Pharyngeal inflammation — commonly dismissed as a minor inconvenience — carries measurable consequences for executive performance that most high-functioning professionals systematically underestimate. Elevated inflammatory cytokines associated with throat pathology directly impair cognitive processing speed, disrupt sleep architecture, and elevate systemic cortisol, compressing the recovery window available to an already-taxed nervous system. For professionals operating at peak cognitive load, even a 48-hour inflammatory episode can degrade decision-making accuracy and working memory retention. Understanding evidence-based throat pain remedies is not a matter of comfort management — it is a strategic intervention with direct implications for sustained cognitive output and immune resilience.
The Inflammatory Cascade Behind Throat Pain
Pharyngeal pain signals a broader inflammatory process — not an isolated symptom. When the pharyngeal epithelium is compromised by viral pathogens, bacterial colonization, or environmental irritants, the immune system initiates a cytokine release cascade. Pro-inflammatory markers including interleukin-6 (IL-6) and tumor necrosis factor-alpha (TNF-α) mobilize rapidly, triggering vasodilation, tissue swelling, and pain that signals tissue damage.
For high-performing professionals, this cascade carries consequences beyond the throat itself. National Institutes of Health research documents that systemic IL-6 elevations — even those from localized pharyngeal inflammation — increase HPA axis activity. This directly disrupts cortisol regulation, compressing recovery capacity during an active inflammatory episode.
Left unmanaged, prolonged inflammation extends cytokine elevation and increases cumulative inflammatory burden. Professionals already carrying chronic low-grade systemic inflammation compound acute episodes with chronic ones. Longevity researchers call this pattern inflammaging: the chronic inflammatory state linked to accelerated biological aging.
Why Standard Over-the-Counter Approaches Fall Short

The default response to throat pain — NSAIDs and topical anesthetic lozenges — addresses symptoms without engaging the immune resolution process. NSAIDs inhibit COX enzymes and reduce prostaglandin synthesis, but they do not accelerate viral clearance or restore mucosal barrier integrity. Symptom suppression is not biological resolution.
Repeated NSAID use in executive populations carries additional considerations. Harvard T.H. Chan School of Public Health research links chronic NSAID use to gut mucosal compromise, renal stress markers, and elevated cardiovascular risk. Professionals already managing cardiovascular risk factors miss a real optimization opportunity when bypassing evidence-based natural throat pain remedies.
Topical anesthetics present a separate limitation. Benzocaine and lidocaine-based formulations reduce pain signal transmission but provide no antimicrobial, anti-inflammatory, or mucosal repair action. Both function as a performance mask rather than a biological solution.
The Mucosal Barrier as a Performance Asset

The pharyngeal mucosa is an active immune interface, not a passive anatomical structure. Secretory immunoglobulin A (sIgA), the primary antibody at mucosal surfaces, serves as the first line of defense against inhaled and ingested pathogens. Maintaining mucosal barrier integrity directly determines how often pharyngeal inflammation occurs and how rapidly resolution follows.
Chronic psychological stress — the defining physiological condition of executive environments — measurably suppresses sIgA secretion. Carnegie Mellon University's laboratory studies on stress and illness susceptibility document this mechanism clearly. That same stress physiology driving professional performance degrades the mucosal immune response protecting against throat infections.
Reframing throat pain remedies through the lens of mucosal barrier support changes the strategic options available. Interventions that restore sIgA secretion, reinforce mucosal hydration, and support epithelial repair work at the causal level. Here, evidence-based natural approaches offer clinically meaningful advantages over standard over-the-counter options.
