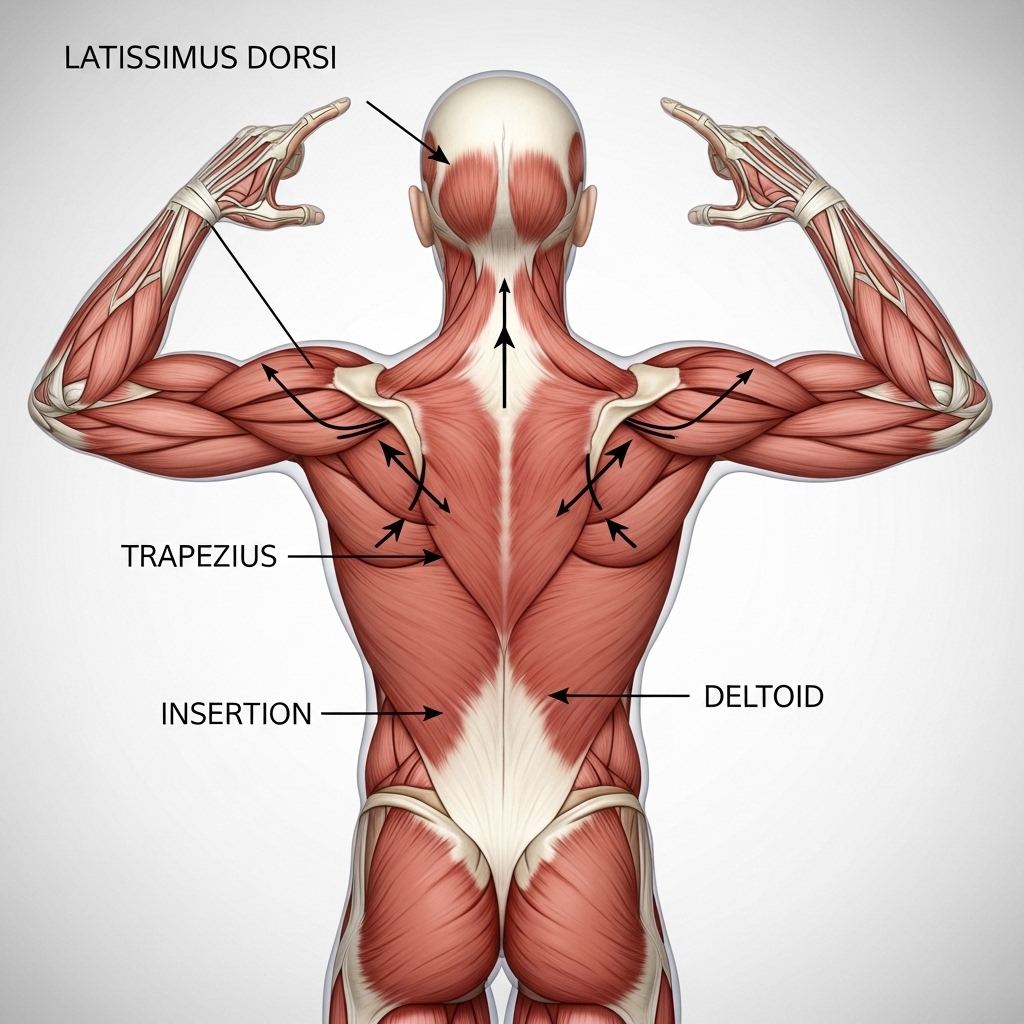
The latissimus dorsi — often called the lats — is the broadest muscle of the back. It connects the upper arm to the lower spine and pelvis, making it one of the longest muscles in the body. Because of this connection, the lap plays a key role in transferring force between the upper and lower body.
It links the arm to the pelvis through a large connective tissue structure called the thoracolumbar fascia. This connection allows the body to generate strength during pulling, climbing, and rotational movements. Weak lats reduce efficiency in these movements and increase stress on the shoulder joints. They also contribute to the rounded-shoulder posture commonly seen in people who spend many hours working at a desk.
Clinically, weak lats are associated with a higher risk of shoulder impingement and reduced strength in pulling or overhead movements. These abilities tend to decline quickly with age when they are not trained deliberately. For professionals who engage in leisure sport or any physical activity, lat strength directly determines both performance and injury resilience in those settings.
The lap also stabilizes the spine during lifting and carrying tasks. When the muscle engages properly, it creates tension through the back fascia that supports the lower spine. When the lap is weak or inactive, this layer of spinal protection disappears. Everyday activities such as carrying luggage or lifting objects from the floor place more strain on the lower back.
Back Muscle Function and Metabolic Health
Skeletal muscle is the body's main site for glucose use during and after exercise. The large muscles of the posterior chain — including the lats, trapezius, and erector spinae — make up a significant portion of total muscle mass. When these muscles weaken or shrink, the body's ability to process glucose decreases.
