For executives and founders, untreated knee pain reduces gait efficiency, limits training volume, lowers daily movement, and can drive a measurable decline in VO2 max, body composition, and long-term mobility capacity. This article addresses knee therapy for pain for serious, high-performing professionals, not a general wellness audience, and treats persistent knee symptoms as a clinical threat to joint function, physical output, and healthy aging. In osteoarthritis and related knee conditions, evidence from the American Academy of Orthopaedic Surgeons, the CDC, and NIH-linked research shows that pain and reduced function can accelerate inactivity, disability risk, and broader cardiometabolic decline.
Knee Pain Reduces More Than Local Joint Comfort

Persistent knee therapy for pain belongs in a performance discussion, not a narrow symptom discussion. Chronic knee pain changes gait, reduces training tolerance, and limits total daily movement, which can lower cardiorespiratory capacity over time. The CDC identifies arthritis as a major source of pain, disability, and functional limitation, and notes that physical activity can reduce pain and improve function.
For high-performing professionals, the downstream effect is often larger than the pain itself. Lower movement volume can reduce VO2 max, increase body fat, and weaken metabolic control, especially when knee pain causes a gradual shift toward inactivity. That pattern can also impair recovery from work stress because reduced exercise capacity narrows one of the strongest nonpharmacologic tools for cardiometabolic stability.
This is why the clinical question is not simply whether the knee hurts. The more useful question is whether knee pain is lowering function, weakening physical output, and increasing long-term disability risk. A serious framework for knee therapy for pain therefore focuses on mobility, strength, load tolerance, and sustained movement capacity rather than short-term symptom masking.
Most Chronic Knee Pain Is a Load and Function Problem
Many high-demand adults assume knee pain reflects structural damage that requires rest until symptoms disappear. Current clinical guidance does not support that view as a default approach for chronic knee osteoarthritis and many nonacute knee pain presentations. The AAOS and NICE both emphasize active management, especially therapeutic exercise, as part of evidence-based care.
This distinction matters because pain and tissue state do not always match perfectly. A knee can feel painful without progressive joint collapse, and imaging findings do not always predict symptom severity or treatment response. NICE specifically notes that imaging often is not necessary for managing osteoarthritis because it may not guide nonsurgical care.
A useful model is load tolerance. When the joint, surrounding muscles, and movement patterns cannot manage current demands, pain often appears during stairs, longer walks, squatting, or prolonged sitting. Effective knee therapy for pain aims to increase the knee’s tolerance for those demands rather than removing activity altogether.
Exercise Therapy Remains the Core Intervention

The strongest nonoperative evidence supports therapeutic exercise. NICE recommends tailored exercise for all people with osteoarthritis, including local muscle strengthening and general aerobic fitness, and also advises considering supervised sessions. The AAOS guideline similarly supports exercise as a core component of nonarthroplasty knee osteoarthritis management.
That recommendation is clinically significant because exercise does more than distract from pain. It improves strength, joint control, walking ability, and confidence with movement while helping reduce pain over time. A 2024 systematic review reported that resistance training improved pain, strength, and function in knee and hip osteoarthritis.
For executives and founders, the practical value is high. Exercise-based knee therapy for pain can address symptoms while also protecting broader performance variables such as cardiovascular fitness, body composition, and work endurance. It offers a route that treats the knee and the system around the knee at the same time.
Strength Protects the Joint by Reducing Mechanical Stress

Weakness around the knee changes how force moves through the joint. When the quadriceps, gluteal muscles, and surrounding stabilizers cannot absorb and distribute load well, the knee often experiences higher stress during common tasks. The AAOS knee conditioning materials state clearly that strengthening the muscles that support the knee helps reduce stress on the joint.
This is one of the most direct reasons strength-based knee therapy for pain works. Stronger muscles improve shock absorption, reduce movement compensation, and support better alignment during walking, stair use, and rising from a chair. Those changes often improve function even before major structural change occurs inside the joint.
The effect extends beyond pain scores. Preserving lower-body strength helps maintain muscle mass, which is especially relevant after age 35 as the risk of sarcopenia rises. For a high-performing adult, stronger legs also protect mobility and make a decline in exercise capacity less likely.
Aerobic Capacity Declines When Knee Pain Limits Movement