Osmotic and Mechanical Interventions: Saline and Irrigation
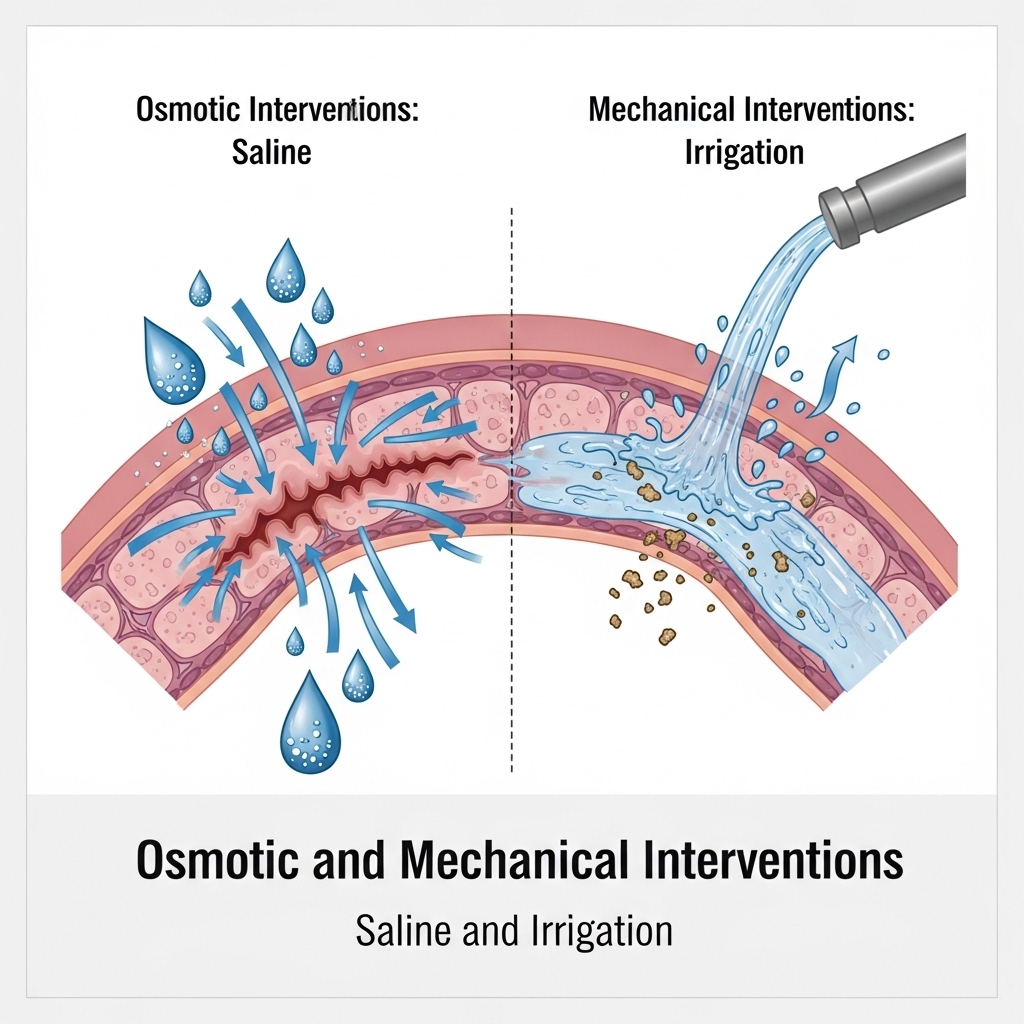
Saline gargling ranks among the most clinically validated throat pain remedies available. Its osmotic action draws inflammatory fluid from swollen pharyngeal tissue, reducing edema and clearing pathogenic load from mucosal surfaces. A randomized controlled trial in the American Journal of Preventive Medicine showed regular saline gargling significantly reduced upper respiratory tract infection rates in healthy adults.
The mechanical component adds further benefit. Turbulence created during gargling physically disrupts biofilm formation on the pharyngeal wall, reducing bacterial adhesion before deeper infection can establish. This matters especially for frequent travelers — an environment associated with reduced mucosal humidity and elevated pathogen exposure.
Nasal saline irrigation addresses an upstream source of many pharyngeal inflammatory episodes: post-nasal drip. When nasal mucosa is irritated, drainage along the posterior pharyngeal wall sustains local inflammation long after initial symptom onset. Regular irrigation in high-travel populations reduces this cycle and shortens symptomatic duration.
