Cardiovascular function is the single most consequential biomarker system for sustained executive performance, yet most high-performing professionals treat cardiac health reactively rather than as a measurable, optimizable variable. Subclinical arterial stiffness, elevated resting heart rate variability suppression, and early-stage endothelial dysfunction routinely precede a cardiac event by a decade or more — silently compressing cognitive output, blunting stress resilience, and accelerating biological age. For professionals operating at the intersection of high cognitive load and chronic physiological stress, hearty health is not a background concern. It is a primary performance variable that demands the same rigor applied to business strategy.
Hearty Health Begins With the Heart as a System

The heart is not merely a pump. It is the central delivery system for every mental and physical output a professional depends on. Cardiac output measures the volume of blood the heart ejects each minute. That output determines how much oxygen reaches the prefrontal cortex — the brain region governing decisions, focus, and risk judgment. So when cardiac efficiency drops, even slightly, mental sharpness declines before any symptoms appear.
Research from the Framingham Heart Study links cardiovascular risk factors to faster cognitive decline over time. These factors include elevated blood pressure, abnormal cholesterol levels, and reduced heart rate variability. Notably, these findings are not limited to sick populations. They appear in working-age adults who believe they are perfectly healthy. As a result, the gap between how professionals feel and how their hearts actually function is one of the most overlooked risks in this demographic.
For executives and founders under sustained pressure, the cardiovascular system faces constant demand. Chronic stress activation raises resting heart rate, blunts recovery, and slowly reshapes arterial structure over years. Consequently, hearty health is not simply about avoiding heart attacks. It is about preserving the circulatory function that makes peak performance possible in the first place.