Knee pain often starts a cycle of movement avoidance. A professional walks less, trains less, and gradually loses aerobic conditioning because everyday discomfort turns physical activity into a negotiation. Over time, this can lower VO2 max, reduce insulin sensitivity, and weaken recovery from work stress.
This is why knee therapy for pain should not be separated from cardiovascular health. The CDC notes that physical activity in adults with arthritis can reduce pain, disability, and functional limitations while also improving mental health and quality of life. When knee pain blocks movement, it removes these broader protective effects.
A therapy plan that restores walking tolerance, cycling tolerance, or other low-impact conditioning capacity does more than help the joint. It helps preserve metabolic and cardiovascular resilience. For high-demand professionals, that matters because inactivity rarely stays isolated to one body part; it often spreads into energy, sleep, and broader physiologic decline.
Sleep and Pain Amplify Each Other

Poor sleep and chronic musculoskeletal pain often reinforce one another. NIH-linked reviews report that poor sleep is associated with greater pain and inflammation, while behavioral sleep interventions can improve outcomes in people with arthritis and joint pain. This creates a clinically relevant loop in which pain disrupts sleep and poor sleep heightens pain sensitivity.
That loop has direct performance consequences. Poor sleep can impair attention, emotional regulation, pain tolerance, and recovery from exercise, all of which make rehabilitation harder to sustain. It can also increase perceived effort during movement, which makes already painful activity feel even less tolerable.
For this reason, effective knee therapy for pain often requires attention to sleep quality as a parallel variable rather than an unrelated lifestyle concern. When sleep improves, pain modulation often improves with it, and the person may tolerate rehabilitation and physical activity more consistently. That matters for professionals whose schedules already compress recovery time.
READ ALSO: Chronic Lower Abdominal Pain as a Diagnostic Signal for Executive Metabolic and Visceral Decline
Inflammation Matters, but Function Still Leads the Strategy
Inflammation plays a role in many knee pain states, especially osteoarthritis. Inflammatory processes can contribute to pain, swelling, stiffness, and reduced joint function, and chronic pain itself can maintain a state of physiologic stress. Research on osteoarthritis continues to examine inflammatory pathways as part of disease burden and symptom persistence.
Even so, the evidence does not support building all treatment around passive inflammation reduction alone. NICE advises that manual therapy should only be considered alongside therapeutic exercise and notes there is not enough evidence to support manual therapy alone for osteoarthritis management. That is a useful reminder that symptoms may improve most when therapy restores function rather than when it only targets temporary relief.
A clinically sound knee therapy for pain therefore treats inflammation as one part of a larger system. The key targets remain load management, strength, mobility, and activity tolerance. In other words, therapy should reduce symptom burden while also rebuilding the capacity that keeps symptoms from returning under normal professional and physical demands.
READ ALSO: Choosing the Right Mattress for Back Pain: Enhancing Sleep Quality and Long-Term Spinal Health
Passive Therapies Have a Supporting Role, Not the Main Role