Honey: Clinical Evidence Beyond Traditional Use

Raw honey — particularly Manuka honey graded by methylglyoxal (MGO) content — holds a unique position among evidence-supported throat pain remedies. Its clinical relevance is supported by hydrogen peroxide-mediated antimicrobial activity, osmotic bacterial inhibition, and direct anti-inflammatory action on pharyngeal tissue. Research published in BMJ Evidence-Based Medicine found honey more effective than standard over-the-counter treatments for upper respiratory symptoms, including throat discomfort.
Manuka honey's anti-inflammatory mechanism is directly relevant for performance-focused professionals. Its polyphenol content — including luteolin and quercetin — modulates NF-κB signaling, a central pathway governing pro-inflammatory cytokine production. Downregulating this pathway may shorten the period of elevated IL-6 and TNF-α, reducing systemic inflammatory burden and its effects on cortisol regulation and cognitive function.
Beyond acute episodes, high-grade honey coats pharyngeal epithelium, reducing irritant exposure while healing progresses. For professionals who rely on vocal performance — an underappreciated asset for executives and public communicators — this mucosal coating delivers both symptomatic and structural benefit. Synthetic lozenges offering analgesia alone cannot replicate this combined action.
Ginger and Its Bioactive Compounds

Ginger, standardized for gingerol and shogaol content, demonstrates well-characterized anti-inflammatory and analgesic properties relevant to pharyngeal inflammation. Gingerols inhibit prostaglandin synthesis through COX enzyme modulation while also inhibiting leukotriene synthesis — a dual-pathway action that pharmaceutical NSAIDs do not replicate. This dual profile makes ginger a mechanistically strong component of evidence-informed throat pain remedies.
University of Sydney research has examined ginger's antimicrobial properties against respiratory pathogens. Fresh ginger extract showed activity against human respiratory syncytial virus in cellular models. While in vitro evidence requires careful clinical extrapolation, the convergence of anti-inflammatory, analgesic, and antimicrobial mechanisms positions ginger as a functionally broad intervention.
Consumed as a concentrated infusion of fresh rhizome steeped in hot water, ginger delivers active compounds alongside mucosal humidification from steam and fluid intake. Mucosal dehydration — common after air travel and extended time in climate-controlled offices — independently impairs pharyngeal immune defense. Addressing both variables simultaneously strengthens the overall intervention.
Licorice Root and Mucosal Demulcents

Licorice root contains glycyrrhizin — a compound with documented anti-inflammatory, antiviral, and demulcent properties. As a demulcent, it coats inflamed mucous membranes directly, providing structural protection and pain reduction through a mechanism distinct from analgesic drugs. Research on glycyrrhizin has demonstrated antiviral activity against respiratory viruses, including influenza strains, through inhibition of viral replication pathways.
The mucosal demulcent category — including licorice root, marshmallow root, and slippery elm — forms a pharmacologically coherent class of throat pain remedies. High-molecular-weight polysaccharides create a protective gel layer on mucosal surfaces, reducing irritant contact and supporting epithelial repair. This action suits the maintenance phase of recovery, following initial antimicrobial and anti-inflammatory interventions.
For executive professionals, demulcent interventions carry one clear practical advantage: no documented cognitive performance penalties. Sedating antihistamines and some systemic anti-inflammatory medications can dull cognitive output. Demulcents are well-suited to professionals requiring sustained high-level function during active inflammation episodes.
Sleep Architecture, Immune Resolution, and the Recovery Window
Immune resolution is an active biological program — not a passive process. Full execution requires adequate sleep architecture. When pharyngeal inflammation disrupts sleep through pain, mouth breathing, or airway changes from mucosal swelling, resolution slows and symptomatic duration extends.
University of California, San Francisco research published in Sleep journal documented a clear dose-response relationship between sleep duration and upper respiratory infection susceptibility. Individuals sleeping fewer than six hours nightly were significantly more susceptible to clinical illness than those sleeping seven or more hours. An active pharyngeal episode compounds an already-limited recovery window for professionals on compressed sleep schedules.
Protecting sleep quality during active throat inflammation is a direct intervention in the immune resolution pathway. Maintaining sleep environment humidity above 40 percent, elevating head position to reduce post-nasal drainage, and minimizing evening cortisol elevation all support the sleep architecture required for immune resolution. These structural steps carry measurable downstream effects on recovery duration and inflammatory marker clearance.