READ ALSO: Hearty Spinach and Chickpea Soup | Whole Living Eat Well
Arterial Stiffness: A Core Hearty Health Marker
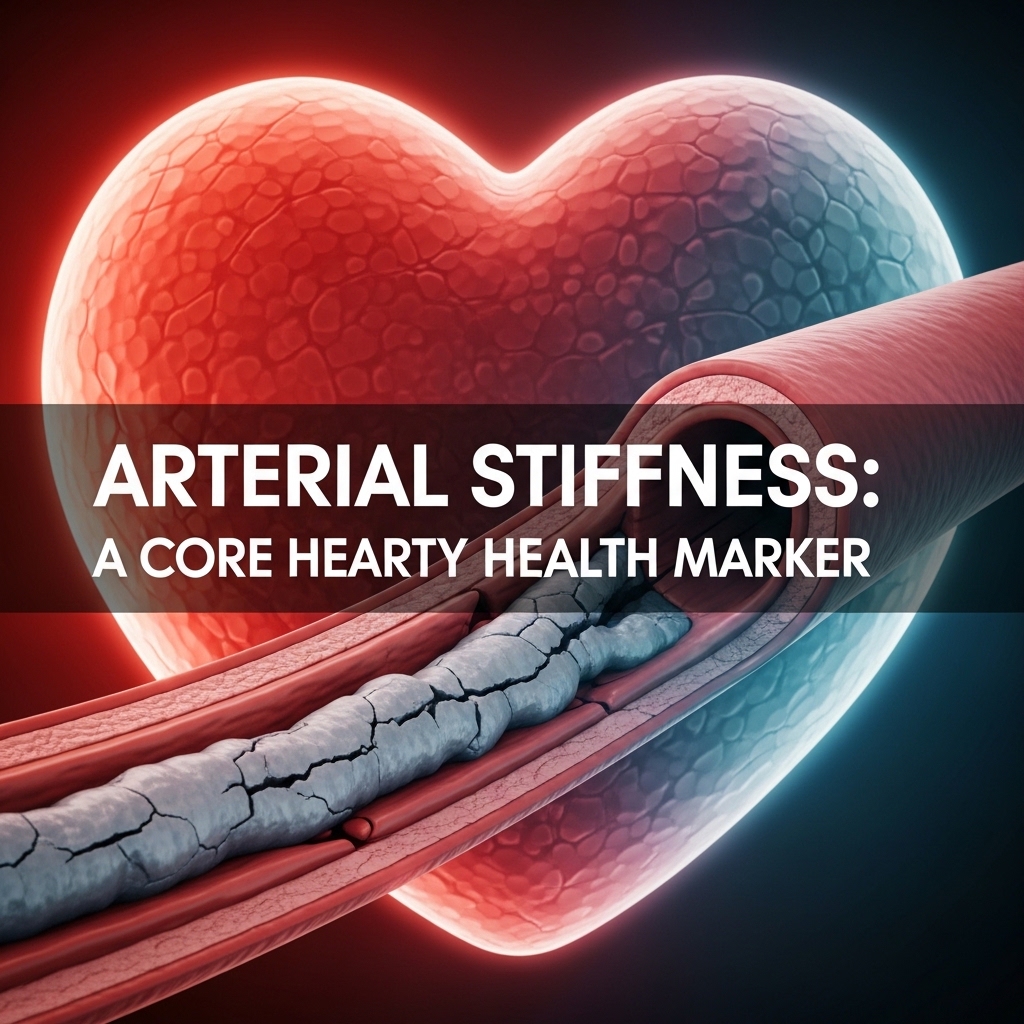
Arterial stiffness is one of the most clinically meaningful and least discussed cardiovascular variables in executive health. When arteries lose their natural flexibility — driven by age, stress, diet, and inflammation — the heart must work harder. This extra workload wears down the heart muscle over time. It also reduces oxygen delivery to the brain and other tissues.
Pulse wave velocity is the clinical tool used to measure arterial stiffness. Moreover, multiple large studies have confirmed it as an independent predictor of cardiovascular events and death from any cause. The American Heart Association now recognizes arterial stiffness as a useful risk tool — one that goes well beyond standard cholesterol readings. For high-performing professionals, this means arterial health is a variable that can be measured and improved, not simply accepted as part of aging.
The drivers of arterial stiffness map directly onto the daily conditions of high-output professional life. Elevated cortisol, poor sleep, long periods of sitting, and high-sugar diets each contribute independently to stiffening of the arterial walls. Together, however, their combined effect is not additive — it is multiplying. Vascular aging accelerates at rates that standard annual check-ups are not built to catch. This is why hearty health demands more than routine care.
Heart Rate Variability and Hearty Health Readiness
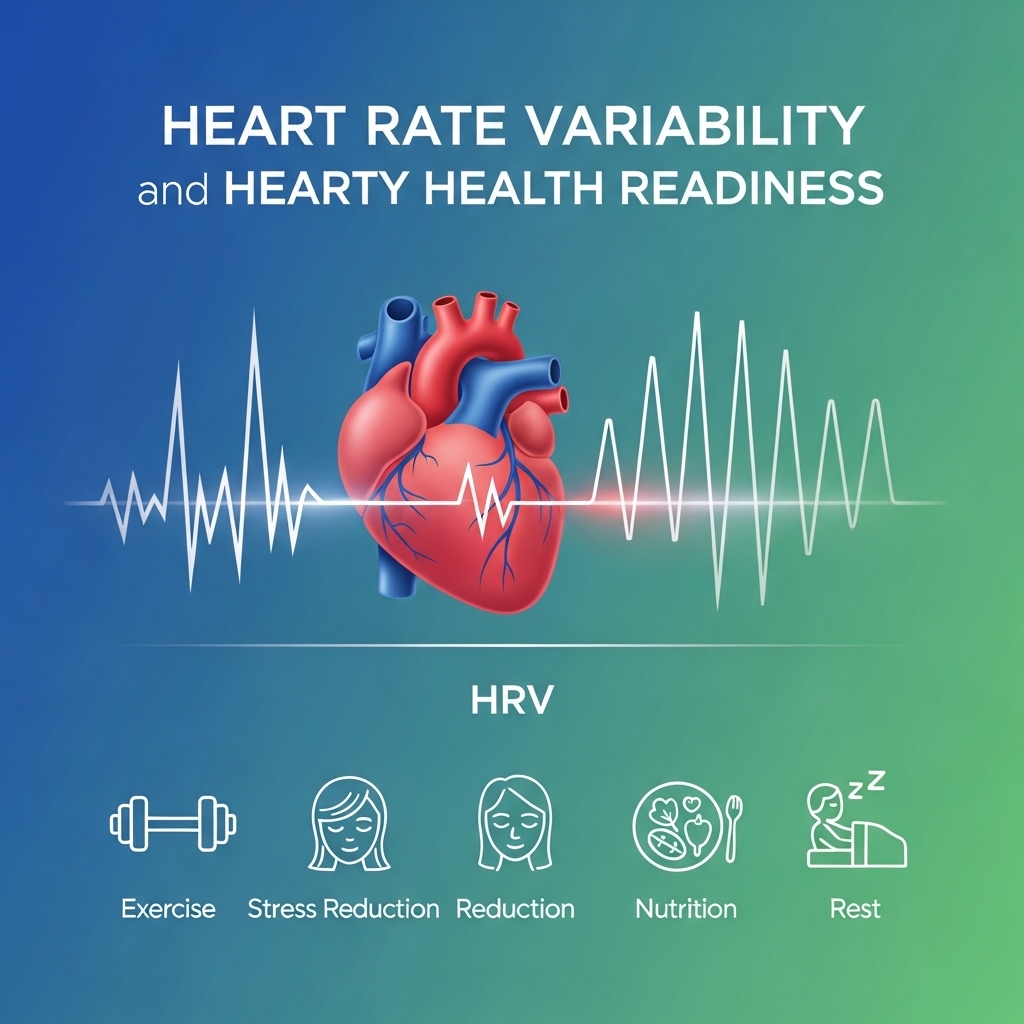
Heart rate variability, or HRV, measures the time variation between consecutive heartbeats. It may sound like a small detail. Yet HRV is one of the most sensitive, non-invasive signals of nervous system balance, recovery capacity, and overall resilience. As a result, a chronically low HRV reliably signals that the body is running under high stress with too little recovery.
