Skin barrier degradation is not a cosmetic inconvenience — for professionals operating under chronic stress loads, it is a measurable signal of systemic NAD+ depletion and accelerated cellular aging. Niacinamide uses for skin extend well beyond surface-level hydration; at the biochemical level, this form of vitamin B3 directly supports mitochondrial function, modulates inflammatory cytokine activity, and reinforces the stratum corneum's integrity against cortisol-driven collagen breakdown. For executives and founders whose biological age increasingly diverges from chronological age, understanding niacinamide's clinical applications is a matter of performance optimization, not vanity.
Niacinamide Uses for Skin Start at the Cellular Level
Niacinamide — also called nicotinamide — is one of two main forms of vitamin B3. The other is nicotinic acid, or niacin.
Both forms act as precursors to NAD+, but they work through distinct metabolic pathways. Niacinamide does not produce the flushing response that niacin causes. This makes it easier to tolerate over sustained use.
Its role as an NAD+ precursor places it at the center of cellular energy metabolism, DNA repair, and sirtuin activation — three processes central to current longevity research.
NAD+ Decline Accelerates Biological Age

NAD+ levels fall steadily with age. Research from the National Institutes of Health has documented declines of up to 50% between early adulthood and midlife.
This depletion does not merely reflect aging — it actively drives it. NAD+ activates PARP enzymes, which coordinate DNA damage repair, and sirtuins, which regulate gene expression, mitochondrial biogenesis, and inflammatory response. When NAD+ falls below functional thresholds, these systems underperform. The result is a measurable gap between chronological age and biological age — a metric that longevity-focused clinicians now track directly.
Niacinamide replenishes NAD+ pools in skin and peripheral tissue, making it relevant for professionals whose biological age metrics are running ahead of their calendar age.
How Niacinamide Uses for Skin Extend Beyond the Surface
The most studied niacinamide uses for skin involve barrier integrity, pigmentation control, and sebaceous activity. These are not purely cosmetic outcomes. Skin is the body's largest organ and its primary buffer against environmental stressors — UV radiation, pollution, and pathogenic exposure.
A compromised barrier does not just cause dryness. It generates chronic low-grade inflammation that raises systemic cytokine levels, including interleukin-1 (IL-1) and tumor necrosis factor-alpha (TNF-α). For professionals already carrying elevated cortisol loads, this inflammatory signal compounds existing physiological stress.
Research in the Journal of Investigative Dermatology has examined niacinamide's capacity to raise ceramide synthesis. Ceramides are the lipid class most responsible for holding the skin's outer layer together. When ceramide production is adequate, the skin retains moisture, resists inflammatory triggers, and maintains structural integrity. Studies show that consistent topical niacinamide use increases measurable ceramide levels within four to eight weeks.
Collagen Loss as a Connective Tissue Variable
Collagen is not simply a structural protein for appearance. It supports vascular integrity, wound healing speed, and tissue resilience throughout the body. Dermal collagen synthesis peaks in the mid-twenties and then declines at roughly 1% per year.
Cortisol — chronically elevated in high-demand professional environments — directly suppresses fibroblast activity. Fibroblasts are the cells that produce collagen. Niacinamide counteracts this suppression by stimulating fibroblast proliferation and increasing the expression of type I and type III collagen genes in dermal tissue.
For professionals in their forties and fifties, maintaining dermal density reflects broader connective tissue health across cardiovascular and musculoskeletal systems.
Niacinamide for Skin Pigmentation and Oxidative Stress