Hydration, Mucosal Humidity, and Symptom Duration
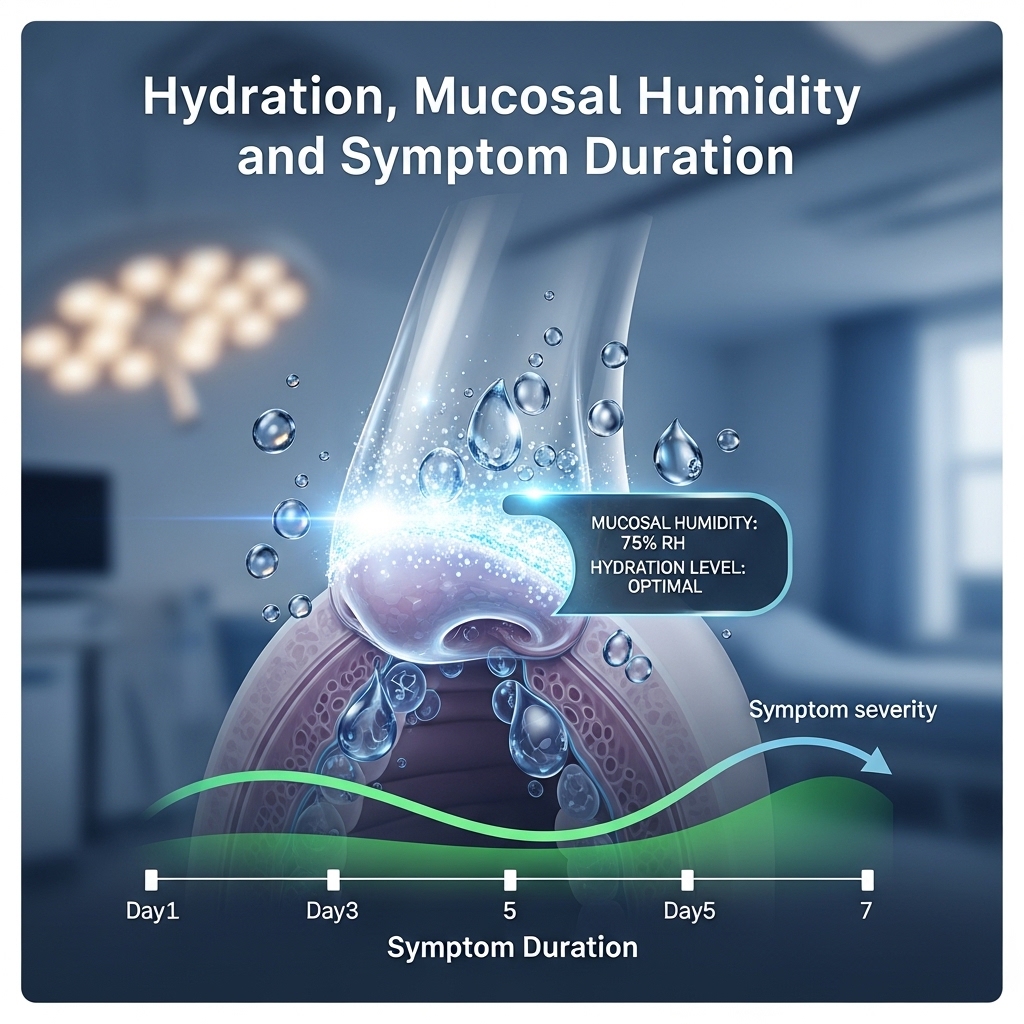
Adequate systemic hydration is among the most consistently supported variables in upper respiratory inflammation management. At the pharyngeal level, it maintains mucosal viscosity, supports ciliary function, and facilitates lymphatic clearance of inflammatory fluid. Subclinical dehydration — common in travel-heavy professional schedules — measurably impairs all three functions.
Environmental humidity matters equally. Clinical otolaryngology research consistently documents that low ambient humidity — characteristic of pressurized aircraft cabins and climate-controlled offices — reduces mucosal surface hydration independently of fluid intake. Drinking more water alone does not fully correct this localized vulnerability.