Research published in the Journal of the American College of Cardiology links reduced HRV to higher risk of atrial fibrillation, sudden cardiac events, and death from any cause. Beyond those clinical risks, low HRV in otherwise healthy individuals also correlates with reduced mental flexibility, slower reactions, and weaker emotional control. All three directly affect professional decision-making under pressure. HRV is therefore not just a heart metric — it is a real-time signal of how much capacity a person has available.
For professionals who track performance through output, HRV offers a biologically grounded alternative measure. It responds quickly to lifestyle inputs. Sleep quality, alcohol intake, training load, and psychological stress all produce measurable HRV shifts within 24 to 72 hours. This fast response makes HRV a practical tool for monitoring the cardiac cost of a demanding professional schedule — not just a theoretical data point.
READ ALSO: Female Heart Attack Pain Isn’t Always What You Expect
VO2 Max, Hearty Health, and Long-Term Survival
VO2 max measures the maximum rate at which the heart, lungs, and muscles can use oxygen during effort. It is the most well-supported single predictor of cardiovascular longevity in the research literature. Additionally, VO2 max declines with age when left unaddressed. However, the rate of that decline is highly responsive to training behavior.
A landmark study published in JAMA Network Open found that cardiorespiratory fitness — as measured by VO2 max — predicted long-term death rates more strongly than high blood pressure, diabetes, smoking, or heart disease in a large adult cohort. Furthermore, the benefit of moving from low to moderate fitness was comparable to — and in some analyses greater than — the survival benefit of quitting smoking. These findings are not minor refinements. They call for a fundamental shift in which health variables professionals treat as priorities.
For professionals between 35 and 60, a declining VO2 max compresses both lifespan and the years of healthy function. Aerobic capacity is therefore not a fitness vanity metric. It is a core measure of how long and how well the cardiovascular system can sustain high-level work. Hearty health, viewed through this lens, is measurable, targeted, and improvable through structured effort.