Uneven skin pigmentation is, in clinical terms, a marker of cumulative oxidative stress and DNA damage in melanocytes. Niacinamide does not block melanin synthesis directly. Instead, it interrupts the transfer of melanosomes from melanocytes to surrounding keratinocytes — the mechanism by which pigment becomes visible at the skin surface. This means niacinamide regulates pigmentation without disrupting the melanocyte's broader protective function.
Photoaging — the accelerated structural breakdown of skin from UV exposure — is now used in longevity medicine as a proxy for systemic oxidative stress burden.
Research from the American Academy of Dermatology links accelerated photoaging scores with elevated inflammatory biomarkers and reduced antioxidant capacity in peripheral blood. Addressing photoaging through niacinamide therefore reduces one measurable component of total oxidative load.
Sebaceous Activity as a Metabolic Signal
Excess sebum production has metabolic roots. Sebaceous glands respond to androgens and insulin-like growth factor 1 (IGF-1) — both of which rise in states of insulin resistance and metabolic dysregulation.
Niacinamide reduces sebaceous output by modulating gland sensitivity to androgenic signaling. This happens without hormonal intervention.
For professionals in midlife navigating metabolic shifts, sebum regulation serves as a peripheral signal of broader endocrine stability.
Inflammatory Biomarkers and Systemic Risk
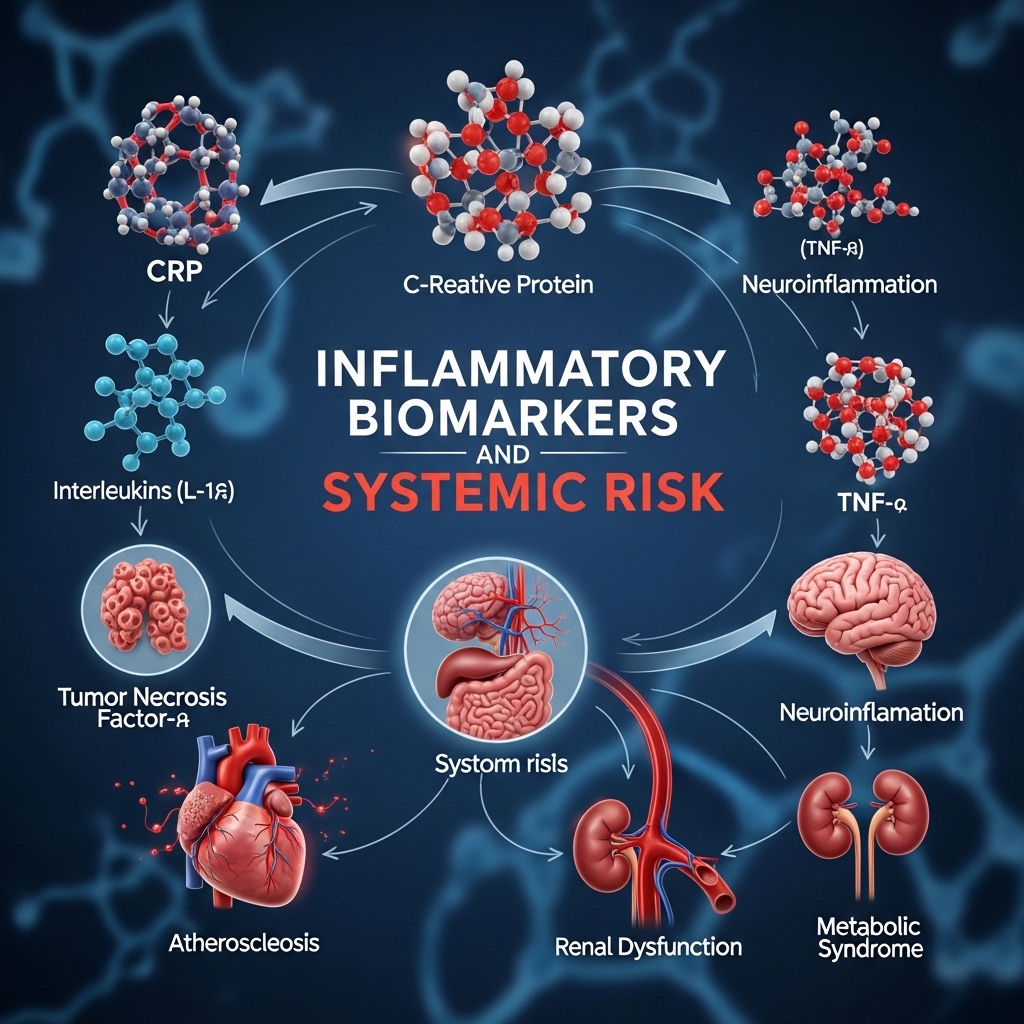
Chronic low-grade inflammation — measured through high-sensitivity C-reactive protein (hs-CRP), interleukin-6, and fibrinogen — is one of the most consistent predictors of accelerated biological aging and cardiovascular risk.
The Framingham Heart Study and its derivative research have identified chronic inflammation as a key mediating factor in atherosclerosis, cognitive decline, and all-cause mortality in midlife populations. Niacinamide reduces inflammatory activity through several pathways.
It suppresses NF-κB activation, decreases pro-inflammatory cytokine expression in keratinocytes, and shifts macrophage behavior toward anti-inflammatory patterns. These mechanisms are systemic. Interventions that reduce inflammation in skin also reduce its total contribution to the body's inflammatory load.
Cognitive Performance and Neural NAD+ Demand