For high-travel professionals, managing ambient humidity during flight and in hotel sleep environments is a structural component of mucosal health maintenance. Portable humidifiers and saline nasal sprays used during long-haul travel address the environmental dehydration mechanism directly. Used proactively, both function as preventive throat pain remedies rather than reactive treatments.
READ ALSO: Secret Kitchen Cures
Zinc and Immune Competence

Zinc ranks among the most extensively studied micronutrients in upper respiratory immune function. Its role in T-cell development, natural killer cell activity, and cytokine regulation makes it a foundational variable in immune competence. The Cochrane Collaboration's systematic review on zinc for the common cold documented that supplementation initiated within 24 hours of symptom onset significantly reduced illness duration in healthy adults.
Zinc's antiviral mechanism includes direct inhibition of viral replication through interference with viral polyprotein processing. This operates independently of the adaptive immune response and is relevant in the early hours of symptom onset. Zinc acetate lozenges — the formulation with the strongest evidence base — maintain sustained zinc ion contact with pharyngeal mucosal surfaces throughout dissolution.
Zinc status in high-performing professional populations warrants monitoring. Chronic stress physiology increases urinary zinc excretion through cortisol-mediated mechanisms, meaning professionals with sustained cortisol elevation may carry subclinical zinc insufficiency. Regular serum zinc assessment is a practical step in performance-oriented health management.
READ ALSO: 15 Natural Remedies for the Winter Season – Whole Living Wellness
Vitamin D, Mucosal Immunity, and Seasonal Vulnerability

Vitamin D's role in innate mucosal immunity is well-established. Receptors for vitamin D sit on upper respiratory tract epithelial cells, and vitamin D signaling directly increases production of antimicrobial peptides — including cathelicidins and defensins — that form a critical first-line mucosal defense. A meta-analysis in the British Medical Journal found that vitamin D supplementation significantly reduced acute respiratory tract infection risk across a pooled population of over 11,000 participants.
The seasonal pattern of throat infections correlates directly with the seasonal decline in serum 25-hydroxyvitamin D levels. High-performing professionals spending most working hours indoors may face this vulnerability year-round, not only in winter. Chronic vitamin D insufficiency quietly erodes mucosal immune competence across all seasons.
Establishing baseline 25-hydroxyvitamin D status through standard laboratory testing provides the objective foundation for evidence-informed decisions. This relationship between serum vitamin D levels and mucosal immune function is measurable and modifiable. Both variables directly influence the frequency and resolution speed of pharyngeal inflammation episodes throughout the year.
READ ALSO: Foods to Avoid Eating with Acid Reflux for Daily Comfort
Evidence-Based Options for the High-Performing Professional

The evidence across this article supports a framework that prioritizes biological resolution over symptomatic suppression. Mucosal barrier support strategies — saline irrigation, systemic and environmental hydration, and demulcent interventions — work most effectively as baseline protective measures, not reactive responses. Early use of zinc acetate lozenges within the first 24 hours of symptom onset, combined with Manuka honey and ginger infusion, addresses both viral replication and the cytokine cascade driving performance impairment. Optimizing serum 25-hydroxyvitamin D and maintaining zinc sufficiency through regular laboratory monitoring builds the upstream immune competence that governs episode frequency and recovery speed. Sleep architecture protection during active inflammation functions as a non-negotiable biological priority given its direct role in immune resolution. Taken together, these evidence-based throat pain remedies offer a clinically grounded, performance-compatible approach that limits downtime, protects cognitive output, and reduces the cumulative inflammatory burden linked to accelerated biological aging.
UP NEXT: Natural Solutions to Thyroid Problems
Repeated episodes of unresolved pharyngeal inflammation elevate systemic cytokine levels — particularly IL-6 — a pattern that large-scale population studies associate with accelerated biological aging and reduced healthy lifespan. WholeLiving's Biological Age Estimation Model incorporates this factor directly — your assessment takes under five minutes.
Ready to understand how these factors are influencing your biological age right now? [Take the Biological Age Assessment →]