Inflammation, Lipid Levels, and Hearty Health Risk
Standard lipid panels — total cholesterol, LDL, HDL, and triglycerides — are the most commonly ordered heart tests in routine care. Yet they are not sufficient on their own for meaningful cardiac risk assessment in high-performing professionals. Advanced lipid testing, including apolipoprotein B (ApoB), lipoprotein(a), and LDL particle count, gives a far more accurate picture of artery disease risk than standard values alone.
Systemic inflammation also drives cardiovascular disease as an independent force. Measured through high-sensitivity C-reactive protein (hs-CRP) and interleukin-6 levels, it operates silently. The JUPITER trial — a major randomized controlled study — found that people with elevated hs-CRP but normal LDL cholesterol still faced significantly higher cardiac risk. Moreover, lowering inflammatory burden produced real reductions in cardiac events. Inflammation is therefore not a secondary issue — it is a primary one that routine panels routinely miss.
For professionals carrying high cognitive and work demands, low-grade chronic inflammation is an occupational hazard. Poor sleep, ongoing psychological stress, processed food diets, and inadequate recovery all sustain an inflamed state. The cardiac consequences build quietly over years. Tracking inflammatory markers alongside advanced lipid data thus gives a far more complete and useful cardiac risk picture than standard annual blood tests deliver.
Sleep Quality and Hearty Health Recovery

The link between sleep and hearty health runs in both directions, and the clinical evidence is strong. During deep slow-wave sleep, heart rate and blood pressure drop in a natural nightly cycle. This drop allows the cardiovascular system to lower its workload, clear waste products, and recover its autonomic balance. Professionals who chronically sleep poorly or too briefly cut this repair window short.
Research from the National Institutes of Health and multiple large cohort studies shows that when blood pressure fails to dip at night — a pattern called non-dipping — cardiovascular events, stroke, and heart wall thickening all become more likely. Non-dipping patterns appear most often in people with chronic sleep disruption, shifting schedules, or high stress at night. These are conditions that many executives managing global teams know well.
Sleep quality — not just total sleep hours — determines how much time is spent in the stages that matter most for heart recovery. Today, wearable devices can track sleep architecture with enough detail to flag low HRV, elevated resting heart rate, and breathing problems — all early signs of cardiovascular strain. For professionals who still treat sleep as optional, the cardiac data frames the issue in terms that are hard to dismiss.
READ ALSO: Heart-Healthy Mediterranean Diet Recipes – Whole Living Eat Well
Cortisol, Stress Load, and Hearty Health

Cortisol is the body's primary stress hormone, and its effects on the heart are well documented. In short, controlled bursts, cortisol helps the cardiovascular system adapt — raising heart rate, increasing blood output, and releasing fuel. But under chronic, unrelenting professional stress, cortisol disruption produces sustained blood vessel tension, arterial inflammation, and faster vascular aging.
Persistently high cortisol links to increased belly fat, insulin resistance, abnormal cholesterol, and high blood pressure — a group of metabolic problems that all hit the cardiovascular system at once. Furthermore, the Harvard T.H. Chan School of Public Health has published research connecting chronic psychological stress and cortisol burden to greater atherosclerotic plaque growth. This connection holds even after accounting for traditional risk factors. It is visible in imaging studies of high-stress professional groups.
For high-output professionals, this means workload management carries direct cardiac weight. The nervous system does not distinguish between a board meeting and a physical threat. Repeated stress activation without adequate recovery is therefore a direct driver of cardiovascular aging. Managing that activation pattern is, in the most literal sense, a heart health intervention.
Metabolic Health and Hearty Health Function

Metabolic health and cardiovascular health are tightly linked — not separate systems running in parallel. Insulin resistance, even without a diabetes diagnosis, damages blood vessel lining, raises triglycerides, lowers HDL, and promotes the most harmful form of LDL cholesterol. Each of these effects adds independently to cardiac risk. A professional with normal body weight but underlying insulin resistance may thus carry a far higher cardiac risk than standard tests reveal.