The brain is among the most metabolically demanding organs in the body. Neural tissue is acutely sensitive to NAD+ availability. Declining NAD+ in neural cells correlates with impaired mitochondrial efficiency, accumulating oxidative DNA damage, and reduced SIRT1 and SIRT3 activity — sirtuins linked to neuroprotection and synaptic plasticity.
Research from the National Institute on Aging has examined how NAD+ precursor supplementation affects cognitive markers in aging animal models. Findings suggest improvements in memory consolidation and reductions in neuroinflammatory markers.
Human data remains in earlier stages, but the mechanistic case for niacinamide's relevance to cognitive performance in midlife professionals rests on established neuroscience. Executive function, working memory, and decision-making velocity all depend on NAD+ status — a variable now trackable through clinical testing.
Sleep, Cellular Repair, and NAD+ Availability
Sleep is the primary window for cellular repair. NAD+-dependent DNA repair processes, including PARP and sirtuin activity, peak during deep sleep stages. Disrupted sleep architecture — common in high-demand environments — compresses these repair windows.
Niacinamide supports NAD+ availability during these periods. It does not act as a sedative.
Its contribution to sleep quality is indirect: reducing inflammatory signaling and supporting parasympathetic tone creates a better biochemical environment for the repair processes that deep sleep is designed to facilitate.
READ ALSO: Salicylic Acid and Skin Barrier Integrity: What High-Stress Professionals Need to Understand
Comparing Topical and Oral Niacinamide for Skin and Systemic Outcomes

Topical and oral niacinamide produce different concentration gradients and tissue-level effects. Topical application delivers high local concentrations to the epidermis and upper dermis. This makes it most effective for barrier function, ceramide synthesis, pigmentation control, and sebaceous regulation — the core niacinamide uses for skin at the surface level.
Oral niacinamide enters systemic circulation and contributes to NAD+ pools across multiple tissue types, including neural, cardiovascular, and musculoskeletal tissue. The two delivery methods are not redundant.
They address different targets and can run concurrently without interaction. Professionals seeking both dermal and systemic outcomes may find that a combined approach, under physician guidance, covers the broadest range.
READ ALSO: Selecting the Correct Facial Toner Preserves Skin Barrier Integrity and Delays Epidermal Aging
Tolerability and Formulation Stability

One clinical advantage of niacinamide over other active compounds in longevity protocols is its tolerability profile. Unlike retinoids, which require careful titration and can temporarily compromise the skin barrier, niacinamide is well-tolerated across skin types. It requires no UV-avoidance protocols. It is water-soluble, stable in formulation, and compatible with most other active compounds. Older literature flagged a theoretical interaction between niacinamide and high-dose ascorbic acid, suggesting the two might form a discolored complex. Current research shows this reaction carries minimal clinical concern at standard concentrations and does not reduce the efficacy of either compound.
READ ALSO: Best Vitamin C Serum for Gentle Radiance
Applying the Evidence: Practical Directions for High-Performing Professionals

For professionals who treat skin health as a systemic indicator rather than an aesthetic metric, the evidence points toward several practical directions. Topical niacinamide at concentrations studied in peer-reviewed dermatology research addresses barrier degradation, inflammatory skin signaling, and collagen support simultaneously — three of the core niacinamide uses for skin with measurable systemic relevance. Oral niacinamide, as part of a broader NAD+ precursor strategy, warrants direct conversation with a physician — particularly for those who track biological age scores or monitor inflammatory biomarkers as part of an executive health program. Baseline assessment of relevant markers — including hs-CRP, biological age testing, and dermal density imaging where available — provides the clearest framework for determining where niacinamide fits within an individualized protocol. Population averages rarely reflect individual physiology at this level of precision; personal data remains the most reliable guide.
UP NEXT: Korean Skin Care Secrets for Glowing, Healthy Skin
Sustained NAD+ depletion — accelerated by chronic stress, UV exposure, and compromised skin barrier function — is a measurable driver of biological age divergence, with research linking systemic nicotinamide deficiency to accelerated cellular aging across dermal, neural, and cardiovascular tissue. WholeLiving's Biological Age Estimation Model incorporates this factor directly — your assessment takes under five minutes.
Ready to understand how these factors are influencing your biological age right now? [Take the Biological Age Assessment →]