Many adults seek passive treatments first because they appear efficient. Soft tissue work, manual therapy, braces, or short-term symptom relief can have value in selected cases, especially when they help a patient re-engage with movement. The problem arises when passive care replaces the active work that improves long-term function.
NICE addresses this directly by stating that manual therapy may be considered for hip or knee osteoarthritis only alongside therapeutic exercise. That wording matters because it positions passive therapy as an adjunct, not a standalone solution. The AAOS guidance takes a similar evidence-based approach by centering exercise and function in nonsurgical management.
For a high-performing audience, this distinction protects time and attention. A passive-only model can create repeated short relief without improving strength, gait, or movement confidence. A better use of care is to deploy symptom-relieving strategies in a way that supports active rehabilitation and sustained return to function.
READ ALSO: How Consistent Stretching Reduces Lumbar Pain and Restores Spinal Mobility in Sedentary Professionals
Body Weight and Metabolic Health Change Knee Loading
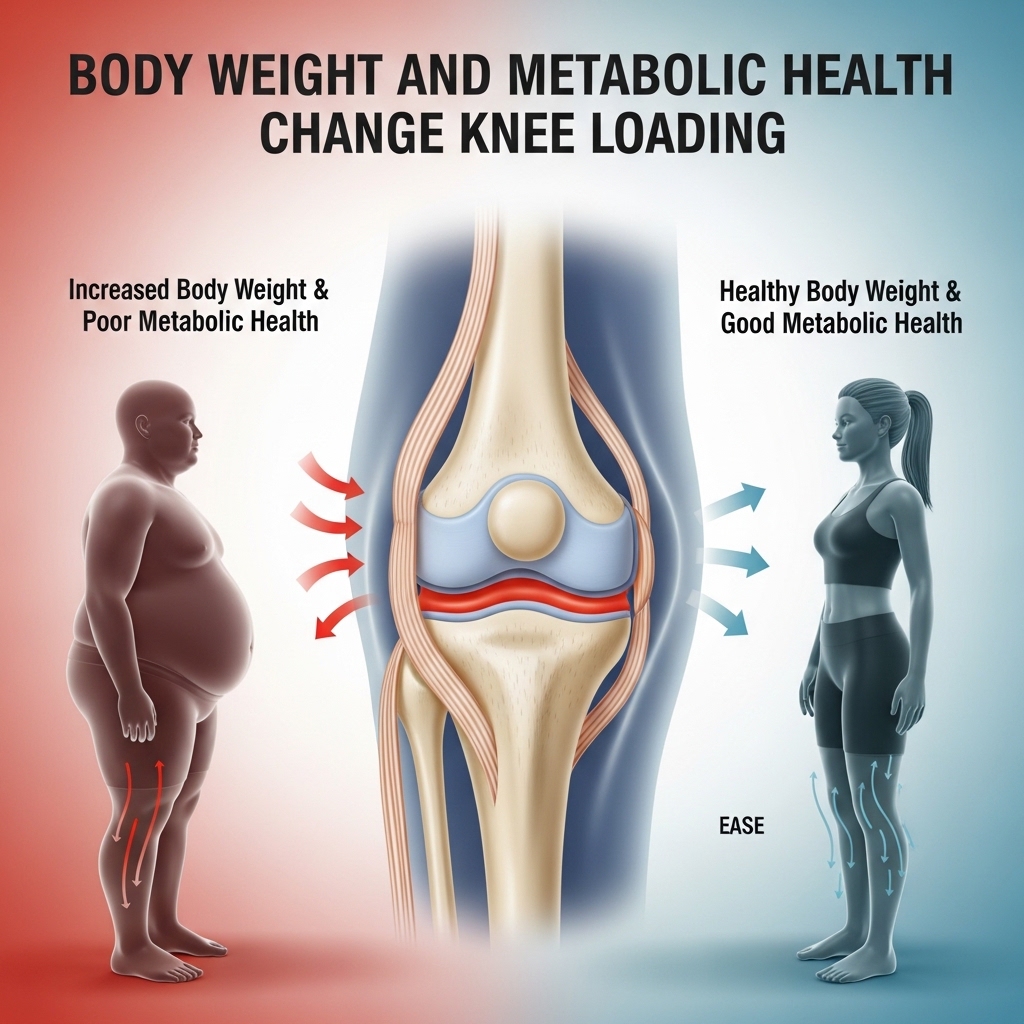
Body weight influences knee symptoms through both mechanical and metabolic pathways. Higher body mass raises load through the joint during walking and stair use, while excess adiposity can also contribute to systemic inflammatory stress. This means knee pain often reflects a broader metabolic picture rather than an isolated orthopedic event.
That connection is relevant for executives because reduced activity from knee pain can worsen body composition, and worsening body composition can then increase knee symptoms. This bidirectional pattern can accelerate decline in physical function and raise cardiometabolic risk at the same time. It also helps explain why comprehensive knee therapy for pain may need to include movement restoration, conditioning, and weight-management strategy as overlapping priorities.
The goal is not cosmetic. The goal is to lower joint stress, improve mobility, and protect long-term movement capacity. When knee symptoms improve enough to restore regular physical activity, the individual often gains benefits that extend into insulin sensitivity, endurance, and cardiovascular health.
UP NEXT: Cobra Posture: Gentle Alignment for Strength and Nourishment
How This Affects Your Biological Age
Persistent knee pain can accelerate biological age indirectly by reducing daily movement, lowering VO2 max, increasing inflammatory burden, and contributing to the muscle loss and metabolic decline that track with faster functional aging. WholeLiving's Biological Age Estimation Model incorporates this factor directly — your assessment takes under five minutes.
Ready to understand how these factors are influencing your biological age right now? [Take the Biological Age Assessment →]