Fasting insulin and HOMA-IR — a calculated measure of insulin resistance — rarely appear in standard annual blood panels. Yet they are among the most informative metabolic markers available. Similarly, post-meal blood sugar spikes — which continuous glucose monitors can now track non-invasively — cause repeated episodes of oxidative stress and blood vessel damage. These accumulate over years. The link between blood sugar control and vascular health is one of the most well-understood mechanisms in cardiovascular science.
Body composition adds another layer to this risk. Specifically, the ratio of belly fat to lean muscle matters more than body weight alone. Belly fat actively releases inflammatory signals and free fatty acids. These directly impair blood vessel function and raise dyslipidemia risk. For professionals in their 40s and 50s — where age-related muscle loss and stress-driven fat gain often occur together — this creates a compounding cardiac risk that active metabolic monitoring can address early.
Cardiac Imaging and Advanced Hearty Health Screening
Standard stress tests and resting electrocardiograms identify cardiac dysfunction that has already developed. They are not built to catch the early changes that precede clinical events by years or decades. For professionals seeking genuine early detection, advanced cardiac imaging offers a meaningfully different level of insight. Coronary artery calcium (CAC) scoring uses low-dose CT to measure calcified plaque in the coronary arteries. It also provides a cardiovascular event risk estimate independent of age and sex.
A CAC score of zero carries a very different prognosis than a score above 400, even when standard lipid profiles look similar. Blood tests alone cannot capture this distinction. Cardiac MRI adds a further layer, detecting early structural changes — including hypertrophy, fibrosis, or infiltrative disease — that standard imaging cannot see. For professionals managing demanding schedules and high physiological load, these tools provide the specific, actionable data that routine clinical care does not deliver.
The value of advanced imaging grows further when combined with biomarker data, lifestyle tracking, and repeat measurements over time. A single CAC score gives one data point. Serial scores, however, reveal the rate of change — which is arguably more useful than any single reading. Professionals who rely on dashboards to manage complex systems will immediately recognize this logic. Point-in-time snapshots are not enough for managing a dynamic, compounding variable like hearty health.
READ ALSO: Heart-Smart Workout: Get Fit
Building a Hearty Health Monitoring Protocol

The evidence from cardiovascular science, metabolic research, sleep medicine, and stress biology all points to one clear principle: hearty health is a systems-level variable that requires systems-level attention. For high-performing professionals, the starting point is a full cardiovascular assessment that goes well beyond standard annual bloodwork. Specifically, this means adding advanced lipid analysis, inflammatory markers, fasting metabolic indices, HRV tracking, and cardiac imaging where clinically appropriate.
Beyond testing, the lifestyle inputs with the strongest evidence for cardiovascular benefit include structured aerobic training to maintain or improve VO2 max, resistance training to preserve muscle mass and metabolic function, and dietary patterns that keep blood sugar stable and support blood vessel health. Additionally, sleep protocols that protect both duration and architecture belong in this list. The evidence behind each of these inputs spans multiple independent research lines and decades of longitudinal data.
Professionals who bring the same analytical rigor to their cardiovascular health that they apply to financial or operational risk are well positioned to act early and effectively. The window between subclinical dysfunction and clinical disease spans years — sometimes decades. Advanced screening tools, paired with evidence-based lifestyle inputs and consistent biomarker tracking, allow that window to be found and used. Hearty health, managed at this level, becomes a measurable asset — not a background assumption.
UP NEXT: Whole-Wheat Penne with Sausage, Chard, and Artichoke Hearts | Whole Living Eat Well
Sustained cardiovascular strain — marked by elevated resting heart rate, suppressed heart rate variability, and rising arterial stiffness — is one of the most consistent drivers of accelerated biological aging, with poor hearty health linked to measurable increases in vascular age that frequently run five or more years ahead of chronological age in high-stress professional populations. WholeLiving's Biological Age Estimation Model incorporates this factor directly — your assessment takes under five minutes.
Ready to understand how these factors are influencing your biological age right now? [Take the Biological Age Assessment →]