Over time, this contributes to higher fasting glucose levels and reduced insulin sensitivity. The American Diabetes Association identifies skeletal muscle mass as an important factor in long-term metabolic health. For professionals already exposed to metabolic risks such as stress, poor sleep, and sedentary work, losing posterior chain muscle worsens the situation. Training these muscles therefore improves more than strength and posture. It also supports metabolic stability.
Resistance training that targets large muscle groups stimulates the release of growth hormone and testosterone. These hormonal responses support muscle repair, fat metabolism, and physical recovery. Smaller isolation exercises do not produce the same effect.
For professionals focused on long-term health and performance, this makes posterior chain training an efficient physical investment. The hormonal and metabolic benefits stack directly on top of the structural ones, making each training session more valuable than its structural benefit alone suggests.
The Trapezius, Neck Loading, and Cognitive Performance
The upper trapezius is one of the most overworked muscles in modern professional life. Long hours at a keyboard or screen keep this muscle in constant low-level contraction. Over time, this reduces local blood flow, creates trigger points, and contributes to neck pain and tension headaches. For professionals working many hours each day at a computer, this strain becomes a daily physical load.
The consequences extend beyond discomfort. Neck tension and headaches are known to reduce attention, slow processing speed, and increase mental fatigue during demanding tasks. For leaders whose work depends on sustained concentration and decision-making, chronic neck strain becomes a hidden cognitive performance issue with a direct structural solution.
At the same time, the middle and lower portions of the trapezius are often weak and underused. This imbalance creates instability around the shoulder blades. The upper fibers remain tight and overactive while the middle and lower fibers become inhibited. This drives further mid-back postural collapse and shoulder dysfunction.
Correcting this imbalance requires two steps: releasing the tight upper fibers and strengthening the middle and lower fibres. Rowing movements and shoulder-blade retraction exercises help restore balance. Professionals who address this imbalance often report rapid improvements in neck comfort, headache frequency, and overall work endurance.
What the Research Says About Training Frequency and Method

Clinical research on posterior chain training highlights several consistent findings. Studies published in the Journal of Orthopaedic and Sports Physical Therapy show that targeted stabilizer training improves spinal stability, reduces pain, and enhances movement quality. Exercises that engage both the multifidus and the transverse abdominis produce these improvements. They occur on their own, independent of surface-level strength gains.
Surface-level strength training alone does not fully replace this effect. A professional may perform heavy deadlifts or rows and still lack proper spinal control if the deep stabilisers remain untrained. This gap is common even among physically active professionals. It is one of the most consequential and least addressed weaknesses in the fitness programmes of high performers.
Research also shows that deep stabilisers respond best to frequent activation rather than occasional high-intensity sessions. Short, regular training sessions improve spinal control more effectively than infrequent heavy workouts. This finding aligns with the broader principle that postural and stabilising muscles respond to regularity rather than intensity. Most high performers already apply this logic to professional skill maintenance. The same principle applies directly here.
For the larger posterior chain muscles — including the lats, trapezius, and erector spinae — the evidence supports progressive resistance training combined with varied movement patterns. Horizontal pulling, vertical pulling, and controlled spinal extension each train different aspects of back function. A programme that includes all three provides the most complete structural and metabolic benefits.
Evidence-Based Options for the High-Performing Professional

The research outlined here supports several practical approaches that fit demanding professional schedules. Training the deep spinal stabilisers strengthens the layer most responsible for spinal longevity and injury prevention. Exercises such as bird-dog, dead bug, and controlled extension movements activate the multifidus and other stabilising muscles. These exercises require little equipment and provide meaningful benefit when practised consistently.
Adding horizontal and vertical pulling movements that target the latissimus dorsi and mid-trapezius helps counteract the effects of long hours at a desk. These exercises also improve mid-back mobility and support efficient breathing. For professionals already experiencing signs of posterior chain dysfunction — persistent lower-back tension, mid-back stiffness, frequent neck strain, or unexplained cardiovascular plateaus — assessment by a musculoskeletal physiotherapist or sports medicine specialist can establish a useful baseline.
From there, a targeted training programme can be developed. Each element addresses a specific variable: structural strength, metabolic health, cardiovascular efficiency, or hormonal balance. All of these outcomes can be measured and tracked over time, aligning with the broader performance-focused approach that many professionals already apply to other areas of health within the WholeLiving performance framework.
Chronic posterior chain weakness and spinal muscle loss are among the most direct physical contributors to accelerated biological aging, with paraspinal muscle atrophy linked to raised inflammatory markers, reduced insulin sensitivity, elevated baseline cortisol, and measurable declines in functional capacity — factors that, together, can add an estimated three to five years to biological age in large-scale population studies. WholeLiving's Biological Age Estimation Model incorporates this factor directly — your assessment takes under five minutes.
UP NEXT: Yoga Posture to Align Your Body and Embrace Gratitude
Ready to understand how these factors are influencing your biological age right now? [Take the Biological Age Assessment →]






